Most people first notice a heart murmur because someone else mentions it. A GP hears an extra sound while listening to your chest, a nurse writes it in your notes, or a parent is told their child has one during a routine check. The word “murmur” can sound ominous, even when you feel perfectly well.
It helps to know that a murmur is not a diagnosis on its own. It is a sound of blood flow that can be completely harmless, or it can be a clue that a valve or heart structure needs a closer look. The practical question is not “is a murmur bad?”, but “what is making that sound, and does it matter for this person?”.1, 2
With the right assessment, most people end up with a clear plan: reassurance and occasional monitoring, or targeted treatment for an underlying condition. Either way, understanding what a murmur can mean tends to take the sting out of the uncertainty.
Why heart murmurs happen
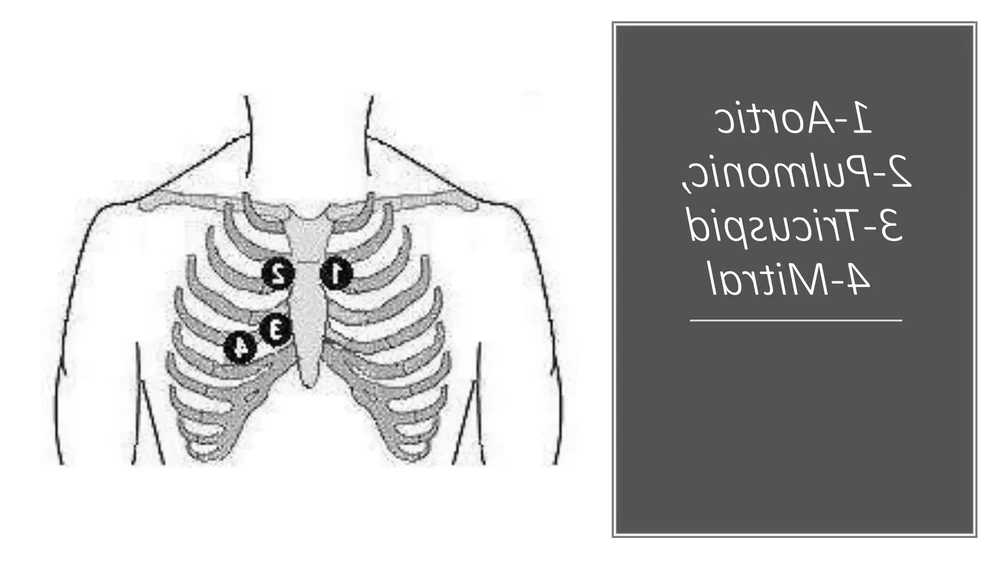
A heart murmur is the sound created by turbulent blood flow in or near the heart. Clinicians often describe it as a whooshing or swishing noise heard between the normal heart sounds when a stethoscope is placed on the chest.1
Turbulence can occur for benign reasons, such as when blood is moving faster than usual (for example during fever, pregnancy, or anaemia). It can also happen when blood is forced through a narrowed valve, leaks backwards through a valve that does not close properly, or is redirected through an abnormal opening in the heart.1, 2
Innocent (harmless) versus abnormal murmurs
Many murmurs are “innocent”, meaning they are not caused by heart disease and do not require treatment. Innocent murmurs are especially common in children, and they may come and go as heart rate and blood flow change with growth, activity, or illness.2
Other murmurs are “abnormal”, which means the sound is more likely to be associated with an underlying problem, most commonly heart valve disease in adults. This is why a murmur is usually treated as a starting point for assessment, not an answer in itself.3
What you might notice, and what you might not

Plenty of people with a murmur have no symptoms at all, particularly when the murmur is innocent. In those cases, the murmur is often found incidentally during an exam for something unrelated.1
When symptoms do appear, they usually relate to the condition causing the murmur rather than the murmur itself. Depending on the cause, this can include shortness of breath, chest pain, dizziness or fainting, swelling (fluid retention), or reduced exercise tolerance. In babies, poor feeding and poor growth can be a clue that the heart is working harder than it should.1
If you notice new symptoms, a change in what you can comfortably do day to day, or symptoms that are persistent rather than situational, it is reasonable to ask for a review even if the murmur was previously described as mild.
How a heart murmur is assessed
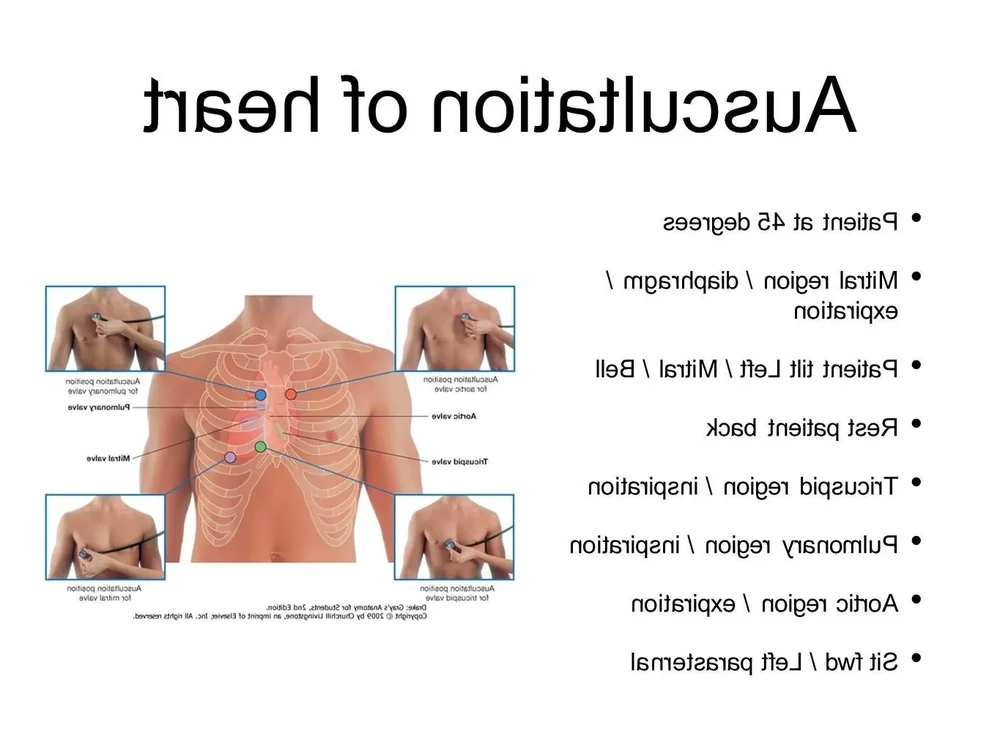
Assessment starts with a careful listen, and a bit of context. Clinicians consider where the murmur is loudest, when it occurs in the heartbeat, how loud it is, and whether it changes with position or activity. These details help decide whether a murmur sounds likely to be innocent or worth investigating further.4
If follow-up testing is needed, an echocardiogram (heart ultrasound) is usually the main test because it shows the heart’s structure and how blood flows through the valves and chambers. Depending on the situation, an ECG and chest X-ray may also be used as part of the overall picture.4
For many people, the outcome of this step is a simple, practical sentence: no heart disease found, or “there is valve disease and here is what we do next”. Either result is useful.
Types of murmurs, in plain language
Murmurs are often described by timing, which is one of the reasons your clinician might use terms that sound technical at first.
Systolic murmurs
Systolic murmurs occur when the heart contracts. Many innocent murmurs are systolic, but some systolic murmurs are related to valve problems or other conditions, so timing alone does not tell the whole story.2, 4
Diastolic murmurs
Diastolic murmurs occur when the heart relaxes and fills. In general, a diastolic murmur is more likely to need further assessment because it can be associated with underlying heart disease.4
Continuous murmurs
Continuous murmurs are heard throughout the heartbeat. Some are linked to specific structural patterns of blood flow that warrant investigation, particularly when found in infants and children.1
Treatment options, and when treatment is not needed
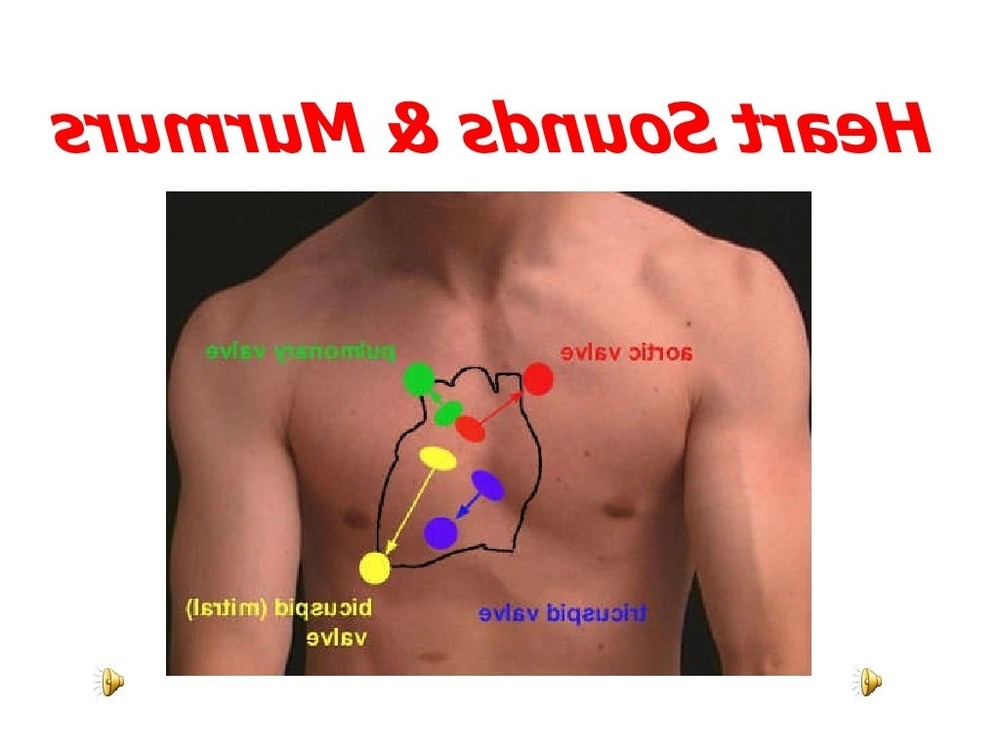
An innocent murmur does not require treatment. If the murmur is related to a temporary state that increases blood flow, such as fever or an overactive thyroid, the sound may lessen or disappear once the underlying issue is managed.4
When a murmur is linked to a heart condition, treatment depends on the cause and how it affects day-to-day function and risk. Options may include medications to manage symptoms and reduce strain on the heart, and in some cases procedures or surgery to repair or replace a faulty valve.4
A helpful way to think about it is this: clinicians do not treat the noise, they treat the reason for the noise. For some people, the right plan is simply periodic monitoring with repeat exams or echocardiograms.
A note on antibiotics before dental work
Many people have heard that a heart murmur means antibiotics are needed before dental procedures. Current guidance is more selective. Antibiotic prophylaxis is recommended only for a relatively small group of people at highest risk of serious outcomes from infective endocarditis, and it depends on the cardiac condition and the type of dental procedure.5, 6
If you have a murmur and upcoming dental work, it is worth asking your treating clinician whether you personally fall into a group where antibiotics are advised, rather than assuming it is automatically required.
Living well with a heart murmur

For many people, living with a murmur mainly means having a clear understanding of what it represents for them. If the murmur is innocent, that clarity is often the most meaningful “treatment”. If the murmur reflects an underlying condition, the goal becomes steady, sensible management rather than constant vigilance.
It can help to focus on the practical fundamentals that support heart health in general, alongside whatever specific plan your clinician recommends:
- Keep regular reviews if advised, especially if you have known valve disease.
- Stay active in a way that matches your fitness and any medical guidance.
- Attend to blood pressure, cholesterol, and diabetes if relevant.
- Prioritise oral health and routine dental care, which reduces everyday sources of bacteraemia and is part of broader endocarditis prevention advice for at-risk people.7
If your symptoms change, or you are unsure whether a new limitation is “just getting older” or something worth checking, it is reasonable to book a review. Murmurs can stay stable for years, but heart conditions can also evolve, and good follow-up is designed to catch that early.
Heart murmurs in children
In children, murmurs are extremely common. A large proportion of kids will have an innocent murmur detected at some point, particularly between early childhood and the teenage years.2
What tends to reassure parents is that innocent murmurs do not mean a child has a heart problem, and they usually do not require activity restrictions. When clinicians are uncertain, or the murmur has features that could suggest a structural issue, an echocardiogram may be recommended to clarify what is going on.2, 4
For the smaller group of children whose murmurs relate to congenital heart disease, early detection and appropriate follow-up makes a real difference. The plan may range from observation to medication or procedures, depending on the specific diagnosis.
Prevention and risk reduction, what actually applies
You cannot always prevent the structural causes of a murmur, especially congenital conditions. But many risk factors for acquired heart disease and valve problems are modifiable, and they matter over the long run.
In day-to-day terms, prevention looks less like special tricks and more like consistent basics: maintaining a healthy weight, staying physically active, managing blood pressure and cholesterol, not smoking, and treating conditions such as diabetes. These steps support cardiovascular health whether or not a murmur is present.8
If you have known valve disease or a condition that increases endocarditis risk, ask your clinician what prevention means for you specifically. In some cases it includes targeted dental antibiotic prophylaxis for certain procedures, but in many cases it does not.5, 6
Final thoughts
A heart murmur is a finding, not a verdict. Sometimes it is simply the sound of a healthy heart moving blood efficiently. Sometimes it is an early hint that a valve or structure needs attention.
The most useful next step is usually the simplest one: confirm what type of murmur it is, clarify whether an echocardiogram is needed, and understand what would count as a meaningful change over time. That combination of information and follow-up is what turns worry into a workable plan.
References
- Mayo Clinic: Heart murmurs (Symptoms and causes)
- American Heart Association: Heart Murmurs
- American Heart Association: Abnormal and “Innocent” Heart Murmurs
- Mayo Clinic: Heart murmurs (Diagnosis and treatment)
- American Dental Association: Antibiotic Prophylaxis Prior to Dental Procedures
- Australian Prescriber: Antibiotic prophylaxis for dental procedures
- NICE Guideline (NCBI Bookshelf summary): Prophylaxis against infective endocarditis
- healthdirect Australia: Heart disease

