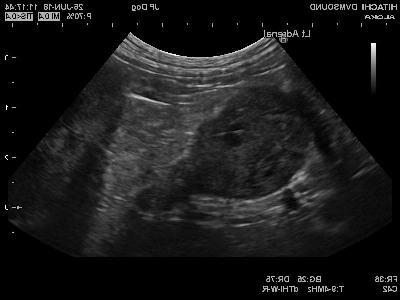
Most people do not start by wondering about a dog’s adrenal glands. They start with a dog who seems a bit different: drinking more, asking to go out overnight, panting when they never used to, or slowly losing muscle despite eating well. Because the changes can be gradual, it is easy to put them down to ageing, stress, or a run of minor issues that will settle.
The tricky part is that the adrenal glands sit at the crossroads of several hormone systems. When a tumour forms there, it can affect the body in two ways: by releasing hormones that push the body out of balance, or by growing into nearby structures and causing physical complications. Some dogs show obvious signs. Others look mostly fine until a scan for something else reveals an adrenal mass.
If you have noticed persistent changes, the practical aim is not to diagnose your dog at home. It is to recognise patterns that are worth a closer veterinary look, and to understand what tests and treatment options your vet or a specialist may raise.
Understanding adrenal gland tumours in dogs

The adrenal glands are small organs near the kidneys. They produce hormones that help regulate stress responses, metabolism, blood pressure, and salt and water balance. A tumour in or near an adrenal gland is not always cancer, but it is always something to take seriously because the adrenal glands influence so many body systems.
In dogs, the adrenal tumours vets most often worry about include:
- Adrenocortical tumours (arising from the outer cortex of the gland), which may be benign or malignant and may produce excess cortisol, leading to Cushing’s syndrome (hyperadrenocorticism).6, 7
- Pheochromocytomas (arising from the inner medulla of the gland), which can release adrenaline-like hormones (catecholamines) and are often difficult to diagnose because signs may be intermittent.1, 3
It is also worth knowing that an “adrenal mass” on ultrasound can represent several possibilities. Sorting out what it is usually requires a combination of history, lab tests, imaging, and sometimes tissue diagnosis, rather than a single definitive test.
What you might notice at home

Signs vary depending on whether the tumour is producing hormones, pressing on nearby structures, or both. Many signs are also shared with far more common conditions, which is why vets tend to think in patterns over time, not single symptoms.
Changes that commonly prompt a vet visit include:
- Increased thirst and urination (often noticed as a heavier water bowl or overnight toileting)
- Increased appetite, panting, or reduced stamina
- Hair thinning, recurrent skin infections, or slower coat regrowth after clipping
- Muscle loss, weakness, or a pot-bellied appearance that develops gradually
These are classic features of Cushing’s syndrome, which can be caused by an adrenal tumour but is more commonly caused by pituitary-driven disease. That distinction matters, because it changes treatment choices and prognosis.6, 7
Signs that can fit pheochromocytoma
Pheochromocytomas can be particularly slippery. Some dogs have few obvious signs until a scan detects the mass. Others have episodes that come and go, which may reflect intermittent hormone release. Vets may consider pheochromocytoma when there is unexplained or difficult-to-control high blood pressure, a fast heart rate, collapse episodes, or restlessness, especially in an older dog.1, 3
When it is urgent
Seek prompt veterinary assessment if your dog collapses, shows sudden weakness, has repeated vomiting, seems acutely unwell, or if your vet is concerned about severe hypertension. Some adrenal-related emergencies can deteriorate quickly and need stabilisation before any further decision-making.1
How vets confirm what is going on
Diagnosis usually happens in layers. Your vet starts with what can be learned safely and quickly, then escalates to more specialised tests when an adrenal problem becomes more likely.
Common steps include:
- Blood and urine tests to look for patterns consistent with hormone imbalance and to assess organ function before imaging or anaesthesia
- Blood pressure measurement, particularly when pheochromocytoma is a possibility1, 3
- Abdominal ultrasound to identify an adrenal mass and look for clues about local invasion
- CT (or MRI) imaging when surgery is being considered, especially to check involvement of major vessels and plan the safest approach3
- Staging tests (such as chest imaging) to check for spread, depending on tumour type and findings3
Why specialists are often involved
Adrenal tumours sit close to major blood vessels. If surgery is on the table, referral to a specialist surgical team is common. Likewise, internal medicine specialists can be helpful for complex hormone testing and for managing complications like hypertension, clot risk, diabetes, or infections that sometimes accompany adrenal hormone disorders.7
Treatment options, and what they look like in real life

Treatment depends on the tumour type, whether it is functional (hormone-secreting), the presence of spread, and whether the mass involves nearby vessels. The best plan is often a blend of tumour control and symptom management, rather than a single “cure” step.
Surgery (adrenalectomy)
When a tumour is localised and surgically accessible, removing the affected adrenal gland can be the most direct treatment. However, adrenal surgery can carry higher risk than many other abdominal procedures because of the gland’s location and, in pheochromocytoma, the cardiovascular effects of catecholamines.1, 3
For pheochromocytoma, vets often use pre-operative medications to reduce blood pressure swings and anaesthetic risk. Phenoxybenzamine is commonly discussed in this context, and careful monitoring is standard around the time of surgery.1, 3
Medical and non-surgical care
If surgery is not suitable, treatment may focus on controlling hormone effects, slowing tumour progression where possible, and protecting quality of life. This might include medications for hypertension or arrhythmias, and condition-specific management if Cushing’s syndrome is present.6, 7
In some cases, oncology options may be considered. Your vet will usually frame these choices around expected benefit, side effects, and what monitoring is realistic for your household.
Prognosis, without false certainty
It is natural to want a simple answer about outlook, but adrenal tumours vary widely. Some dogs do very well after surgery when there is no evidence of spread. Others have tumours that are invasive, metastatic, or complicated by other diseases that limit treatment options. Pheochromocytomas, for example, can be locally invasive and may metastasise in a meaningful proportion of cases, so staging and surgical planning matter.1, 3
Recovery and ongoing monitoring
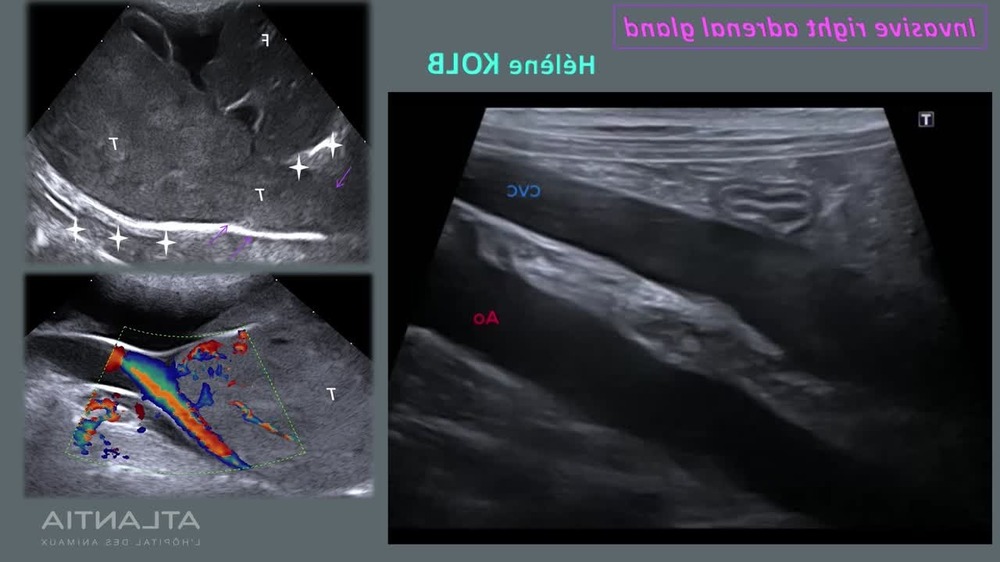
After treatment, the goal shifts to steady recovery and watching for recurrence or complications. Follow-up plans vary, but commonly include repeat blood tests, blood pressure checks, and imaging at intervals recommended by your vet or specialist.
At home, the useful focus is often simple and practical:
- Keep a brief diary of drinking, toileting, appetite, energy, and panting, especially during the first few months
- Give medications consistently, and ask about what to do if a dose is missed
- Choose gentle exercise and routine, particularly while strength returns
If your dog has been treated for Cushing’s syndrome or has ongoing hormone imbalance, your vet may also talk through longer-term monitoring and the kinds of infections or skin problems that should prompt a recheck sooner rather than later.7
Early detection and prevention, what is realistic
There is no reliable way to prevent most adrenal tumours. What does help is noticing small changes early and keeping regular veterinary check-ups as dogs age. Older dogs are more likely to develop adrenal-related disease, and many hormone conditions develop gradually enough that a pattern can be missed without routine screening.
If your dog shows signs consistent with Cushing’s syndrome, your vet may recommend specific endocrine testing. Most cases of Cushing’s in dogs are pituitary-dependent rather than adrenal-dependent, which is part of why careful diagnosis matters before treatment decisions are made.6, 7
For Australian readers, local data continues to build on which dogs are over-represented in endocrine disease groups, which can help clinicians keep a sharper index of suspicion in the right patients.2
Final thoughts
An adrenal tumour is one of those diagnoses that can sound overwhelming, partly because the adrenal glands are involved in so many systems at once. In day-to-day terms, it often begins with ordinary observations: a dog who is thirstier, softer in muscle, more pot-bellied, or just not quite themselves.
What helps most is a steady approach: document what you are seeing, bring it to your vet early, and be open to referral when imaging or surgery planning becomes complex. In many cases, the aim is safe, thoughtful decision-making, with comfort and function kept firmly at the centre.
References
- Merck Veterinary Manual (Dog Owners): Disorders of the adrenal glands in dogs
- PubMed: Patient signalment and aetiology of hypercortisolism in Australian dogs with Cushing’s syndrome
- VCA Animal Hospitals: Adrenal medulla tumours
- Merck Veterinary Manual (Professional): Pheochromocytomas in animals
- Greencross Vets: Hyperadrenocorticoidism (Cushing’s disease)
- Merck Veterinary Manual (Professional): Cushing syndrome (hyperadrenocorticism) in animals
- Australian Veterinary Association: Your pet and Cushing’s disease
- Colorado State University Veterinary Teaching Hospital: Endocrinology service (small animals)