It often starts with something small that feels easy to explain away. A dog who hesitates at the stairs. A jump onto the couch that suddenly looks awkward. A stiff neck after play that does not quite settle by the next morning.
Because dogs can be so good at pushing through discomfort, it is common for spinal trouble to be missed early. Some problems come on dramatically, but many begin as quiet changes in movement that look like ageing, soreness, or a “bad landing”.
Spinal disorders matter because the spine is not just bones. It also protects the spinal cord and nerves, and when those structures are irritated or compressed, the effects can range from pain to weakness, wobbliness, and in severe cases, loss of bladder control or paralysis. Recognising what is normal for your dog, and what is new, is often the most useful first step.
Common causes of spinal disorders in dogs
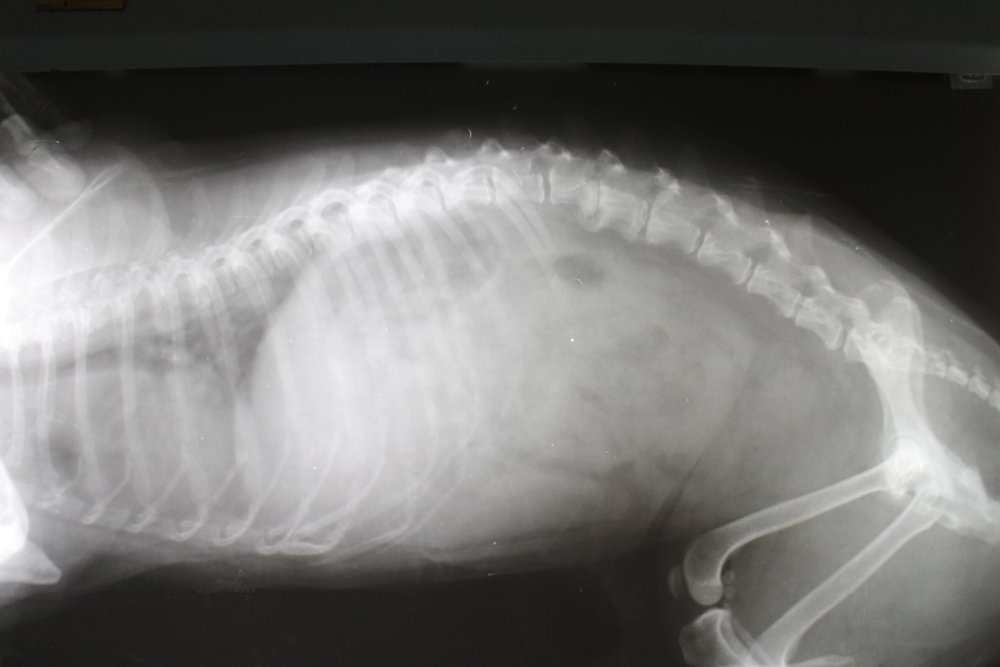
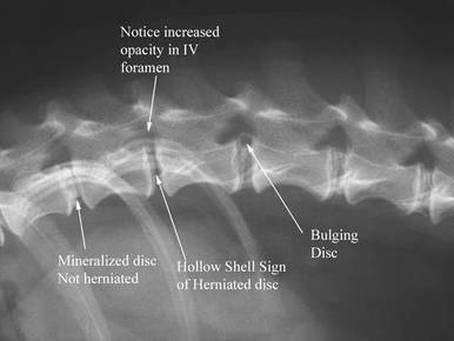
“Spinal disorder” is a broad label. It can mean a problem with the bones of the spine, the discs that sit between vertebrae, the joints and ligaments that stabilise the back, or the spinal cord itself. In everyday practice, one of the most common culprits vets see is intervertebral disc disease (IVDD), where disc material presses on or concusses the spinal cord. 1
Breed shape, genetics, and risk
Some body types carry a higher risk of disc degeneration and disc herniation, particularly the so-called chondrodystrophic breeds (dogs with shortened legs and specific cartilage growth patterns). Dachshunds are the best-known example, but they are not the only ones. The point is not that these dogs are “fragile”, it is that their discs can change earlier in life, which can make back injuries more likely from everyday movements. 1, 2
Injury and sudden overload
Trauma matters, but it is not always dramatic. A slip on tiles, a twist while chasing a ball, or landing awkwardly off furniture can be enough to tip a vulnerable disc into trouble. In some cases, high-velocity activity or severe trauma can injure the spinal cord even with minimal ongoing compression. 1
Degenerative and age-related change
Older dogs can develop slower, progressive disc bulging and arthritic change around the spine. These cases may be less obvious at first, with a gradual loss of comfort and flexibility rather than a sudden collapse. It is one reason vets take “moving differently” seriously, even when a dog is still keen to eat, play, and go for walks. 1
What to notice at home, and when it is urgent
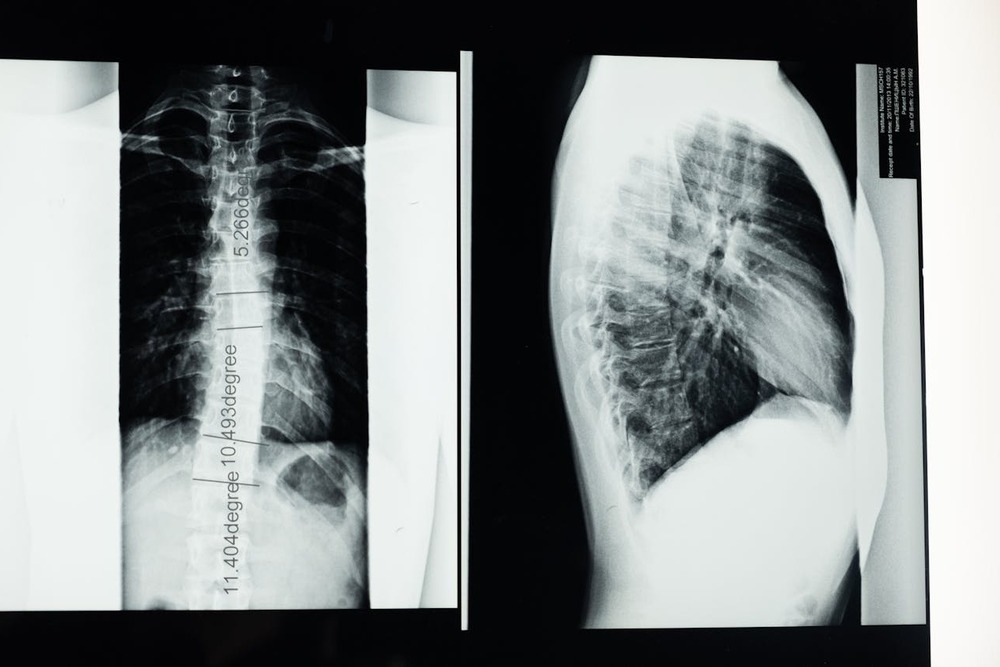
Spinal problems do not always announce themselves with obvious limping. Often, what you see is a dog making small adjustments to protect a painful area. That can look like slowing down, changing posture, or avoiding particular movements.
Common signs worth taking seriously include:
- Reluctance to jump (onto the couch, into the car) or hesitation on stairs
- Back or neck pain, including yelping when picked up, or tensing when touched
- Stiffness, a hunched back, or a lowered head and guarded neck
- Wobbliness, knuckling over on the paws, dragging toes, or scuff marks on nails
- Weakness in the back legs, difficulty standing, or collapsing
- Loss of bladder or bowel control, or inability to urinate normally
If your dog suddenly cannot walk, seems rapidly weaker, or loses bladder control, treat it as an urgent veterinary situation. Early assessment can make a real difference to outcome. 3, 4
How vets diagnose spinal disorders
A good diagnosis usually starts with a careful history and a neurological exam. Vets are not only looking for pain, they are also mapping which limbs are affected, checking reflexes, and working out where along the spine the problem might be. That “where” matters because it shapes the next steps.
Imaging choices depend on what your vet suspects, how unwell your dog is, and what is available locally. In suspected disc disease or spinal cord compression, advanced imaging is often needed to properly understand what is happening.
X-rays versus CT, MRI, and myelography
X-rays can help identify fractures, vertebral changes, and some patterns of disc mineralisation. However, they do not directly show the spinal cord, and they are not a reliable way to confirm or rule out IVDD on their own.
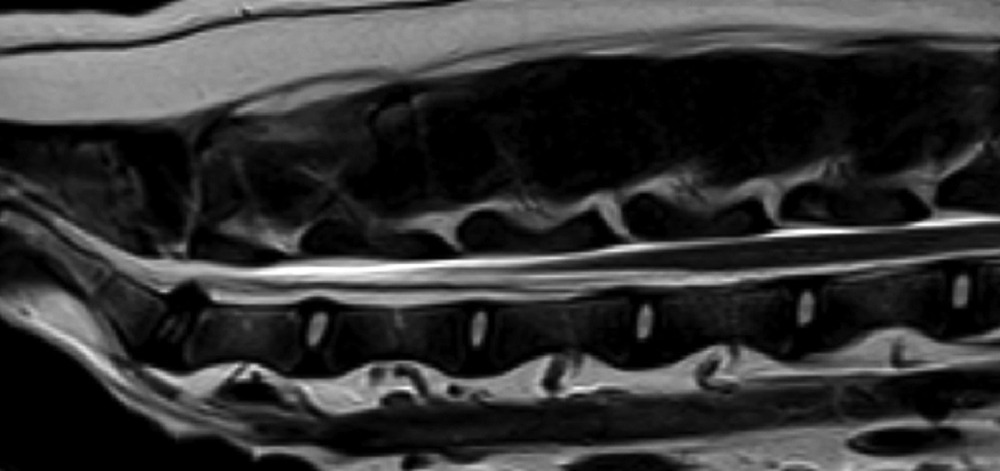
CT and MRI provide a much clearer view of the spine and the tissues around it. Myelography (a contrast study around the spinal cord) is sometimes used as well, especially in surgical planning. Your vet will talk you through what each test can and cannot answer in your dog’s case. 5, 6
Treatment options, from rest to surgery

Treatment is guided by two things: what is causing the problem, and how badly the nerves are affected right now. A dog who is sore but walking is a different situation from a dog who cannot stand, or who has lost deep pain sensation in the feet.
Conservative management
For milder cases, vets may recommend a period of strict rest, pain relief, and anti-inflammatory medication. “Rest” here is not just fewer walks. It usually means controlled confinement and carefully managed toileting to limit spinal movement while tissues settle. Your vet may also add medications for nerve pain, depending on the pattern of discomfort. 7
Surgery and what outcomes depend on
Surgery is typically considered when there are significant neurological deficits, severe pain that cannot be controlled, or imaging shows compression that is unlikely to respond to conservative care. In disc disease, one key factor is whether deep pain sensation is present. In general, dogs that still have deep pain sensation have a much better chance of functional recovery after surgery than dogs who have lost it, especially if the loss has been prolonged. 1
Because timing can affect outcomes, it is worth acting promptly when a dog deteriorates quickly, even if you are unsure what started it. 1, 4
Rehabilitation and return to function
Rehab is not just “extra”, it is often where steady progress happens. Depending on your dog’s needs, this can include gentle strength and balance work, assisted standing and walking, hydrotherapy, and a plan to rebuild stamina without overloading the spine. Recovery tends to be measured in weeks to months, not days.
Good pain control also matters. Pain makes dogs move differently, which can slow rehab and strain other parts of the body. Many veterinary teams use structured pain scoring and multimodal pain management approaches to keep dogs as comfortable and functional as possible during recovery. 8
Practical prevention and long-term management
Not every spinal disorder is preventable. But there is a lot you can do to reduce everyday strain and make setbacks less likely, particularly for dogs with known risk factors or a history of back pain.
Helpful, realistic habits include:
- Keeping your dog at a healthy body condition, as extra weight increases mechanical load on the spine
- Using a well-fitted harness instead of attaching a lead to a collar, especially for dogs with neck pain or known disc disease
- Adding rugs or non-slip runners on slippery flooring to prevent splits and sudden twists
- Using steps or ramps where your dog routinely jumps up or down (bed, couch, car)
- Choosing exercise that builds muscle steadily (controlled leash walks, gentle hill work, swimming if appropriate) rather than repeated high-impact leaps
If your dog has already had a spinal episode, prevention becomes management. The goal is not to keep them wrapped in cotton wool, it is to create an environment where safe movement is easy, and risky movement is less tempting. A physiotherapist or rehab-trained vet can be very helpful in setting that up.
Living with a dog who has spinal disease
A spinal diagnosis can land heavily, particularly if it arrives suddenly. It helps to remember that many dogs improve with the right plan, and that quality of life is often shaped by the day-to-day details: comfort, confidence on their feet, predictable routines, and support during flare-ups.
It is also worth being honest about what you are seeing at home. Videos of your dog walking, standing up, or trying stairs can help your vet interpret subtle changes over time. If something shifts quickly, or your dog seems less steady than yesterday, say so clearly and include the timeline. Those details can change triage decisions and treatment recommendations.
References
- American College of Veterinary Surgeons (ACVS): Intervertebral Disc Disease (IVDD)
- Dachshund IVDD Support Australia (DISA): What is IVDD
- Veterinary Specialist & Oncology Services (Australia): Intervertebral Disc Disease (IVDD) in Dogs
- Animal Referral Hospital (Australia): What is IVDD and what to do about it
- Today’s Veterinary Practice: Intervertebral Disk Disease in Dogs
- Animal Referral Hospital (Australia): Spinal disease in dogs, uncommon facts
- Queensland Veterinary Specialists (Australia): Intervertebral Disc Disease
- World Small Animal Veterinary Association (WSAVA): Global Pain Management Guidelines (update announcement)