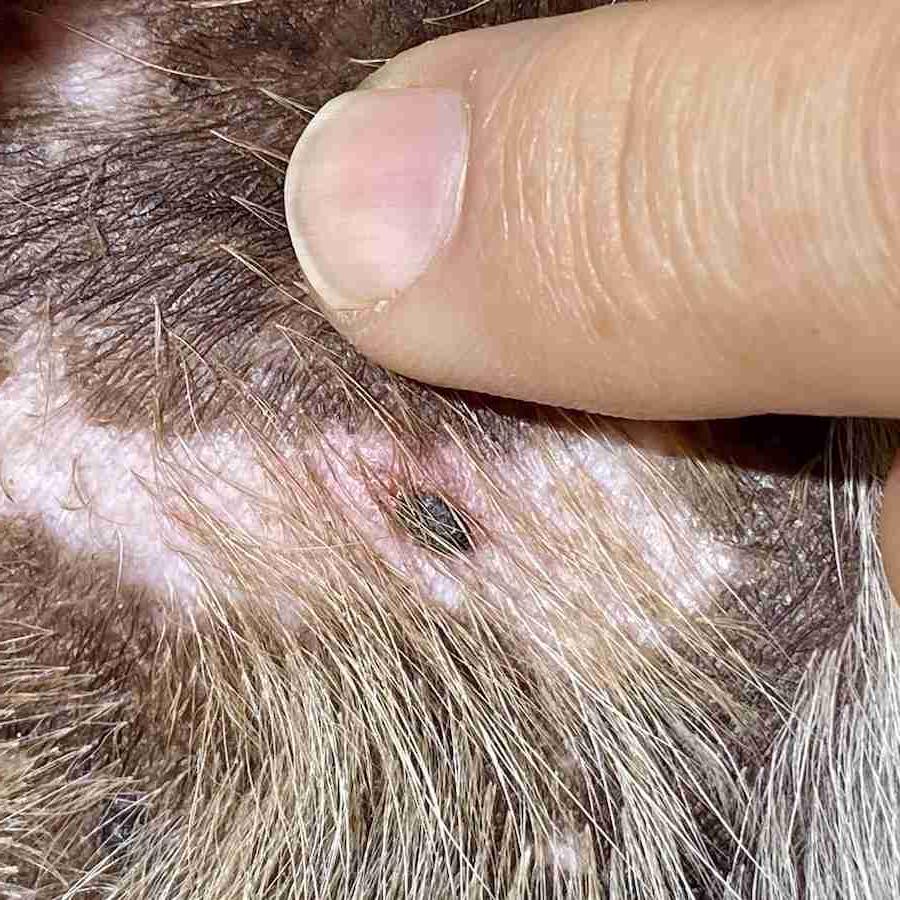
You might notice a new lump while patting your dog, or realise they are slowing down on walks in a way that does not quite fit their age. Sometimes it is a change in appetite, a smell that was not there before, or a sore that keeps reopening. These little details can be easy to explain away, especially when your dog still seems bright and keen for dinner.
Cancer is one of those diagnoses people often associate with dramatic symptoms, but in dogs it can begin quietly. Many cancers are more treatable when they are found earlier, and just as importantly, earlier veterinary advice can help you make calmer, clearer decisions about what is worth investigating and what can simply be monitored.
In Australia, cancer is common in older dogs, and the risk rises with age. Some estimates used by veterinary organisations and pet health bodies suggest around one in four dogs will develop cancer in their lifetime, and the proportion is higher in dogs over ten years of age.1 Those figures are not there to frighten you. They are a reminder that noticing change, and checking in with your vet, is part of ordinary good care.
Common types of cancer in dogs

When vets talk about canine cancer, they are talking about many different diseases that behave in different ways. Some grow slowly and stay local. Others spread early. The most practical approach for owners is to know that “cancer” is not one single story, and that a diagnosis usually starts with identifying what sort of cells are involved.
Lymphoma
Lymphoma affects the lymphatic system, which is part of the immune system. One of the more noticeable signs can be enlarged lymph nodes, often felt as firm swellings under the jaw, in front of the shoulders, or behind the knees. Lymphoma is commonly treated with chemotherapy, sometimes with very good quality of life during treatment, but the plan depends on the type and stage of disease.2, 3
Mast cell tumours
Mast cell tumours are common skin tumours in dogs. They can look like almost anything, including a small wart-like bump, a soft lump, or a sore that changes shape. They can also fluctuate, seeming to swell and settle. Because they can be unpredictable, vets often recommend sampling a suspicious lump rather than guessing by appearance alone.2
Other cancers you may hear about
Depending on your dog’s breed, age, and history, your vet might also discuss cancers such as osteosarcoma (bone cancer), haemangiosarcoma (a cancer of blood vessel cells), or oral tumours. The names are unfamiliar at first, but what matters is how they behave and what options are realistic for your dog in front of you.
Symptoms and early detection

Many of the early signs of cancer overlap with other, more common problems. A new lump can be benign. Weight loss can be caused by dental pain. Coughing might be a simple infection. What lifts a concern from “keep an eye on it” to “book in” is often a pattern: persistence, progression, or multiple changes at once.
Warning signs that are worth discussing with your vet include:
- New or changing lumps, especially those growing over weeks.
- Unexplained weight loss, or appetite changes that last more than a few days.
- Wounds or sores that do not heal normally.
- Coughing, noisy breathing, or reduced exercise tolerance that is new for your dog.
- Ongoing vomiting or diarrhoea, especially with lethargy.
- Bleeding or discharge that does not have an obvious cause.
- Changes in toileting habits, straining, or blood in urine or faeces.
These are widely used “warning sign” prompts in veterinary medicine. They are not a diagnosis, but they are a sensible reason to seek an examination.2, 4, 5
Regular check-ups help because vets can compare what they are seeing now with what they have seen before. If something needs monitoring, they can also help you define what “change” actually means, for example measuring a lump, photographing it, or setting a timeframe to recheck.
Diagnostic procedures
Diagnosis usually happens in steps. Your vet might begin with a physical exam, then recommend tests that help answer one practical question at a time, such as: is this lump inflammatory or a tumour, has the cancer spread, and is treatment likely to be tolerated?
Common diagnostic tools include:
- Fine needle aspiration, using a small needle to collect cells from a lump.
- Biopsy, taking a tissue sample to identify the tumour type and grade.
- Blood and urine tests to assess overall health and organ function.
- Imaging, such as X-rays and ultrasound, and sometimes CT or MRI, to look for masses and check for spread.
Biopsy and imaging are often the turning point between uncertainty and a real plan, because they can clarify what is treatable, what is manageable, and what is unlikely to benefit from aggressive intervention.2, 3
When a veterinary oncologist is involved
A veterinary oncologist is a specialist who focuses on cancer care. Not every dog needs an oncologist, but they can be helpful when treatment options are complex, when advanced imaging or radiation therapy is being considered, or when you want a second opinion about balancing treatment intensity with quality of life. Many oncology services work closely with your regular vet so your dog can have routine monitoring locally while receiving specialist input for the bigger decisions.
Treatment options
Treatment depends on the cancer type, stage, and where it sits in the body, and also on your dog’s age, other medical conditions, and temperament. Just as importantly, it depends on your priorities. For many families, the goal is not “do everything possible”, it is good days with minimal distress.
Surgery
Surgery can be curative for some tumours if the cancer is localised and can be removed with adequate margins. In other cases, surgery is part of a larger plan, such as removing a mass and then using other therapies to reduce the risk of recurrence.
Chemotherapy
Chemotherapy is commonly used for cancers such as lymphoma, and for some higher-grade mast cell tumours. A key difference from human oncology is that veterinary chemotherapy is often designed around quality of life. Many dogs tolerate chemotherapy reasonably well, and severe complications are uncommon but still possible, which is why monitoring and clear instructions matter.3, 6
Radiation therapy
Radiation therapy may be used when a tumour cannot be fully removed surgically, when a tumour is in a difficult location, or to help with pain control. It is typically delivered through referral centres, and your vet can talk you through whether travel and repeated visits are feasible for your household.
Targeted therapies and immunotherapies
Some cancers may be treated with targeted drugs that act on specific pathways, and there is growing interest in immunotherapy approaches. Availability varies by tumour type and location, and evidence is stronger for some treatments than others. A specialist is usually the best person to advise on what is established care versus emerging options.
Managing side effects and recovery
Side effects, when they happen, often show up as gastrointestinal upset, reduced appetite, and tiredness. Some treatments can also affect blood cell counts, which is why vets schedule follow-up blood tests during chemotherapy cycles. The aim is to spot problems early and adjust the plan before your dog feels truly unwell.6
Practical ways to support recovery at home include:
- Keep a simple daily log of appetite, energy, toileting, and any vomiting or diarrhoea.
- Ask your vet what to do if your dog skips meals, and when that becomes urgent.
- Use gentle exercise, but let your dog set the pace.
- Create a quiet rest area, particularly after procedures or treatment days.
- Know the “call the clinic” signs, including repeated vomiting, ongoing diarrhoea, marked lethargy, or any concern about fever after chemotherapy.
It also helps to remember that a dog’s experience of illness is often shaped by comfort, routine, and how manageable symptoms are. Small adjustments to pain relief, nausea control, or feeding can change the feel of a whole week.
Prevention and risk reduction
Not all cancers are preventable, and some risks, such as age and genetics, are outside anyone’s control. Still, there are sensible steps that improve general health and may reduce risk for some diseases, including certain cancers.
Healthy weight and everyday fitness
Keeping your dog at a healthy weight supports mobility, heart and lung function, and surgical safety. If you are unsure what “healthy” looks like, your vet can use a body condition score and help you set a realistic plan that does not rely on guesswork.7
Reducing exposure to smoke
Second-hand smoke exposure is not just a human health issue. Animal welfare and veterinary sources note associations between smoke exposure and health problems in pets, including cancers. If someone in the household smokes, keeping the home and car smoke-free is one of the simplest changes you can make for your dog’s long-term health.8, 9
Support for owners making decisions

A cancer diagnosis can bring a particular kind of mental load. There are appointments to schedule, results to interpret, medications to give, and decisions that can feel too big for an ordinary Tuesday night. It often helps to name the real question you are trying to answer right now, for example: “Is this curable?”, “Is treatment likely to be kind?”, or “What would comfort-focused care look like?”
If you are feeling stuck, consider asking your vet to talk through:
- Best-case and likely outcomes, not just worst-case scenarios.
- What success means for your dog, such as remission time, pain control, or stable appetite.
- Costs, travel requirements, and the time commitment of each option.
- How to recognise when your dog is coping well, and when a plan needs revisiting.
Quality-of-life discussions are a normal part of veterinary oncology. They are not about “giving up”. They are about choosing care that fits your dog and your household, and adjusting as you learn how your dog responds.
Final thoughts
Canine cancer is common enough that most owners will brush up against it at some point, either directly or through friends and family. The most helpful stance is a steady one: notice changes, seek advice early, and avoid assumptions based on how a lump or symptom looks on the outside.
With a clear diagnosis, many dogs can do very well for meaningful stretches of time, whether the plan is surgery, chemotherapy, radiation, or comfort-focused care. The thread running through good care is simple: stay observant, keep communication open with your vet, and keep your dog’s day-to-day wellbeing at the centre of each decision.
References
- American Veterinary Medical Association (AVMA): Cancer in Pets
- American Animal Hospital Association (AAHA): Signs of Cancer in Pets
- AAHA: 2026 Oncology Guidelines (Chemotherapy and side effects)
- NC State College of Veterinary Medicine: Common Warning Signs of Cancer in Pets
- The Animal Medical Center: Cancer Warning Signs in Pets
- OncoLink: Chemotherapy in Veterinary Medicine
- RSPCA Australia: 4 ways to avoid obesity in your dog
- RSPCA Knowledgebase: Is it risky to smoke or vape around companion animals?
- Cancer Council Australia: Tobacco and second-hand smoke