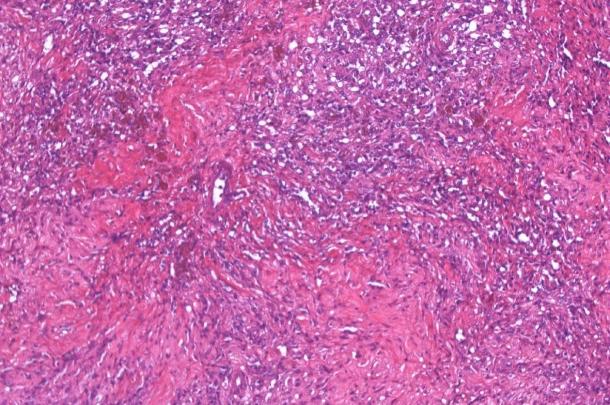
People often first hear the word “hemangiosarcoma” after something unsettling and sudden, a dog collapsing on a walk, an unexpected bout of weakness, or a vet finding fluid in the abdomen on an ultrasound. It can feel confusing because the dog may have seemed largely fine the day before, perhaps just a bit quieter, off their food, or not quite themselves.
One of the difficult things about hemangiosarcoma is that it grows from blood vessel cells and can form fragile, blood-filled tumours. When those tumours leak or rupture, the first obvious sign can be internal bleeding rather than a slow build-up of symptoms.1, 2 Understanding how it behaves helps you make sense of what vets look for, why some decisions feel time-sensitive, and what treatment can realistically offer.
Not every faint, wobble, or pale gum points to cancer, and many dogs with vague signs have far more ordinary problems. Still, haemangiosarcoma is common enough, and serious enough, that it is worth knowing the pattern, especially if you live with a large-breed, deep-chested, or older dog.2
Causes and risk factors
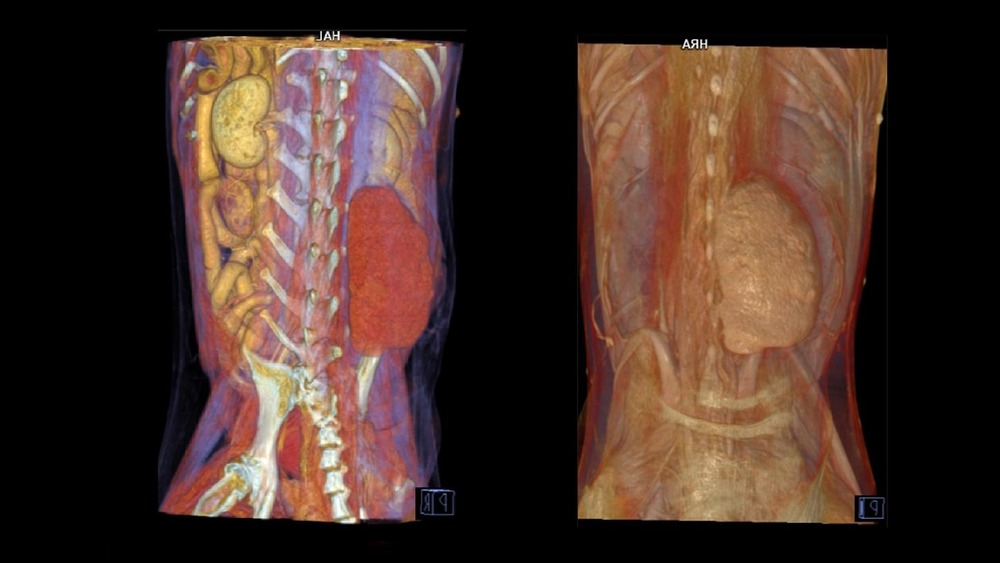
Hemangiosarcoma (often shortened to HSA) is a malignant cancer of cells associated with blood vessels. In dogs, it is most often discussed in relation to the spleen, heart (right atrium), liver, and the skin or tissues under the skin, but it can develop in other locations too.2
Breed and age patterns
We do not have a single confirmed cause, but patterns show up repeatedly. It is seen more often in middle-aged to older dogs, and it appears more commonly in some breeds, including German Shepherd Dogs, Golden Retrievers, and Labrador Retrievers, which suggests a genetic contribution.2
Environment and lifestyle, what we do and do not know
Owners sometimes worry about yard chemicals, diet, or a particular “trigger”. For visceral hemangiosarcoma (tumours in internal organs), specific environmental causes have not been clearly established in routine clinical guidance. For the skin form, UV exposure is suspected to play a role, particularly in lightly pigmented skin.2
It is still reasonable to aim for the basics that support health over a lifetime: steady weight, regular exercise suited to the dog, parasite prevention, and avoiding unnecessary exposure to harsh chemicals. Those steps cannot guarantee prevention, but they can make it easier to notice when something changes.
Symptoms and diagnosis
Hemangiosarcoma is notorious for producing signs that are vague and on-and-off, right up until a crisis. A small bleed into the abdomen can temporarily settle, then recur. A dog may look tired for a day, then appear almost normal again.2
Signs people notice at home
Some common signs reported by owners include:
- lethargy, weakness, or exercise intolerance
- reduced appetite
- pale gums
- rapid breathing, difficulty breathing, or panting at rest
- a swollen belly (from fluid or bleeding)
- collapse, especially after exertion
Dogs with tumours in the spleen or heart are at risk of rupture and sudden internal bleeding, which can be life-threatening.2 If your dog collapses, has very pale gums, or seems suddenly weak, it is appropriate to treat it as urgent and contact a vet or emergency clinic.
How vets investigate suspected hemangiosarcoma
Diagnosis is often a process of building a picture from several findings. Vets commonly start with an exam, a packed cell volume or full blood count (to assess anaemia), and imaging such as X-rays or ultrasound to look for abdominal fluid or masses.2
If internal bleeding is suspected, sampling abdominal fluid can help confirm that blood is present. For splenic masses, many dogs go to surgery because the immediate risk is bleeding and shock, and final confirmation typically comes from histopathology of the removed tissue rather than a pre-op needle sample.1, 2
Treatment options
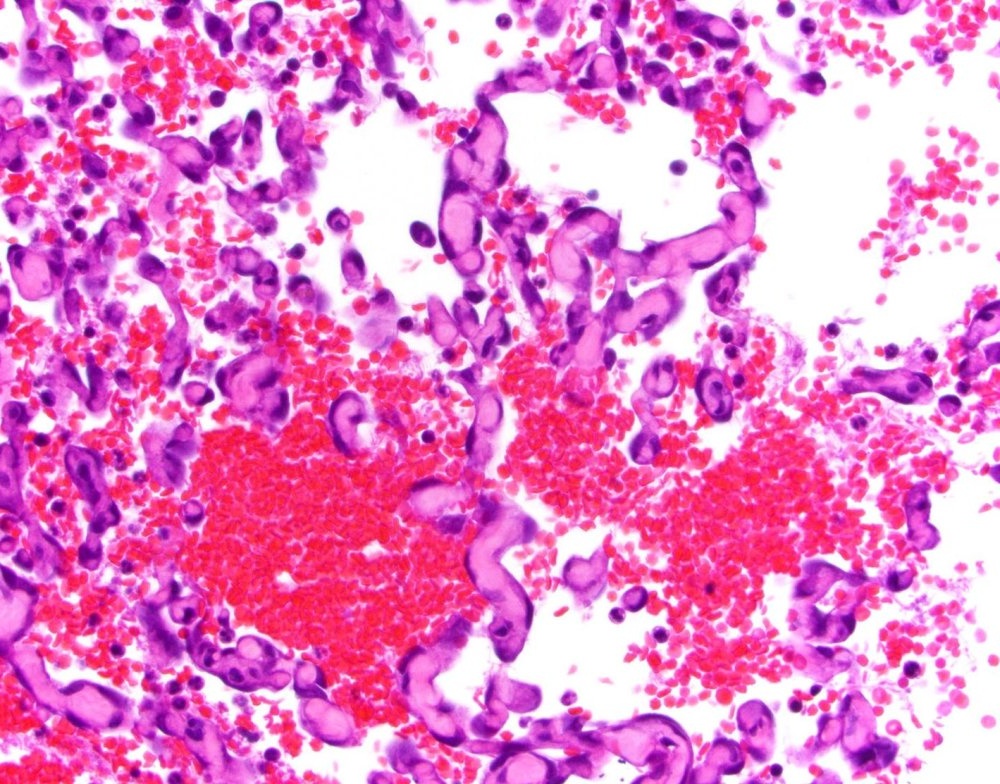
Treatment depends on the tumour’s location, whether there is evidence of spread (metastasis), and the dog’s stability at presentation. A practical way to think about treatment is that it often has two goals: stop bleeding now, and slow or delay metastasis where possible.2, 3
Surgery
For splenic tumours, splenectomy (removal of the spleen) is commonly recommended. It can remove the main tumour and reduces the immediate risk of rupture and ongoing internal bleeding.1, 2 For cardiac tumours, surgery is often not feasible, and care may focus on stabilisation and comfort, sometimes with specialist procedures depending on the case.2
Chemotherapy
Because hemangiosarcoma has a high tendency to spread, chemotherapy is often recommended after surgery, particularly for visceral disease. Doxorubicin-based protocols are commonly referenced in veterinary oncology guidance.2, 4
It helps to hold this with some nuance. Research findings vary by study design and population, but overall the intent of adjuvant chemotherapy is to delay progression rather than promise a cure. Some studies report modest median survival improvements, and timing of chemotherapy after splenectomy may matter for non-metastatic cases.5, 6
Radiation therapy and supportive care
Radiation therapy may be considered in some situations, such as incompletely removed skin tumours, or when surgery is not an option and local control could improve comfort.2, 4 Supportive care can include transfusions, IV fluids, pain relief, and management of nausea or appetite, depending on what the dog is experiencing.2
Emerging treatments and clinical trials
You may hear about immunotherapy, targeted therapies, or drug combinations being explored. Some referral hospitals run clinical trials that combine standard chemotherapy with investigational approaches. These options can be worth discussing with a veterinary oncologist, particularly if your dog is otherwise well and you have access to specialist care.7
Prognosis and survival, making sense of the numbers
Prognosis depends heavily on tumour location, clinical stage, and whether the tumour has ruptured or metastasised. In splenic hemangiosarcoma, stage is consistently associated with outcome.5
Median survival times reported in the literature for splenic hemangiosarcoma treated with splenectomy alone are often short (around weeks to a couple of months), and adjuvant chemotherapy is frequently described as extending median survival into the months rather than years, although individual outcomes vary and some dogs do better than expected.5, 8
In practice, many owners find that the hardest part is not the number itself, but the uncertainty around how a dog will feel. A useful question to ask your vet is what signs would suggest that the disease is progressing, and what can be done early to keep your dog comfortable. Quality of life is not a single moment, it is a pattern over days and weeks.
Early detection and what is realistically preventable
There is currently no guaranteed way to prevent hemangiosarcoma. For dogs at higher risk, the focus tends to be on noticing changes early, and having a plan for rapid assessment if something feels off.
What “early” can look like with HSA
Because internal tumours can be silent, “early detection” often means catching the first bleed or the first subtle decline, rather than finding a tiny tumour months in advance. If your dog is in a higher-risk group, it can help to take note of what is normal for them: resting breathing rate, gum colour, appetite, and stamina.
If you see pale gums, sudden weakness, or a distended abdomen, seek veterinary attention promptly.2
Health checks and screening conversations
Routine check-ups matter because they create context. If your vet already knows your dog’s baseline, small changes can stand out. Some owners of higher-risk breeds ask about periodic blood tests or abdominal ultrasound. The benefits and limitations of screening vary, so it is best framed as a conversation about your dog’s age, temperament, and what you would do with the information.
Living with hemangiosarcoma, day-to-day decisions
Once hemangiosarcoma is suspected or confirmed, many households shift into close observation mode. That can be draining. It helps to simplify what you are watching for, and to write it down, especially if more than one person shares care.
Practical monitoring at home
Your vet may tailor advice, but common things to monitor include:
- energy and willingness to move around
- appetite and drinking
- resting breathing effort
- gum colour
- abdominal swelling
- pain signs and sleep quality
If a splenic tumour is suspected and surgery is pending, strict rest is often advised because rupture and bleeding are major risks. Guidance may also include avoiding medications that increase bleeding risk unless specifically prescribed.1
Support for owners and caregivers
It is normal to need extra support, whether that is help with transport, keeping routine steady, or talking through decisions with a vet you trust. If you are referred to an oncologist, bring a list of questions, including expected side effects, what “good days” tend to look like, and what you should do if your dog suddenly collapses again.
Final thoughts
Hemangiosarcoma asks a lot of owners because it often arrives without a clear build-up, and because even good treatment is usually about buying time and preserving comfort rather than promising certainty. Still, there is meaning in understanding the pattern. It helps you notice small changes sooner, advocate clearly at the vet, and make decisions that fit your dog and your household.
If there is one steady takeaway, it is this: trust your observations. When a dog’s gums look unusually pale, when their breathing is not right, or when they seem weak in a way that does not fit the day, those details matter, and they are worth acting on.2
References
- VCA Animal Hospitals: Vascular Tumors (Hemangioma and Hemangiosarcoma)
- Cornell University College of Veterinary Medicine: Hemangiosarcoma in Dogs
- NC State Veterinary Hospital: Hemangiosarcoma (Medical Oncology)
- Merck Veterinary Manual: Hemangiosarcoma in Animals
- PubMed: Survival time of dogs with splenic hemangiosarcoma treated by splenectomy with or without adjuvant chemotherapy (208 cases)
- PubMed: Timely adjuvant chemotherapy improves outcome in dogs with non-metastatic splenic hemangiosarcoma undergoing splenectomy
- The Animal Medical Center (NYC): Combination Chemotherapy and Immunotherapy for Dogs with Splenic Hemangiosarcoma (Clinical Trial)
- PubMed: Does thalidomide prolong survival in dogs with splenic haemangiosarcoma?
- MDPI Veterinary Sciences: Doxorubicin–Cyclophosphamide Protocol in Dogs with Splenic Haemangiosarcoma and Haemoabdomen