It is easy to notice the obvious things with dogs, a limp, an upset stomach, a sore ear. Hormone problems tend to arrive differently. A dog might just seem a bit flatter on walks, or their coat starts looking dry and sparse, or they are suddenly drinking a lot more water and asking to go outside at odd times.
Because these shifts can be gradual, people often put them down to ageing, the weather, a change in food, or “just one of those weeks”. Sometimes they are. Still, when the changes stick around, or several small changes show up together, it is worth considering whether an underlying hormonal disorder is nudging your dog’s whole system off balance.
Hormones quietly influence appetite, skin and coat, muscle tone, water balance, and the way the body handles stress. When something in that signalling goes wrong, the signs can look oddly general at first. The good news is that many endocrine conditions are very manageable once properly diagnosed, and many dogs return to a steady, comfortable routine with the right support.
Common canine hormonal disorders
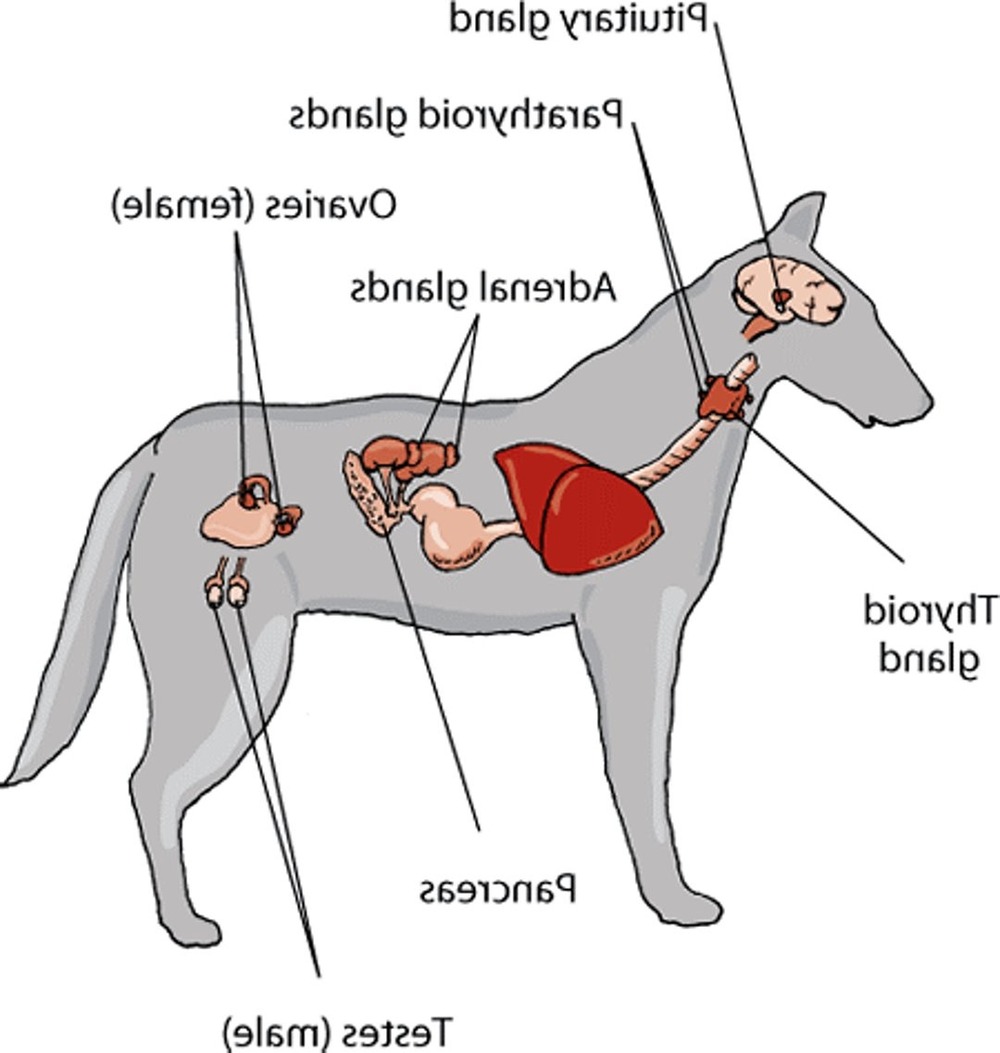
“Hormonal disorder” is a broad label. In practice, it usually means a problem with the thyroid, adrenal glands, or pancreas. Each condition has its own pattern, but there is overlap, which is why diagnosis matters more than guessing based on one symptom.
Hypothyroidism
Hypothyroidism happens when the thyroid gland does not produce enough thyroid hormone. It is often seen in middle-aged to older dogs and is more common in medium to large breeds.1
Common signs include weight gain without a clear increase in food, lethargy, and coat and skin changes (dull coat, thinning hair, recurring skin or ear infections). Signs often come on slowly, so they can be easy to miss until you look back and realise how much has changed.1
Diagnosis is based on a vet’s assessment plus blood tests, and it can be complicated by other illness or some medications that influence thyroid values.1 Treatment is usually lifelong thyroid hormone replacement (levothyroxine) with monitoring to make sure the dose is right.1
Cushing’s disease (hyperadrenocorticism)
Cushing’s is caused by the body producing too much cortisol. In dogs, the most common cause is a pituitary tumour that drives the adrenal glands to overproduce cortisol, although adrenal tumours can also be responsible.2
The signs owners notice tend to be practical, increased thirst and urination, a bigger appetite, panting, a pot-bellied appearance from muscle changes, and hair loss or thinning coat.2
Vets may use screening and diagnostic tests such as a urine cortisol:creatinine ratio, ACTH stimulation test, and low-dose dexamethasone suppression test. Imaging can help differentiate pituitary-driven disease from an adrenal tumour.2 Treatment may involve medication, and in selected cases, surgery, radiation, or other targeted approaches depending on the cause.3
Addison’s disease (hypoadrenocorticism)
Addison’s is essentially the other end of the adrenal spectrum, where the body produces too little cortisol, and in primary Addison’s, too little aldosterone as well. It can be difficult to spot because early signs can be vague and come and go, such as reduced appetite, vomiting or diarrhoea, weakness, or seeming “off” after stress.4
Diagnosis is typically confirmed with an ACTH stimulation test, and bloodwork may show characteristic electrolyte changes (especially with primary Addison’s).4
Treatment is usually very successful once established. It commonly includes lifelong glucocorticoid support and, for primary Addison’s, mineralocorticoid replacement such as DOCP injections, with regular monitoring of electrolytes.4
Diabetes mellitus
Diabetes mellitus occurs when the body cannot properly regulate blood glucose due to inadequate insulin, insulin resistance, or both. Many dogs will show increased thirst and urination, weight loss despite a good appetite, and sometimes lethargy.5, 6
For many dogs, treatment involves insulin and careful feeding routines, along with monitoring recommended by your vet. With consistent care, many diabetic dogs do well and keep enjoying their normal activities.5, 6
Why these disorders happen (and who is more at risk)
Endocrine disorders rarely have one simple cause. Sometimes there is a clear driver (such as an adrenal tumour in some cases of Cushing’s). Other times, it is more about predisposition and biology than anything an owner did “wrong”.
Age is a common thread. Hypothyroidism and Cushing’s are often diagnosed in middle-aged or older dogs, partly because changes develop over time and partly because the conditions themselves are more common in those life stages.1, 2
Breed tendencies also matter, although they are not destiny. Some breeds are over-represented in particular conditions, and your vet may keep those patterns in mind when symptoms appear. Breed is only one piece of the puzzle, and it should not replace testing.1, 4
There are also everyday factors that can muddy the picture. Stress, concurrent illness, and certain medications can affect test results or mimic endocrine signs. This is one reason vets often recommend repeat testing or a full diagnostic work-up rather than treating based on a single borderline result.1
Signs that are worth taking seriously

Hormone-related signs can look like “general unwellness”, especially early on. What often makes them stand out is persistence, or a cluster of small changes rather than one dramatic symptom.
- Thirst and urination changes (drinking more, asking to go out more, accidents in a previously housetrained dog)2, 5
- Weight gain or weight loss that does not match food intake changes1, 5
- Coat thinning, hair loss, recurrent skin or ear infections1, 2
- Reduced stamina, lethargy, muscle weakness1, 2
- Vomiting, diarrhoea, episodic weakness, or seeming worse after stress (a pattern that can fit Addison’s)4
If your dog is unwell in a sudden or severe way, for example collapse, repeated vomiting, profound weakness, or signs of dehydration, treat it as urgent and contact a vet or emergency clinic. Some endocrine crises, particularly Addisonian crisis or diabetic complications, can become serious quickly.4, 6
How vets diagnose hormonal disorders
Diagnosis usually starts with the basics, a history, a physical exam, and standard blood and urine tests. Those routine results often provide clues about what system is under strain, and they also help rule out other common causes that can look similar.
From there, endocrine testing becomes more specific. Thyroid diagnosis may involve multiple blood tests interpreted in context, because other illness and some medications can lower thyroid hormone values without true hypothyroidism.1
For Cushing’s, vets may use tests such as urine cortisol:creatinine ratio, ACTH stimulation, or low-dose dexamethasone suppression testing, and imaging can help distinguish pituitary-driven disease from an adrenal tumour.2
Addison’s is commonly confirmed with an ACTH stimulation test, and electrolyte patterns can also support suspicion, especially with primary Addison’s.4
For diabetes, diagnosis generally involves measuring blood glucose and assessing urine for glucose, then working with you on a practical plan for insulin, feeding, and monitoring.6
Treatment, what “manageable” often looks like

Treatment depends on the condition and the individual dog, but many plans share a similar rhythm: medication, monitoring, and adjustments over time.
Medication and hormone replacement
Hypothyroidism is typically treated with levothyroxine, and dogs need monitoring because the right dose is individual and can change with time, weight, and other health issues.1
Cushing’s is often managed with medication or, in some cases, surgery or other interventions. The best approach depends on whether the cause is pituitary-driven or an adrenal tumour, and on the dog’s overall health.2, 3
Addison’s treatment commonly involves ongoing glucocorticoid support, plus mineralocorticoid replacement (often DOCP) when needed, with regular electrolyte checks to keep the dog stable.4
Diabetes management usually involves insulin and consistent routines around meals and activity. Your vet will help you find a monitoring method that fits your confidence level and your dog’s temperament, then adjust the plan based on results.6
Diet and routine
Food and exercise do not “cure” endocrine disease, but they often make treatment smoother. Keeping meals predictable, avoiding unplanned treats (especially for diabetic dogs), and aiming for steady, moderate activity can help stabilise appetite, weight, and daily comfort.6
When surgery is part of the picture
Surgery is not common for every hormonal disorder, but it can be relevant in certain tumour-related cases, such as some adrenal tumours causing Cushing’s. Whether it is appropriate depends on imaging results, the dog’s surgical risk, and specialist input.3
Living with a dog who has a hormonal condition
Once treatment begins, many owners notice that life becomes less about “fixing” and more about keeping things steady. A well-managed endocrine condition often looks wonderfully ordinary: walks at the usual pace, a reliable appetite, a coat that slowly improves, and fewer odd little episodes that used to make you wonder.
It helps to track simple, real-world markers. How much water your dog is drinking, whether they are waking at night to urinate, how their coat is changing, how quickly they tire, and whether their appetite feels out of character. These observations are not overthinking. They are useful information for your vet when it comes time to adjust a dose or recheck bloods.
If your dog takes long-term medication, ask your vet what side effects to watch for, and how often monitoring is recommended. For some conditions, missing doses or stopping medication abruptly can cause a significant setback, so it is worth building a system that suits your household.1, 4
Prevention and early intervention
You cannot prevent every endocrine disorder, and it is not realistic to aim for perfect control over biology. Still, there are sensible steps that reduce risk and improve early detection.
- Keep regular vet check-ups, especially as dogs reach middle age, when gradual changes can be easier to miss at home.1, 2
- Follow through on recommended blood and urine testing when signs persist or recur. Early diagnosis often means simpler management.2, 6
- Maintain a stable routine for food and exercise, and aim for a healthy weight, which supports overall resilience even when an underlying condition is present.6
If something feels “not quite right” for more than a few days, or it keeps returning, that pattern itself is worth discussing with your vet. Hormonal disorders often reveal themselves through repetition rather than drama.
Final thoughts
Hormonal disorders can feel confusing at first because the signs are often ordinary things, drinking, eating, sleeping, coat quality, that have quietly shifted. With proper testing, most endocrine conditions can be managed in a way that brings daily life back into balance.
The most helpful mindset is calm attention: noticing patterns, following up when changes persist, and working with your vet on a plan that is realistic for your dog and your household. Small adjustments, made steadily, tend to add up to a dog who feels more like themselves again.
References
- FDA: Hypothyroidism in Dogs, signs, diagnosis, and FDA-approved levothyroxine treatment
- Merck Veterinary Manual: Cushing Disease (pituitary-dependent hyperadrenocorticism) in animals
- Merck Veterinary Manual: Cushing Syndrome (hyperadrenocorticism) in animals
- Today’s Veterinary Practice: Canine hypoadrenocorticism (Addison’s), overview, diagnosis, and treatment
- RSPCA Pet Insurance Australia: Diabetes in dogs, symptoms, diet, and treatment
- Merck Veterinary Manual: Diabetes mellitus in dogs and cats
- Veterinary Information Network: Approach to diagnosis of canine hypothyroidism (clinical considerations and testing)
- American College of Veterinary Internal Medicine: Endocrine disease information for pet owners

