You might notice the water bowl emptying faster than usual, or find yourself letting your dog outside more often, with bigger puddles each time. Some dogs seem hungrier but gradually lose condition. Others just feel a bit “off”, sleeping more, looking duller, picking up recurring skin or urinary infections.
Those everyday changes can be easy to explain away, hot weather, getting older, a new routine. But when the pattern sticks around, it is worth thinking about diabetes mellitus, a condition where the body cannot properly move glucose from the bloodstream into the cells that need it. In dogs, that most often comes down to not enough effective insulin to keep blood sugar in a healthy range.
Canine diabetes is serious, but it is also one of those diagnoses where calm, consistent management can make life feel very normal again for many dogs and their people. The practical goal is not perfection, it is steady control that keeps your dog comfortable and reduces complications over time.1, 2
Causes and risk factors
In dogs, diabetes mellitus is usually linked to progressive loss or dysfunction of the insulin-producing beta cells in the pancreas. The underlying trigger can be complex, and in many cases it is not possible to point to a single cause. What matters clinically is recognising the patterns that raise risk, and spotting early signs before a crisis develops.2
Some contributing factors show up repeatedly in real-world practice:
- Body weight and insulin resistance, especially when obesity is present.2, 4
- Concurrent conditions that alter hormones or metabolism, such as pancreatitis, Cushing’s disease (hyperadrenocorticism), hypothyroidism, and systemic infection.2, 3
- Medication exposure, particularly glucocorticoids (steroids) and some progestins, which can increase insulin resistance in susceptible dogs.2, 5
- Reproductive status: entire female dogs can be more prone due to hormone patterns during diestrus, and some dogs improve when desexed if hormones are a contributor.2
Breed risk is real, although it varies between studies and populations. Research in the UK has identified higher risk in some terrier breeds, among others, and many clinicians also see family lines that appear more susceptible. It is best to treat breed as a risk clue, not a prediction.2, 4
What diabetes can look like at home

The classic signs are often practical, not dramatic. Many people first notice increased thirst and urination. Hunger can increase too, and yet weight may slowly drop because glucose is not being used properly by the tissues. Coat quality can become dull, and some dogs seem less keen to exercise or play.2, 3
Some dogs are diagnosed after developing complications. Cataracts can develop relatively quickly in diabetic dogs and may be the first obvious sign that something bigger is going on. Recurrent urinary tract infections are also common, partly because glucose in the urine creates a friendlier environment for bacteria.2, 6
If you are weighing up whether it is “just a phase”, note the timeline. A single thirsty day after a beach run is one thing. A week or two of consistent changes, especially alongside weight loss or accidents indoors, is a sensible reason to book a vet visit.
Diagnosis: what your vet is looking for
Diagnosis is usually straightforward, but it needs a proper work-up. Vets typically diagnose diabetes mellitus based on persistently high blood glucose (hyperglycaemia) together with glucose in the urine (glucosuria), matched to the signs you are seeing at home.3
Additional testing helps in two important ways. First, it confirms that the high glucose is persistent rather than a one-off spike. Second, it checks for problems that can complicate management, such as infection, pancreatitis, or hormone disorders.
Depending on your dog’s situation, your vet may recommend:
- Blood and urine testing, often including ketone checks.2, 3
- A fructosamine test, which helps assess average glucose levels over the preceding weeks and can support the overall picture.3
- Urine culture, because infection can be present even when the urine sediment looks quiet.6
Treatment in practice: insulin, food, and routine
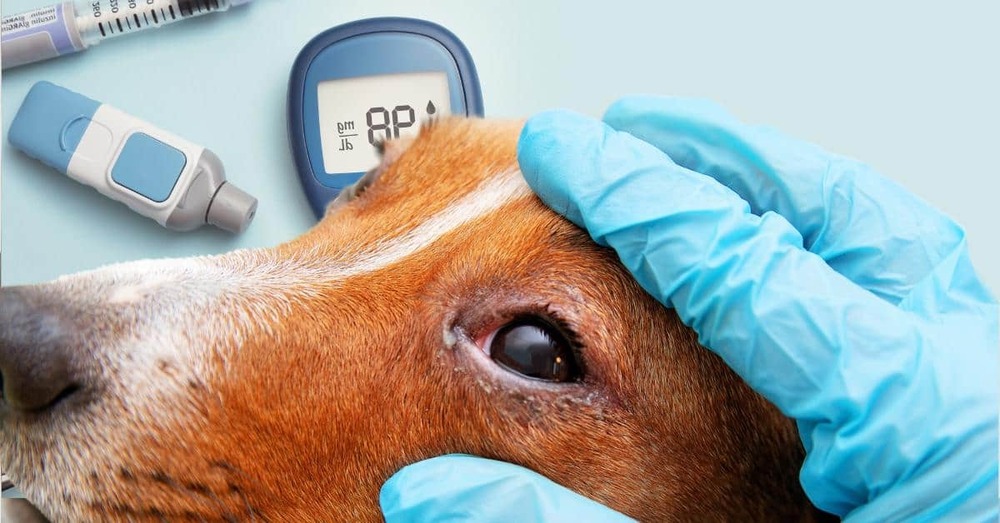
For most dogs, insulin is the foundation of treatment. The aim is to reduce clinical signs and keep glucose in a safer range while avoiding the bigger risk at home, hypoglycaemia (blood glucose dropping too low). Your vet will select an insulin type, set a starting dose, and then refine it based on response and monitoring.1, 2
Diet matters, not because there is one magical formula, but because consistent nutrition makes insulin effects more predictable. Many dogs do well on diets designed to support stable glucose curves, often with higher fibre and carefully managed carbohydrates. If weight loss is needed, it should be gradual and planned, since changing body condition can change insulin needs too.1, 6
Daily life with a diabetic dog tends to work best when it is pleasantly boring. Similar meal timing, similar walk timing, and a predictable insulin routine usually lead to smoother glucose control than constantly changing the plan “depending on the day”.1
Monitoring and the day-to-day adjustments
Monitoring is where diabetes care becomes personal to your dog. Two dogs on the same insulin and the same dose can respond quite differently, especially at the beginning. Over time, many households settle into a rhythm that includes regular check-ins and occasional dose changes, rather than constant tweaking.
Ways vets may monitor and adjust management include clinic glucose curves, home blood glucose monitoring, and periodic fructosamine testing. Home monitoring can be especially helpful for dogs that get stressed at the clinic, and it gives you a clearer sense of how your dog responds in their normal environment.1
Practical habits that usually help:
- Keep a simple log of meals, insulin doses, exercise, and any unusual signs.
- If your dog’s appetite changes, or vomiting/diarrhoea appears, treat that as a management flag and call your vet for advice before giving insulin as usual.
- Ask your vet to show you what to do if you suspect low blood sugar, including what to keep at home and when to go straight to an emergency clinic.1
Complications and when it is urgent

Not every “off day” is an emergency, but some patterns should move you from watchful to urgent. The two big concerns are hypoglycaemia (too little glucose available) and diabetic ketoacidosis (DKA), a dangerous state where the body produces ketones and becomes acidotic.
Hypoglycaemia can occur if insulin dose is too high, food intake is lower than usual, or exercise is significantly increased. Signs may include weakness, wobbliness, unusual sleepiness, tremors, or collapse. This is a situation where it is safer to treat promptly and seek guidance quickly, because severe hypoglycaemia can be life-threatening.1
DKA is an emergency. It is more likely when diabetes is poorly controlled or when another illness is present. Seek urgent veterinary care if you see vomiting, refusal to eat, marked lethargy, dehydration, rapid breathing, collapse, or a sweet, acetone-like breath smell.7, 8
Long-term outlook and quality of life
Diabetes is usually a lifelong condition for dogs, but “lifelong” does not need to mean “constantly unwell”. Many dogs return to a stable, enjoyable routine once insulin, food, and monitoring settle into place. The steadiness is often as much for the humans as it is for the dog.
Follow-up care is not just about glucose numbers. Regular reviews help your vet look for infections, dental disease, pancreatitis, hormonal problems, and changes in body condition that shift insulin needs. This is also where discussions about cataracts, vision, and comfort can happen early, rather than after a sudden change.1, 2
If you are living with a diabetic dog, the most useful mindset is practical kindness. Aim for consistent care, notice patterns, and lean on your veterinary team when something changes. That steady attention is often what keeps diabetic dogs feeling like themselves for years.
References
- American Animal Hospital Association (AAHA): 2018 Diabetes Management Guidelines for Dogs and Cats
- AAHA: Diabetes Management Guidelines overview (risk factors and clinical signs)
- Merck Veterinary Manual: Diabetes mellitus in dogs and cats (diagnosis and treatment overview)
- VetCompass study (2020): Diabetes mellitus in dogs attending UK primary-care practices: frequency, risk factors and survival
- Royal Veterinary College (VetCompass): Study summary on glucocorticoid exposure and diabetes risk in dogs (2023)
- Journal of the American Animal Hospital Association: 2018 AAHA Diabetes Management Guidelines for Dogs and Cats (full text)
- AkoVet: Diabetic ketoacidosis (DKA) in dogs, owner warning signs and urgency
- Royal Canin Academy: Canine diabetic ketoacidosis (overview and complications)

