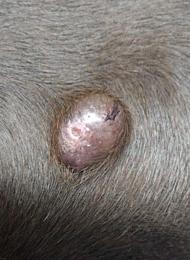
Most people do not set out to learn about mast cell tumours. They find a new bump while patting their dog, or they notice a lump that seems to change size from one day to the next. It might look like a bite, a harmless skin tag, or something your dog has had “forever”, until it suddenly feels different.
What catches many owners off guard is how ordinary these tumours can look. A mast cell tumour (often shortened to MCT) can mimic a long list of benign skin lumps, and even experienced clinicians rely on sampling cells to be sure. At the same time, some MCTs can behave in ways that make dogs unwell beyond the skin, because mast cells carry chemicals like histamine.
If you are watching a suspicious lump, or you have just heard the words “mast cell tumour” at the vet, the practical aim is simple: get an accurate diagnosis early, understand what “grade” and “stage” really mean, and choose treatment that fits your dog, your family, and the biology of that specific tumour.
Understanding mast cell tumours in dogs
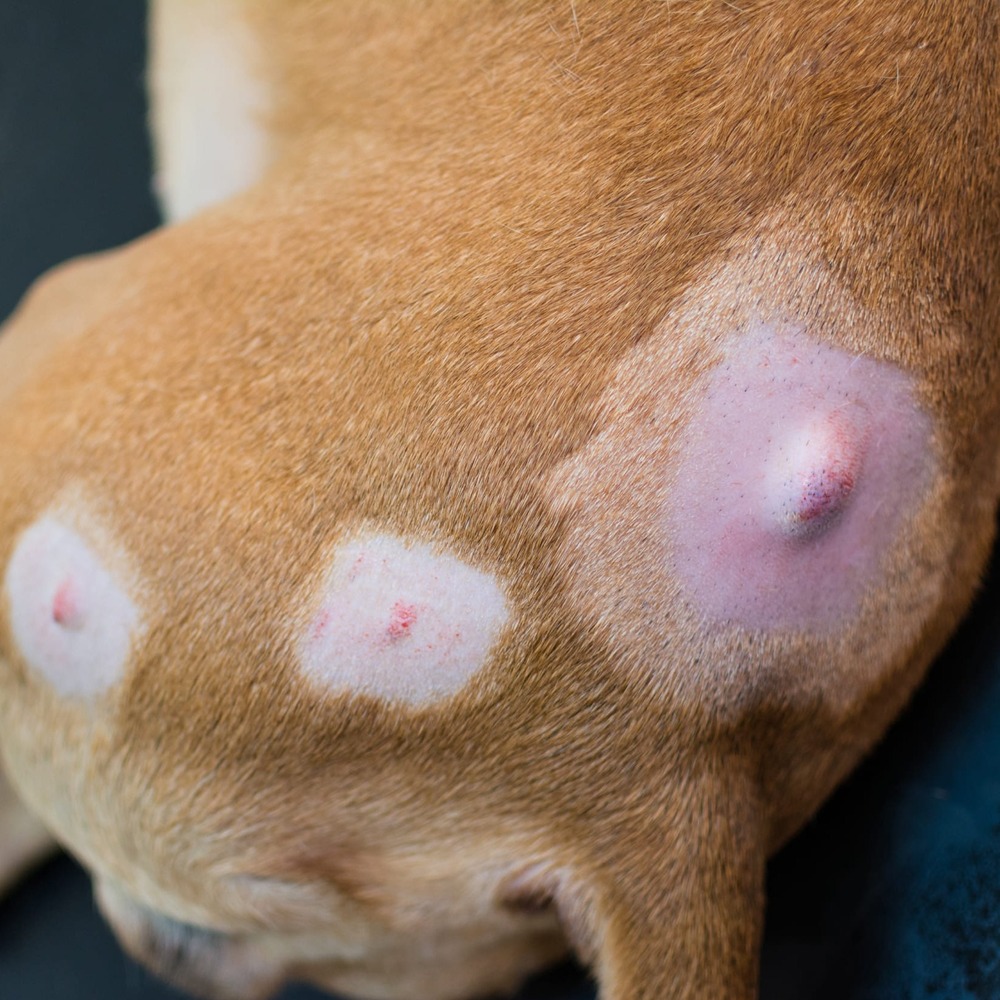
Mast cells are part of the immune system. They are involved in inflammatory and allergic responses, and they store chemical mediators such as histamine. A mast cell tumour forms when these cells become cancerous and multiply in an uncontrolled way, most commonly in the skin or the tissues just under it.1, 2
MCTs are often described as unpredictable, and that is not just a figure of speech. Some are slow growing and locally contained. Others are more invasive, more likely to recur after surgery, or more likely to spread to lymph nodes or internal organs. The reason vets take them seriously is not because every MCT is aggressive, but because you cannot tell by looking which one you are dealing with.2, 3
Breeds and patterns that show up often
Any dog can develop a mast cell tumour, but some breeds are overrepresented in clinical case loads. Boxers and Boston Terriers are commonly mentioned, along with several others including Staffordshire-type terriers, Labradors, Golden Retrievers, Beagles and Pugs.1
Breed risk can be useful as background, but it should not be treated as destiny. In day-to-day life, the more useful habit is knowing what is normal for your dog’s skin and coat, so you notice when something new appears, or when an old lump starts changing.
Causes and risk factors, what is known and what is not
Owners often ask what “caused” the tumour. For most dogs, we do not have a single clear trigger. There is evidence that genetics play a role, especially given breed predispositions. Beyond that, any discussion of environmental factors tends to be more cautious, because the science is not straightforward and risk is hard to measure in individual dogs.1
One well-established practical point is that mast cells can release histamine and other mediators when irritated, which helps explain why an MCT might suddenly swell, redden, feel itchy, or seem to wax and wane. That fluctuation can mislead people into waiting, but it is often a reason to sample the lump rather than watch it passively.2
What mast cell tumours can look like at home

The classic description is “a lump”, but that is where the certainty ends. Mast cell tumours can be small or large, soft or firm, hairless or hidden under fur, and they can appear almost anywhere on the body. They may also look like a cyst, a wart, a lipoma, or a healing wound, which is why vets often recommend sampling any new mass rather than guessing.2, 4
Some dogs also show signs that seem unrelated to the skin. Because mast cell mediators can affect the gut, a subset of dogs develop vomiting, diarrhoea, reduced appetite, or signs consistent with gastrointestinal ulceration. These signs are not specific to MCTs, but they can matter when a suspicious skin mass is present at the same time.2, 3
Book a prompt check if you notice any of the following:
- a new lump that persists beyond a week or two
- a lump that changes size quickly, especially swelling and settling repeatedly
- redness, itch, bruising, or weeping around a lump
- vomiting or diarrhoea alongside a suspicious skin mass
Diagnosis, grading, and staging
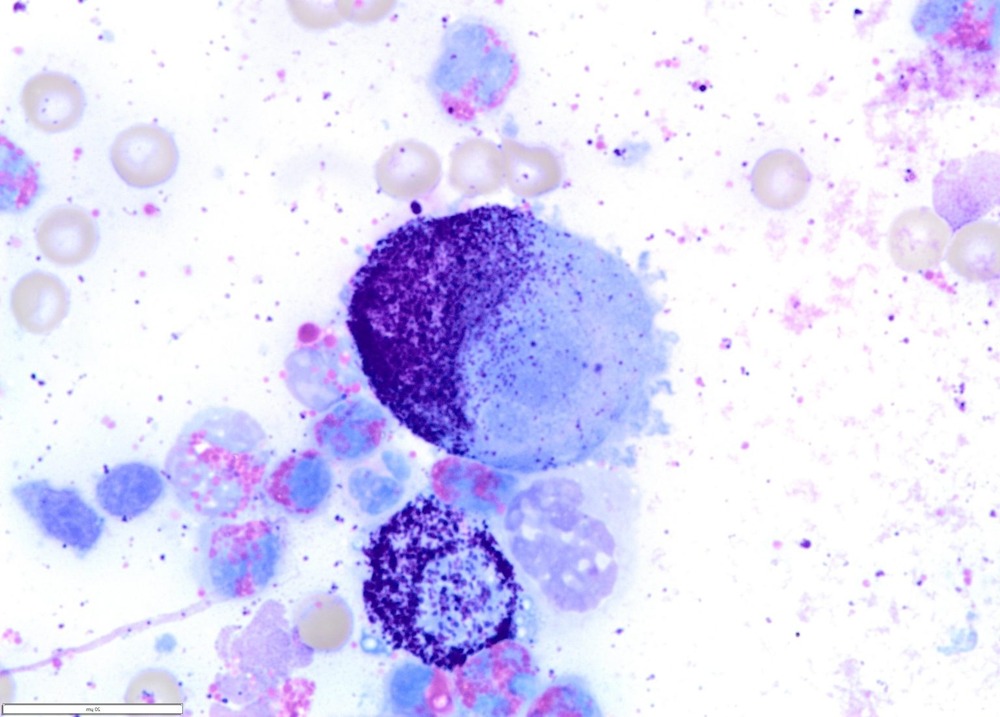
For many dogs, the first useful test is a fine needle aspirate, a quick needle sample of cells from the lump that can often be examined the same day. Mast cells have distinctive features under the microscope, so this test can provide an early direction, even though it does not always answer every question about aggressiveness.2, 4
If surgery is planned, the removed tissue is usually sent to a pathology laboratory. This is where “grading” comes in. Grade describes how the tumour cells look under the microscope, and it helps estimate likely behaviour. Two grading systems you may hear about are the Patnaik three-tier system and the Kiupel two-tier system (low grade vs high grade). The Kiupel system aims to be more objective, and many labs report one or both.5, 6
Why staging sometimes matters as much as grading
Staging is about where the tumour is and whether there is evidence of spread. Depending on the case, your vet may recommend checking nearby lymph nodes, bloodwork, and imaging such as ultrasound. The point is not to “do everything” for every dog, but to match the work-up to the tumour grade, the location, how the lump is behaving, and your dog’s overall health.2, 3
It can help to think of it this way: grade is the tumour’s nature, stage is the tumour’s reach. Both influence the treatment plan.
Treatment options
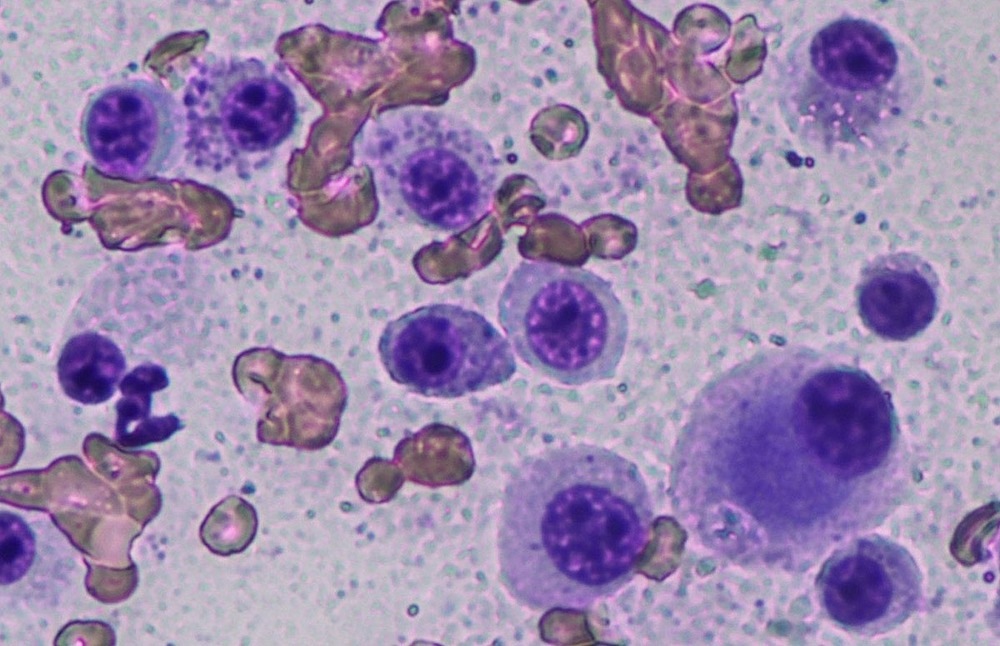
Treatment is not one-size-fits-all. The best option depends on the tumour’s location, whether wide surgical margins are achievable, the pathology report, and what is realistic for your dog and household. In many dogs, especially with low grade disease that can be fully removed, surgery is the main treatment and may be curative.1, 2
Surgery
The aim of surgery is to remove the tumour with a rim of normal tissue around it (surgical margins). Older “rules” about very wide margins are now often interpreted more flexibly, with many surgeons tailoring margins to tumour size, body site, and grade, then using the pathology report to confirm whether the excision was complete.1, 3
Where margins are incomplete, options may include a second surgery, radiotherapy for local control, or careful monitoring in selected cases. Your vet will usually discuss these decisions in the context of grade and stage, not just the margin status alone.1, 2
Radiotherapy and chemotherapy
Radiotherapy is commonly considered when a tumour cannot be widely excised, or when the pathology report indicates residual disease in an area that is difficult to re-operate on. Chemotherapy may be used for higher-risk tumours, evidence of spread, or in some cases to shrink a tumour before attempting surgery.1, 2
It is also common for vets to use supportive medications around diagnosis and treatment, particularly where there is concern about mast cell degranulation and histamine effects. The exact combination varies by case and clinician, but the rationale is well established in specialist guidance.2
Targeted and local therapies, including tigilanol tiglate
In recent years, some dogs have become candidates for local drug treatment delivered directly into the tumour. In the United States, the FDA approved tigilanol tiglate injection (Stelfonta) in November 2020 for treatment of certain non-metastatic cutaneous and eligible subcutaneous mast cell tumours, administered intratumourally by a veterinarian, with specific safety requirements and monitoring.7
It is not suitable for every lump. Case selection depends on tumour location, size, and staging, as well as the ability to manage the expected wound as the treated tumour breaks down and heals. If your dog’s tumour is in a difficult surgical site, it can be worth asking a vet or oncology service whether a local non-surgical option is appropriate in your situation.7
Prognosis, what it means in practice
Prognosis is where online information can become unhelpful, because people understandably want a simple number. The reality is more specific. A low grade, completely removed tumour in a straightforward location may never trouble a dog again. A high grade tumour, or one that has spread, needs a broader plan and closer follow-up. Grading systems exist because cell appearance under the microscope correlates with outcomes across large groups of dogs, even though individual cases still vary.5, 6
Location also matters. Tumours in areas where wide margins are hard to achieve can behave “worse” simply because local control is harder, even if the biology is not the most aggressive. This is one reason referral to a surgeon or oncologist is sometimes suggested, not because your regular vet cannot help, but because planning the first treatment well can reduce the chance of repeat procedures later.1, 2
Living with a dog after an MCT diagnosis

After diagnosis, life often becomes a little more observational. Many owners get into the habit of checking the coat during grooming or pats, and keeping a simple note of where lumps are and whether they change. That is not about becoming anxious. It is about building a calm baseline so you can spot meaningful change.
If your dog is having treatment, the day-to-day priorities are usually simple: comfort, appetite, toileting, and wound care if surgery or intratumoural therapy is used. Ask your vet what signs should prompt a call. In mast cell disease, it is reasonable to clarify what to do if you see sudden swelling around a lump, vomiting, black stools, or weakness, since those can relate to mediator release in some cases.2
Longer term, follow-up is often about catching recurrence early and watching for new tumours. Some dogs do develop additional MCTs over time, which is another reason cytology and good record-keeping are so useful in real life. It shifts decision-making from guesswork to evidence.
Final thoughts
Mast cell tumours sit in that uncomfortable space between “often manageable” and “sometimes serious”. If there is one practical takeaway, it is that a fast, minimally invasive sample of a lump can save weeks of uncertainty and can meaningfully change outcomes.
With a clear diagnosis, sensible staging when indicated, and a treatment plan that matches the tumour’s behaviour, many dogs do well. The work is not only medical. It is also about steady observation, realistic choices, and staying in close conversation with your veterinary team.
References
- American College of Veterinary Surgeons: Mast Cell Tumors
- Brisbane Veterinary Specialist Centre: Mast Cell Tumours in Dogs
- Veterinary Information Network (VIN): Current Management Recommendations for Canine Mast Cell Tumors (Proceedings)
- Southern Cross Vet: Mast Cell Tumours
- MSPCA-Angell: Tumor grading, is it applicable?
- Acta Veterinaria Scandinavica (2024): Histopathological features of subcutaneous and cutaneous mast cell tumors in dogs
- U.S. FDA (2020): FDA Approves First Intratumoral Injection to Treat Non-Metastatic Mast Cell Tumors in Dogs