Sometimes it starts as a small change you cannot quite place. A dog that used to bounce at the door for a walk now hangs back. A game of fetch ends sooner. You might hear a cough at night, or notice breathing that looks a little too busy for the amount of effort.
It is easy to assume it is age, fitness, or a minor respiratory bug. The tricky part is that some heart problems can look like ordinary “slowing down” until they do not. Dilated cardiomyopathy (DCM) is one of those conditions, because it can sit quietly for a long time and then show up as tiredness, fainting, or signs of heart failure.1
DCM is not the only explanation for these signs, and many dogs with a cough have something else going on. But understanding what DCM is, who tends to get it, and how vets investigate it can make it easier to act early and make calmer decisions.
What dilated cardiomyopathy is

DCM is a disease of the heart muscle where the main pumping chambers, especially the left ventricle, become enlarged and the muscle contracts less effectively.1, 2 As the heart stretches and weakens, it can struggle to move blood forward with the usual force.
In the early stages, the body compensates. Hormones that regulate blood pressure and fluid balance help maintain circulation for a while, which is one reason DCM can be silent at first.1 Over time, that same compensation can contribute to fluid retention and congestion, which is when signs become harder to miss.
How DCM changes day-to-day function
When pumping efficiency drops, a dog may show exercise intolerance, tiring sooner on walks or needing longer recovery after play. If heart failure develops, fluid may build up in the lungs (coughing, faster breathing, breathlessness) or, less commonly, in the abdomen (a pot-bellied look that feels more like fluid than fat).1
DCM can also involve rhythm problems. Some dogs faint or suddenly seem weak because the heart is beating irregularly rather than because the muscle is failing alone.1
Causes and risk factors

DCM is best thought of as a pattern of heart muscle disease that can have different contributors. In many dogs it is considered primary (often inherited), but DCM can also be secondary to other factors, including certain medications and nutritional issues.1, 2
Breed and family tendency
Some breeds are over-represented, including Doberman Pinschers, Boxers, Great Danes, Irish Wolfhounds, Newfoundlands and others.1 Breed risk does not guarantee a dog will develop DCM, and dogs outside these breeds can still be affected.
Diet-associated DCM and taurine
Over the past decade, vets have also reported DCM in dogs without the classic breed pattern, and diet has been investigated as one possible factor. In the US, the FDA has reviewed reports of DCM in dogs eating certain foods, many labelled grain-free and often high in pulses such as peas and lentils, and sometimes potatoes.3, 4
What is known is more nuanced than most headlines. Some affected dogs have low taurine (an amino acid important in cardiac function), others have normal taurine, and some improve with a mix of veterinary treatment plus diet change (with or without supplementation).3, 4 The overall picture suggests a complex, multi-factor problem, rather than a single ingredient being “the cause”.4, 5
Signs you might notice at home

DCM does not announce itself in one neat way. Many signs overlap with lung disease, arthritis, ageing, or simple deconditioning. Still, there are a few patterns that tend to bring DCM onto a vet’s radar.1
- Reduced stamina, slowing down on walks, less interest in play
- Faster breathing at rest, or breathlessness with mild effort
- Coughing, especially at night or after lying down
- Fainting or sudden weakness episodes
- Restlessness, trouble settling, or needing to sit up to rest
- Reduced appetite or weight loss in more advanced disease
If your dog collapses, struggles to breathe, or has gums that look pale or grey, treat it as urgent and seek veterinary care immediately.
How vets diagnose DCM
Diagnosis is usually a step-by-step process, because “tired and coughy” has many possible causes. Your vet will start with history and a physical exam, including listening for murmurs, rhythm changes, and lung sounds.1
Key tests you may be offered
- Echocardiogram (heart ultrasound), this is the most definitive way to assess chamber size and pumping function for DCM.1
- Electrocardiogram (ECG) and sometimes a Holter monitor to look for rhythm disturbances that can accompany DCM.1
- Chest X-ray to check heart size and look for fluid in the lungs when heart failure is suspected.1
- Blood and urine tests to assess overall health and guide safe medication choices. In some situations, taurine testing may be considered, particularly if diet-associated DCM is on the differential list.6, 7
If diet could be a factor, it helps to bring the food bag, take photos of the ingredients panel, and note treats, chews, and any supplements. Small details can matter when a vet is trying to make sense of the whole picture.
Treatment options and what they are aiming to do
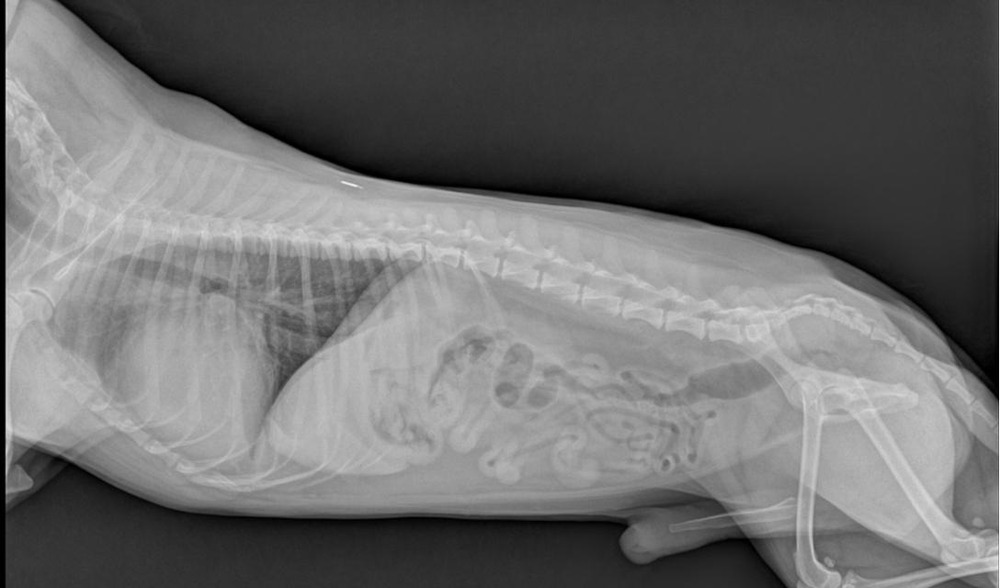
Treatment depends on whether a dog has early (occult) disease, active heart failure, significant rhythm disturbance, or a mix of these. The goal is usually not “cure”, but better function and comfort, plus slowing progression where possible.1
Common medications
Vets often use a combination of:
- Pimobendan, to help the heart pump more effectively (commonly used in canine heart failure and often used in DCM management).1
- Diuretics such as furosemide, if fluid in the lungs is present, to reduce congestion and ease breathing.1
- ACE inhibitors (for example enalapril or benazepril) and sometimes other drugs to support circulation and reduce maladaptive hormone effects.1
- Anti-arrhythmic medications if abnormal rhythms are contributing to fainting or weakness.1
If taurine deficiency is suspected or confirmed, your vet may recommend taurine supplementation alongside other treatment, and a diet change may be part of the plan in possible diet-associated cases.1, 6
Supportive care at home
Good management is often quietly practical. Keep exercise gentle and consistent, avoid sudden bursts that leave your dog winded, and focus on maintaining a lean body condition. Ask your vet what changes in breathing rate at rest should prompt a phone call, because this can be one of the earliest signs of fluid returning.
Prognosis and quality of life
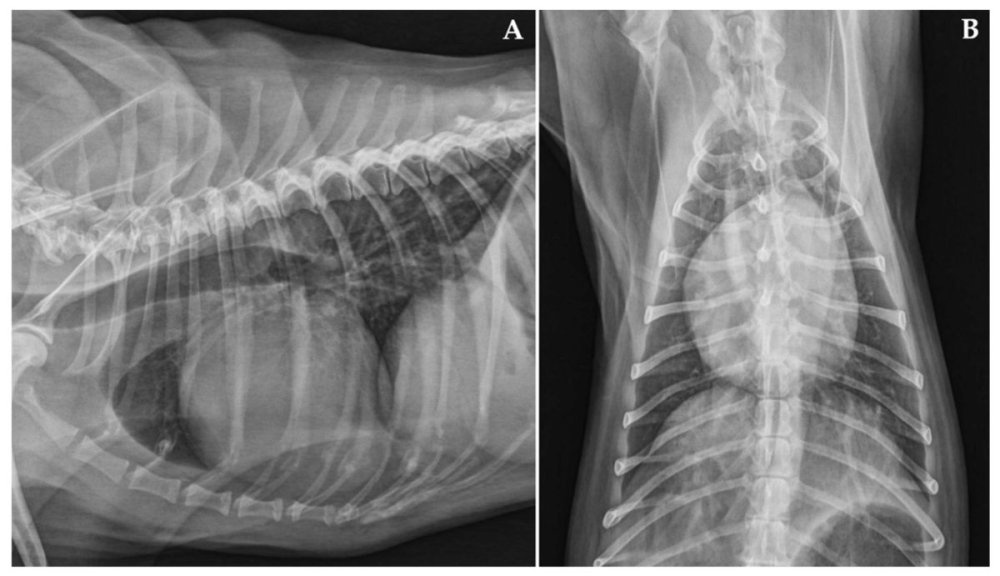
Prognosis in DCM varies widely. It is influenced by the underlying cause, whether the disease was picked up before heart failure, the presence of significant arrhythmias, and how the dog responds to treatment.1
Some dogs live comfortably for a meaningful period with well-managed medication and monitoring. Others deteriorate quickly, particularly if severe heart failure or malignant arrhythmias are present. It is also worth knowing that some dogs with suspected diet-associated DCM show improvement in heart measurements after treatment and diet change, although this is not guaranteed and does not apply to every case.3, 6
What matters day-to-day is whether your dog can still do the small things that make up a good dog life: move around the house comfortably, enjoy gentle outings, eat with interest, and rest without struggling for breath. Those are the conversations worth having regularly with your vet.
Diet, prevention, and sensible choices
There is no single prevention plan that fits every dog, but there are sensible habits that reduce avoidable risk and make problems easier to spot earlier.
Feeding decisions that stand up over time
If your dog is healthy and you are choosing a diet, look beyond marketing. Ingredient lists can be misleading, and “grain-free” is not automatically a health choice. Veterinary nutrition groups encourage looking for evidence of nutritional adequacy, quality control, and transparency from the manufacturer, and doing a brief nutrition assessment at routine visits.8
If your dog is on a grain-free, boutique, vegetarian/vegan, or home-prepared diet and DCM is suspected, do not panic-switch randomly. Bring it to your vet, because the best approach is usually a planned change to a well-established, balanced diet, and targeted testing where appropriate.4, 6
Monitoring for at-risk dogs
For breeds with known predisposition, early screening can matter, because there can be a long symptom-free phase. Your vet may suggest periodic checks, and in some dogs, referral to a veterinary cardiologist for echo and rhythm monitoring.1
Living with a dog with DCM
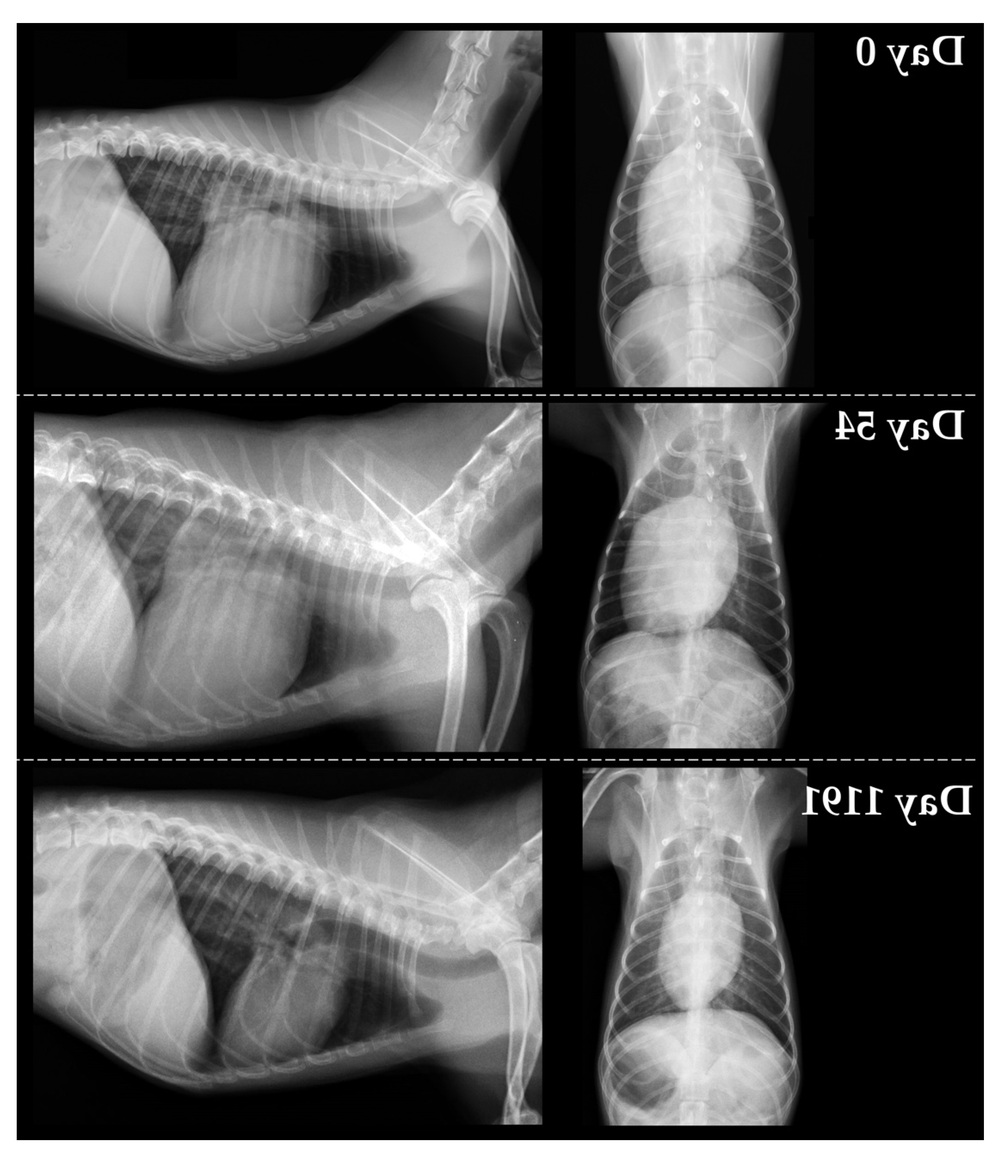
Once a dog has a DCM diagnosis, routines become the quiet backbone of care. Medication timing, repeat visits, and watching for small shifts in breathing or stamina often make more difference than any single “big” intervention.
It can help to keep a short log for a few weeks, especially when starting or adjusting medication. Note appetite, cough episodes, any fainting, and your dog’s resting breathing rate when asleep. These details give your vet something concrete to work with, and they can reduce the guesswork when things change.
Most importantly, make it easy for your dog to succeed. Choose flatter walking routes, keep play calm, avoid heat stress, and let rest be rest. Many dogs with heart disease still enjoy their world, just at a different pace.
References
- Merck Veterinary Manual: Dilated Cardiomyopathy in Dogs and Cats
- Merck Veterinary Manual: Overview of Cardiomyopathy in Dogs and Cats
- US FDA: Investigation into Potential Link between Certain Diets and Canine Dilated Cardiomyopathy
- US FDA: Vet-LIRN Update on Investigation into Dilated Cardiomyopathy
- AAHA: Diet-associated Dilated Cardiomyopathy
- University of Wisconsin School of Veterinary Medicine: Diet-Associated Cardiac Disease in Dogs (Resources and Recommendations)
- UC Davis: Taurine and Dilated Cardiomyopathy in Dogs
- WSAVA: Global Nutrition Guidelines
- ACVIM Consensus Guidelines (2019): Diagnosis and Treatment of Myxomatous Mitral Valve Disease in Dogs

