Most people first come across patent ductus arteriosus (PDA) in an ordinary moment, a new puppy check, a routine vaccination visit, or a comment from the vet that they can hear a murmur. The puppy might otherwise seem bright and busy, which can make the whole thing feel confusing.
It is also easy to assume that a murmur automatically means a failing heart, or that it will simply “grow out of it”. In reality, some young dogs do have harmless, short-lived murmurs, but a continuous murmur is a different pattern and is one of the classic clues for PDA.1, 2
PDA matters because it is a condition where time and decision-making change the outcome. When it is recognised early and closed appropriately, many dogs go on to live normal lives. When it is missed, the heart and lungs can be placed under avoidable strain over months or years.1, 3
Understanding patent ductus arteriosus (PDA) in dogs

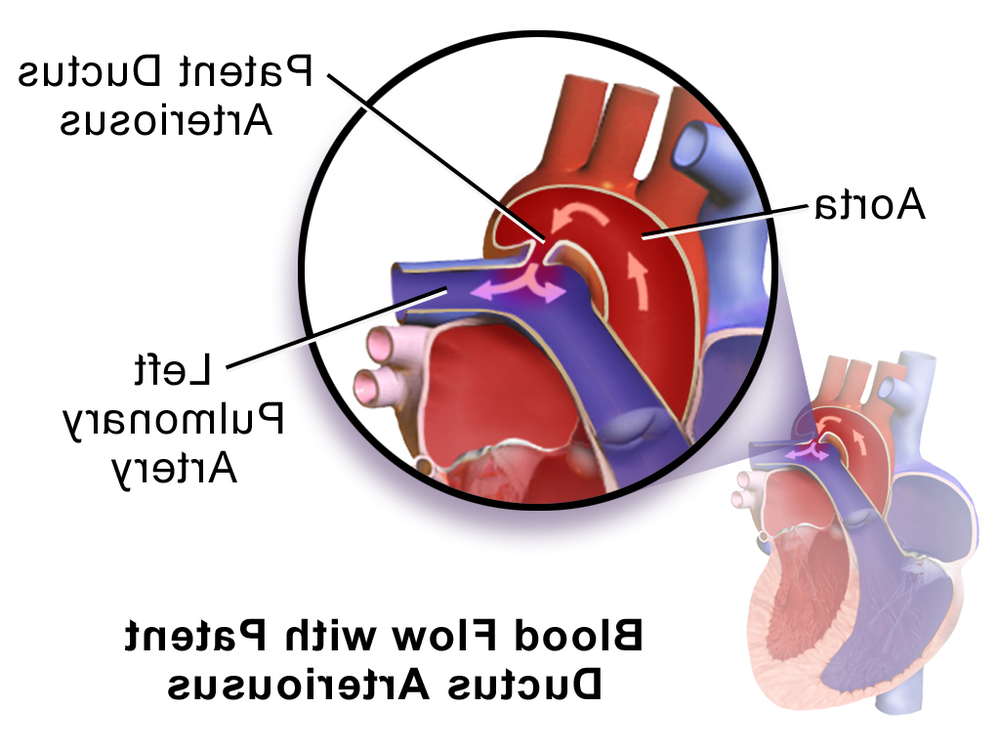
PDA is a birth defect involving a normal fetal blood vessel, the ductus arteriosus. Before birth, this vessel helps blood bypass the lungs. After a puppy takes its first breaths, the vessel is meant to close as circulation switches over to using the lungs for oxygen exchange.3, 4
When the ductus arteriosus stays open (patent), blood usually shunts from the aorta back into the pulmonary artery. This creates extra volume load for the lungs and the left side of the heart. Over time, this can lead to enlargement of the left heart chambers, fluid build-up in the lungs (congestive heart failure), and reduced exercise tolerance.1, 3
PDA is widely described as one of the most common congenital heart defects in dogs. Breed predispositions are reported, and a genetic contribution has been demonstrated in some lines (notably poodles), which is why vets often raise breeding history when PDA is diagnosed.5, 1
“Left-to-right” versus “reverse” PDA
Most PDAs are “left-to-right”, meaning blood moves from the higher-pressure aorta into the pulmonary artery. Less commonly, severe pulmonary hypertension can reverse the direction of flow (“right-to-left”, sometimes called reverse PDA). This distinction is important because closure is not always safe in reverse PDA, and the approach shifts towards careful medical management and specialist guidance.1
What you might notice at home
Many puppies with PDA look entirely well at first. Often, the first “sign” is not something an owner notices, but what a vet hears through a stethoscope at a routine visit.3
When symptoms do show up, they tend to reflect the strain on the heart and lungs. You might see:
- Getting tired quickly on walks or during play
- Coughing, especially at rest or overnight
- Fast or effortful breathing
- Poor growth compared with littermates
- In more advanced cases, signs consistent with congestive heart failure (for example, breathing difficulty and reduced stamina)
None of these signs prove PDA on their own. They are simply reasons to go back to your vet promptly, particularly if a murmur has already been mentioned.3, 1
How PDA is diagnosed
A vet will usually begin with a physical examination and careful listening. A classic PDA produces a continuous, machinery-like murmur that carries through both systole and diastole, rather than being heard only between beats.1, 2
The test that confirms PDA is an echocardiogram (cardiac ultrasound), often with Doppler to visualise abnormal blood flow. This also helps assess how much the heart has adapted (or struggled to adapt), and it helps rule out other congenital problems that can change treatment decisions.1, 3
Chest X-rays and an ECG may be used as supporting tests to look for heart enlargement, pulmonary over-circulation, or rhythm changes, but they do not replace echocardiography for a definitive diagnosis.1
A note about “innocent” murmurs
Some puppies have low-grade murmurs that resolve as they grow, and not every murmur is a congenital defect. That said, continuous or diastolic murmurs are generally considered more concerning patterns and deserve timely investigation rather than watchful waiting alone.6, 2
Treatment options, and what they involve

For the common left-to-right PDA, the goal is straightforward: close the abnormal vessel so blood no longer shunts the wrong way. In practice, the “best” method depends on a dog’s size, the duct’s anatomy, the equipment available, and the experience of the treating team.1
Catheter-based (minimally invasive) closure
Many dogs can have their PDA closed via a catheter procedure performed by a veterinary cardiologist. Devices such as the Amplatz Canine Duct Occluder are commonly used, and studies report high procedural success with relatively low complication rates, including a small risk of device embolisation (movement) and residual flow that is often trivial.7, 8
Catheter-based approaches may be limited by very small patient size or particular duct shapes, which is why some tiny dogs and many cats are still directed towards surgery instead.1
Surgical ligation
Surgical closure (ligation) via thoracotomy is a well-established option, particularly where catheter devices are not suitable. It is typically very effective when performed by an experienced surgeon, but it is more invasive and comes with the usual considerations around anaesthesia, pain control, and recovery time.1
What about medication?
Medication does not close a PDA in dogs. Medicines may be used to stabilise a dog that has gone into congestive heart failure before a procedure, or to manage cases where closure is contraindicated (such as reverse PDA), but they are not a substitute for closure in the usual left-to-right PDA.1
Aftercare and longer-term management
After closure, most dogs need a short period of restricted activity while the body adjusts to the new, more normal circulation. Your vet or cardiologist will tell you what to watch for at home (breathing rate at rest, appetite, energy, incision or catheter-site changes) and when rechecks should happen.3, 1
Follow-up echocardiography is commonly recommended to confirm closure and assess how the heart remodels over time. One of the reassuring features of successful PDA closure is that left heart enlargement often reduces, sometimes quite quickly, depending on how long the shunt has been present and how severe it was.8
If your dog was already showing signs of heart strain before treatment, your clinician may advise ongoing monitoring, and sometimes short to medium-term medication. The plan is individual, and it is normal for it to change as your dog’s heart adapts.
Prognosis, and when outcomes differ
For typical left-to-right PDA, early closure is associated with an excellent prognosis, especially when done before congestive heart failure develops. Many dogs go on to live a normal lifespan with good quality of life.1
When PDA is left untreated, the ongoing volume overload can progress to congestive heart failure, arrhythmias, and in some cases premature death. This progression is not identical for every dog, but the overall risk is high enough that timely closure is generally recommended when appropriate.1, 4
Reverse PDA sits in a different category. Because closure can worsen right-sided pressures, management needs specialist input, and the long-term outlook is more guarded.1
Breeding and early detection
If you are purchasing a puppy, it is reasonable to ask whether the litter has had a vet check that included heart auscultation, and whether there is any family history of congenital heart disease. If PDA has appeared in a line, breeders are usually advised not to repeat the mating, and affected dogs should not be bred.5
For owners, the practical takeaway is simple: keep routine puppy checks, and take murmurs seriously without panicking. A murmur is a finding, not a final diagnosis. The combination of a careful exam and an echocardiogram can turn uncertainty into a clear plan.
Final thoughts
Hearing that your puppy has a heart murmur can land heavily, mostly because it arrives without warning. PDA is one of those conditions where clear diagnosis changes everything. With the right tests, you can understand whether the murmur is likely to be harmless, or whether it points to a PDA that can be closed.
Working alongside your vet and, when needed, a veterinary cardiologist, helps you make decisions based on your dog’s anatomy and health, not on guesswork. In many cases, that steady, practical approach leads to the best possible outcome.
References
- Merck Veterinary Manual, Cardiac Shunts in Animals (Patent Ductus Arteriosus)
- Merck Veterinary Manual, Diagnosis of Heart Disease in Animals (murmur patterns)
- Cornell University College of Veterinary Medicine, Patent Ductus Arteriosus
- NCBI Bookshelf (StatPearls), Patent Ductus Arteriosus (background physiology)
- MSPCA-Angell, Patent Ductus Arteriosus and Other Causes of Continuous Murmurs
- Merck Veterinary Manual, Overview of Congenital and Inherited Cardiovascular Anomalies (innocent murmurs and red flags)
- Journal article (PubMed), Occlusion devices and approaches in canine PDA (comparison of outcomes)
- Journal article (PubMed), Retrospective analysis of Amplatz Canine Duct Occluder outcomes and complications in 200 dogs
- Journal of Veterinary Internal Medicine, Per-catheter PDA occlusion in dogs using a prototype duct occluder