You might first notice it as a small change that is easy to explain away. Your dog hangs back on the walk, takes longer to stand, or skips the jump into the car that used to be effortless. Some dogs still look cheerful and keen, but their movement tells a quieter story.
It is tempting to think these moments are simply “getting older”, or that a limp must mean a short-term knock. In practice, muscles, bones and joints rarely operate in isolation. A mild strain can shift how a dog carries themselves, which can then load a joint differently. Long-running joint discomfort can also show up as stiffness, reluctance, or shorter strides, rather than obvious limping.1, 2
Musculoskeletal health matters because it shapes almost everything your dog does, from play and exercise to balance, toileting, and settling comfortably at home. The good news is that many problems are manageable, especially when you spot the pattern early and work with your vet on a plan that suits your dog’s age, breed, body condition and lifestyle.3, 4
Common muscular issues in dogs
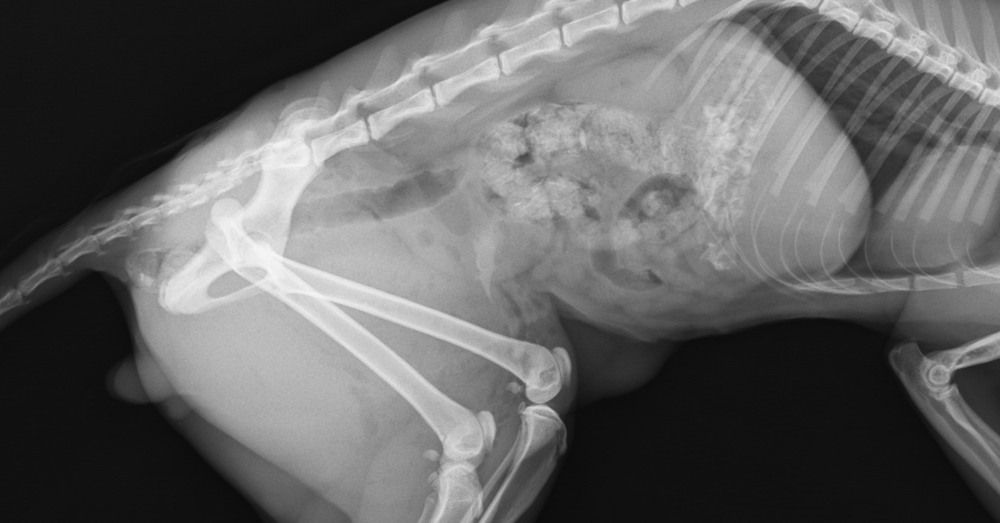
Muscle strains and soft-tissue sprains are common, particularly in dogs that launch into high-speed play without much conditioning. The tricky part is that dogs often compensate well at first. A slight hitch in the gait, a shortened step, or choosing to sit rather than stand can be the only early hints.
A useful distinction is that a muscle strain involves overstretching or tearing of muscle fibres, while a sprain affects ligaments around a joint. Either can follow a slip on tiles, an awkward landing, rough play, or sudden bursts from a cold start.
Signs you might notice at home include:
- stiffness after rest or the next morning
- tenderness when you touch a particular area (some dogs will simply move away)
- limping that improves as they “warm up”, or returns after exercise
- reluctance to run, climb stairs, or jump up
If the issue is mild, vets often start with rest and controlled activity, alongside pain relief if needed. It is important not to improvise with human medicines. Even common drugs can be unsafe for dogs, and combining medications can create real risk.5
Bone-related problems in dogs
Bones do not usually become painful without a reason. Sometimes that reason is obvious, like a fall or collision. Other times it is more gradual, such as developmental problems during growth, or bone changes associated with disease. Your vet’s job is to work out which category your dog fits into, because the next steps look very different.
Fractures can range from small cracks to complete breaks. They typically need prompt veterinary assessment and stabilisation, which might mean a splint, bandage, pins and plates, or other surgical approaches. Even when a fracture heals well, recovery often includes a period of strict activity restriction and careful return to movement.
For longer-running concerns, vets may look beyond the limb itself. Nutritional history, growth rate, overall body condition, and breed can all matter. Imaging, usually starting with X-rays, helps show bone alignment, joint surfaces and evidence of arthritis or other changes. In more complex cases, CT or MRI may be recommended to see detail that plain X-rays cannot provide.3, 4
Joint disorders, from arthritis to hip dysplasia

Joint problems are a frequent reason dogs slow down, especially as they age. Osteoarthritis is common and can show up as stiffness, reduced range of motion, or a dog choosing softer, shorter activities. Importantly, many dogs with arthritis do not limp all the time, and some never limp at all. Instead, you see small changes in daily choices: less enthusiasm for stairs, fewer jumps, more rest breaks, or a different posture when sitting.1, 2
Hip dysplasia is a developmental condition where the hip joint does not form as well as it should. Over time, that looseness can contribute to degenerative joint disease and arthritis. Signs vary widely, and they do not always match what an X-ray shows. Some dogs show symptoms young, others later, and some cope quietly until arthritis advances.6
Management is usually multimodal, which means combining approaches rather than relying on one fix. Depending on your dog, this may include weight management, tailored exercise, environmental changes at home, physiotherapy, and medications when appropriate.3, 4
Other common causes of lameness that mimic “sore joints”
Not every limp is arthritis, and not every sore back end is the hip. One of the most common causes of hindlimb lameness is cranial cruciate ligament disease (often compared to an ACL injury in people). In dogs, it is frequently a degenerative process that progresses over time, with partial tears often worsening. You might notice difficulty rising, a “sit” that looks slightly off, a swollen knee, or lameness that comes and goes before it becomes more consistent.7
This is one reason it helps to describe patterns to your vet, rather than focusing only on a single moment of limping. Details such as “worse after rest”, “worse after big play”, or “improved then suddenly worse again” can be very informative.
Breeds prone to musculoskeletal issues

Breed does not determine destiny, but it can shape risk. Larger breeds are over-represented in conditions such as hip dysplasia and cruciate ligament disease, partly due to conformation, growth patterns, and the loads placed through joints. Some smaller breeds are more prone to certain spine and knee issues due to their body shape.
What helps most, across breeds, is focusing on the basics that are within your control: steady conditioning, a sensible approach to high-impact exercise, and keeping your dog at a healthy body condition. Even a modest amount of extra weight can change how forces travel through hips, knees, elbows and the spine, especially over years.1, 7
If you have an at-risk breed, consider these preventative habits:
- keep exercise regular and consistent, rather than occasional “big days”
- avoid rapid weight gain during growth and adulthood
- use rugs or runners on slippery floors
- book a check-up early if you see recurring stiffness or lameness
Signs and symptoms worth taking seriously
Some signs are obvious, like not using a leg. Others are subtle and easier to miss because they look like personality or age. It helps to watch your dog in ordinary moments, such as getting up from bed, turning tightly in the hallway, or stepping into the car.
Common indicators include:
- stiffness after rest, especially first thing in the morning
- limping or a shortened stride
- difficulty with stairs, jumping, or getting on and off furniture
- hesitation to play, run, or go for walks they previously enjoyed
- licking at a joint or limb, or seeming sensitive to touch in one area
If your dog is not weight-bearing, has sudden severe pain, or seems unwell alongside lameness, treat it as a prompt veterinary visit. For milder signs, it is still worth booking in sooner rather than later, because early support can prevent compensation patterns and secondary strain.2, 4
How vets diagnose muscle, bone and joint problems
A good work-up usually starts with careful observation and a hands-on examination, which may include checking joint range of motion, muscle symmetry, and specific areas of tenderness. From there, vets choose tests based on what they find and what your dog can tolerate.
Imaging is often central. X-rays are commonly used to assess bones and joints, including evidence of arthritis. When soft tissue injury is suspected, or when the picture is more complicated, advanced imaging such as CT or MRI can be helpful. For chronic pain, vets also pay close attention to how your dog behaves at home, because pain can be situational and subtle in a clinic setting.3, 4
An accurate diagnosis matters because it guides the safest, most effective plan. Rest can be right for one injury and inadequate for another. The goal is not only to reduce discomfort, but also to protect function and keep your dog moving well over the long term.
Treatment and management options that actually help

Most dogs do best with a combination of approaches. Pain management guidelines in small animal practice increasingly emphasise multimodal care, which may include medication, movement plans, physical rehabilitation, and home adjustments. The right mix depends on whether the issue is acute (like a strain) or chronic (like osteoarthritis).3, 4
Medication and safety
Anti-inflammatory medicines can be very effective when they are prescribed appropriately and monitored. They also need to be used carefully. Dogs should not be given left-over prescriptions from another pet, and owners should not adjust doses without veterinary advice. Some combinations, such as using an NSAID with a corticosteroid, can be particularly risky.5
Rehabilitation and movement
Controlled exercise is often part of recovery and long-term management. This may look like shorter, more frequent walks, avoiding sudden sprints, and introducing strength and balance work through a rehabilitation program. Hydrotherapy can be useful for some dogs because it supports the body while still allowing movement.
Home and lifestyle changes
Small changes can reduce day-to-day strain:
- non-slip surfaces where your dog turns quickly
- ramps or steps for cars and couches
- supportive bedding, especially for older dogs
- nail care and paw checks, since sore feet can alter gait
Prevention, keeping dogs comfortable over time
Prevention is rarely about perfection. It is about giving your dog a body that is prepared for the life they lead. Regular exercise that builds steady conditioning, rather than occasional bursts, helps muscles support joints. A diet that maintains a healthy body condition helps reduce load through hips, knees, elbows and the spine.1, 7
Supplements such as glucosamine, chondroitin, and omega-3 fatty acids are commonly discussed for joint support. The evidence base varies by product and condition, so it is best to treat supplements as something to review with your vet, rather than a universal solution.
If you want one practical habit that pays off, it is this: track small changes. A note on your phone about when stiffness happens, which leg looks off, and what improves or worsens it can make the veterinary visit far more productive.
Final thoughts
Musculoskeletal problems are part of life for many dogs, especially as they age, but they are not something you have to simply accept or “push through”. The aim is to keep your dog moving comfortably, with the least medication necessary, and with routines that support their body rather than challenge it.
When you notice a change, trust what you are seeing. Dogs are good at adapting, and that can make pain hard to spot. A timely check, a clear diagnosis, and a thoughtful plan can protect mobility and make daily life feel easier for your dog and for you.2, 3
References
- RSPCA Knowledgebase: I think my dog has arthritis, what can I do?
- RSPCA Pet Insurance: Arthritis in pets, what is it, and how can you help?
- WSAVA: Global Guidelines for the Recognition, Assessment and Treatment of Pain
- AAHA: 2022 Pain Management Guidelines for Dogs and Cats
- US FDA: Controlling pain and inflammation in your dog with NSAIDs
- Merck Veterinary Manual (Pet Owner): Hip dysplasia
- American College of Veterinary Surgeons: Cranial cruciate ligament disease (partial ACL injury)
- Colorado State University Veterinary Teaching Hospital: Canine cruciate ligament injury
- US FDA: What veterinarians should advise clients about pain control and NSAIDs