You might notice it as a strange moment on a walk: your dog pauses, seems a bit flat, then carries on. Or a vet mentions an “irregular rhythm” during a routine check, even though your dog looks perfectly well. Because dogs cannot tell us what they feel, heart rhythm changes can sit in that uneasy space between “probably nothing” and “should I be worried?”
It helps to know that not every irregular beat is an emergency. Some rhythm changes are brief and harmless, while others are a clue that the heart (or something elsewhere in the body) is under strain. What matters in practice is how your dog is coping, what the rhythm problem actually is, and whether there is an underlying cause that needs attention.1
An arrhythmia is simply a heartbeat that is too fast, too slow, or uneven. The right next step is rarely guesswork. It is careful observation at home, and the right tests at the vet, so decisions about treatment are based on what is happening in your dog’s body, not just what we fear might be happening.1, 2
What a heartbeat arrhythmia means in dogs

Vets use “arrhythmia” as an umbrella term. It covers rhythms that originate from the heart’s upper chambers (atria), lower chambers (ventricles), or the conduction pathways that carry the electrical signal through the heart. Some arrhythmias are found incidentally during a check-up, others show up because a dog has fainted, collapsed, or cannot manage exercise the way they used to.1
One common misconception is that an irregular heartbeat automatically equals heart failure. In reality, arrhythmias can occur with or without structural heart disease, and they can also be triggered by problems outside the heart, such as electrolyte disturbances or systemic illness. The rhythm itself may be the main issue, or it may be a sign pointing to something else that needs treating.1
Common causes and risk factors

Arrhythmias most often develop secondary to underlying cardiac disease (for example dilated cardiomyopathy or significant valve disease), changes in the heart muscle, or abnormalities in electrical pathways. They can also be linked to low oxygen states, inflammation, drug effects, or electrolyte abnormalities, which is why vets often look well beyond the heart when they investigate an irregular rhythm.1, 3
Breed and genetics sometimes matter, not because a breed is “doomed”, but because certain conditions are more common in some lines. For example, atrial fibrillation is particularly associated with large and giant breed dogs and dogs with advanced heart disease and atrial enlargement. Ventricular arrhythmias are also recognised in some breed-associated cardiomyopathies.1, 4
Lifestyle is still part of the picture, but usually in an indirect way. Keeping a dog at a healthy weight, supporting fitness appropriate to their condition, and managing concurrent disease (such as respiratory disease) can reduce overall strain on the cardiovascular system. It is rarely as simple as “more exercise fixes it”, especially once a significant arrhythmia has been confirmed.5
Signs you might notice at home
Some dogs with arrhythmias seem completely normal between episodes. Others show subtle changes that only stand out in hindsight, such as stopping earlier on walks, choosing to lie down more, or seeming “not quite themselves” after excitement. In more significant cases, signs can include weakness, collapse, fainting (syncope), or breathing that looks laboured or faster than expected at rest.1, 5
It is worth taking fainting seriously, even if your dog bounces back quickly. Syncope can occur when a rhythm problem reduces cardiac output, sometimes intermittently, which is why a dog may appear fine at the clinic and still have a meaningful issue that needs capturing on an ECG or longer monitoring.1, 2
If your dog is struggling to breathe, has blue or very pale gums, or repeatedly collapses, treat it as urgent veterinary care. Breathing difficulty can be linked to heart disease and other emergencies, and it is not something to “watch and wait” on overnight.6
How vets confirm an arrhythmia
A physical exam and a stethoscope are a starting point, but diagnosis rests on recording the heart’s electrical activity. A standard ECG can identify many rhythm problems quickly and help determine whether the arrhythmia is coming from the atria, ventricles, or the conduction pathways.1
Because arrhythmias can be intermittent, your vet may recommend a Holter monitor (24-hour ECG). This is a wearable recorder that tracks rhythm and rate through normal daily life, with an activity diary to help match events (like exercise, sleep, or an episode of weakness) to the tracing. Holter monitoring is also used to assess treatment response and, in some cases, to check pacemaker function.2
Most work-ups also include blood tests, particularly when an extracardiac trigger is possible. An echocardiogram (ultrasound of the heart) may be recommended if structural heart disease is suspected or if the arrhythmia pattern suggests it. Chest imaging can be used when breathing signs are present or to assess the broader cardiac picture.1, 2
Types of arrhythmias you may hear about
Atrial fibrillation
Atrial fibrillation (AF) is the most common supraventricular arrhythmia in dogs. Instead of coordinated atrial contractions, the atria depolarise in a disorganised way, and the ventricular rhythm becomes irregular, often fast. AF is particularly associated with large and giant breeds and dogs with advanced cardiac disease and atrial enlargement, although “lone” AF can occur in some dogs without obvious structural disease.1, 4
Ventricular premature beats and ventricular tachycardia
Ventricular premature beats are extra beats arising from the ventricles. A few isolated beats may be incidental, but frequent or complex ventricular ectopy can be clinically important, particularly if it progresses to ventricular tachycardia (a sustained run of rapid ventricular beats). Ventricular tachycardia can reduce blood flow and lead to weakness, syncope, and in some cases may deteriorate to ventricular fibrillation, which is life-threatening.1
Bradyarrhythmias, sick sinus syndrome, and atrioventricular block
“Bradycardia” means a slower than expected heart rate, but the reason matters. Some dogs have sinus node dysfunction (often called sick sinus syndrome), where pauses, slow rates, or alternating slow and fast rhythms can lead to episodic weakness or fainting. Atrioventricular (AV) blocks occur when the electrical signal does not conduct normally from atria to ventricles. High-grade second-degree and third-degree (complete) AV block are always abnormal, and may cause collapse or syncope.3, 1
Treatment options, from monitoring to procedures
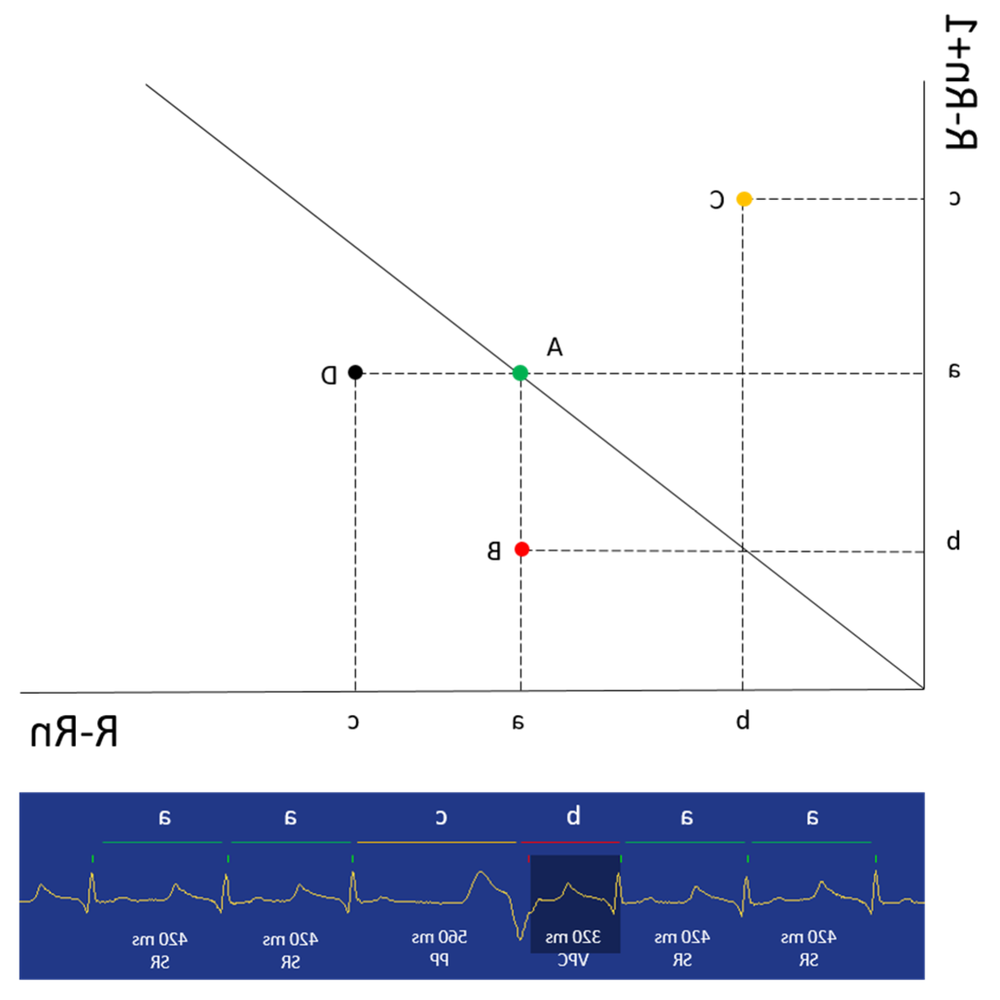
Treatment depends on two things: the rhythm problem itself, and what is driving it. Sometimes the safest plan is monitoring, especially for arrhythmias that are not causing clinical signs and are not associated with dangerous patterns on ECG or Holter. In other cases, treatment is aimed at reducing risk and improving function, rather than trying to create a perfectly “normal” rhythm at all times.1
Medications
Antiarrhythmic drugs are chosen based on the arrhythmia type, the dog’s underlying heart function, and whether the goal is rate control (slowing the heart) or rhythm control (reducing abnormal beats). For example, sotalol is commonly used for clinically significant ventricular arrhythmias in dogs, and may be combined with other agents if needed. For atrial fibrillation, drugs such as diltiazem and digoxin are often used to slow AV nodal conduction and control ventricular rate, sometimes in combination when one drug alone is insufficient.7, 8
Pacemakers
For chronic symptomatic bradyarrhythmias, particularly high-grade AV block or complete AV block, pacemaker implantation is generally the treatment of choice. A pacemaker does not “cure” the underlying disease, but it can stabilise heart rate and reduce episodes of collapse or syncope, which is often the practical goal for day-to-day quality of life.3, 1
Catheter ablation in selected cases
Some arrhythmias are driven by a discrete abnormal pathway or focus that can be treated with radiofrequency catheter ablation in specialist centres. In dogs with accessory pathways, published case series report high success rates for long-term elimination of abnormal conduction after ablation, with many dogs showing improvement when tachycardia-induced cardiomyopathy is present.9
Living with a dog who has an arrhythmia
Most owners quickly become skilled at noticing patterns: what your dog looks like after excitement, whether they recover normally after a walk, and what “usual” breathing looks like when they are asleep. Those quiet observations can be valuable clinical information, especially when episodes are intermittent and do not show up on cue at the clinic.2
Exercise is often still part of a good life, but it may need reshaping. Many dogs do best with steady, moderate activity rather than sudden bursts, overheating, or long high-intensity sessions. Your vet may advise limits based on the specific rhythm and any underlying heart disease, rather than using a one-size-fits-all rule.
Food and supplements deserve a measured approach. Heart-supportive nutrition can help overall health, but supplements are not universally “safe” or “necessary”, especially when a dog is on cardiac medications. If you are considering omega-3s or other add-ons, treat it as a vet-guided decision so doses and interactions are considered properly.7
Prevention and sensible risk management
You cannot prevent every arrhythmia, particularly those linked to inherited disease or age-related change. What you can do is reduce avoidable strain, follow up on small concerns before they become bigger ones, and keep routine care consistent. Annual check-ups, and more frequent reviews for at-risk breeds or dogs with known heart disease, improve the chance that a meaningful rhythm issue is caught before it leads to a frightening collapse at home.5
For breeders and buyers, it is worth having calm, practical conversations about known breed risks and screening. Not every arrhythmia is hereditary, but when a breed has recognised cardiac issues, thoughtful selection and veterinary guidance can reduce risk over time.
If you take one thing away, let it be this: an irregular heartbeat is information. With the right testing and follow-up, many dogs with arrhythmias can be managed well, and the plan can be adjusted as your dog’s needs change.1, 3
References
- Merck Veterinary Manual: Abnormalities of the Cardiovascular System in Animals (Arrhythmias)
- Cornell University College of Veterinary Medicine: Holter Monitoring
- Merck Veterinary Manual: Conduction Abnormalities in Dogs and Cats (AV block, sick sinus syndrome, pacemakers)
- Veterinary Sciences (2024): Risk Factors for Atrial Fibrillation in the Dog, a Systematic Review
- Sydney Animal Hospitals: Heart disease in dogs (signs and monitoring)
- RSPCA Victoria: Issues requiring medical help (difficulty breathing and other emergencies)
- Merck Veterinary Manual: Antiarrhythmics for Use in Animals
- Merck Veterinary Manual: Principles of Therapy of Cardiovascular Disease in Animals (diltiazem and digoxin use)
- Journal of Veterinary Internal Medicine (2018): Atrioventricular accessory pathways in 89 dogs, outcome after radiofrequency catheter ablation

