Most people do not start by wondering whether their dog has high blood pressure. It usually begins with something small that does not quite add up: a dog that seems a bit “off”, a sudden change in vision, an eye that looks different in the light, or a routine blood test that hints at kidney trouble.
What makes canine hypertension (high blood pressure) tricky is that it can sit quietly in the background. Dogs can look perfectly normal while pressure is building in vessels that supply the eyes, brain, kidneys, and heart. By the time obvious signs appear, there may already be what vets call target organ damage, which is why this condition matters in day-to-day care, not just in emergencies.1, 2
Hypertension is also easy to misunderstand. It is often assumed to be a “heart problem”, but in dogs it is more commonly a sign that something else is going on, especially kidney or hormone disease. The practical goal is not to panic about a single reading, but to measure well, look for causes, and treat early enough to protect the organs that are most vulnerable.1, 2, 3
What hypertension means for dogs
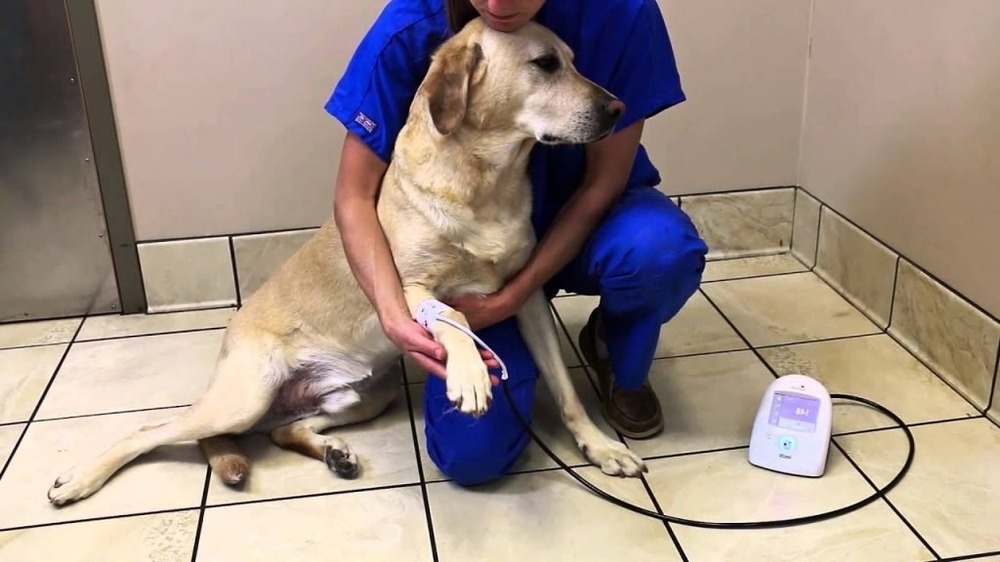
Hypertension simply means the blood is pushing against artery walls at a higher pressure than is healthy over time. In practice, vets focus most on systolic blood pressure (the “top number”), because it is the figure most commonly measured in clinics and most closely tied to risk of complications in dogs and cats.1, 2
One of the most useful ways to think about hypertension is through what it can do to the body rather than how it “feels”. Sustained high blood pressure can injure delicate blood vessels, particularly in the retina, kidneys, and brain. In dogs, that can show up as sudden visual loss, retinal bleeding, worsening kidney parameters, or neurological episodes such as seizures.1, 2, 4
Causes of hypertension in dogs
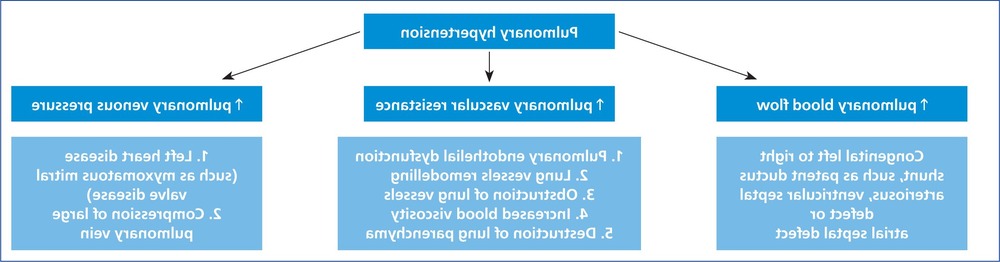
Hypertension in dogs is usually grouped into primary (idiopathic) and secondary forms. Primary hypertension means no underlying cause is found. It exists, but in dogs it is considered uncommon, and most cases are secondary to another medical issue.1, 2
Secondary hypertension, the common pattern
Secondary hypertension is driven by an identifiable condition. The most common contributors discussed in veterinary guidelines and reviews include:
- Kidney disease (chronic kidney disease or acute kidney injury)1, 3
- Hyperadrenocorticism (Cushing’s disease)1, 5
- Diabetes mellitus and rarer endocrine or adrenal tumours (for example pheochromocytoma)1, 5
It is worth noting that “older dog” is not a cause on its own. Age matters because the underlying diseases that trigger hypertension become more likely over time, and because some changes can be subtle until a screening test brings them into view.2, 5
Weight, fitness, and the bigger health picture
Obesity is not a neat, single-line cause of hypertension in dogs the way it is often talked about in people. Still, extra weight can complicate a dog’s health, affect stamina and mobility, and raise the odds of other problems that do influence blood pressure and long-term wellbeing. If your dog is carrying extra condition, a vet-guided plan is a sensible, low-regret step.6, 7
Signs you might notice at home
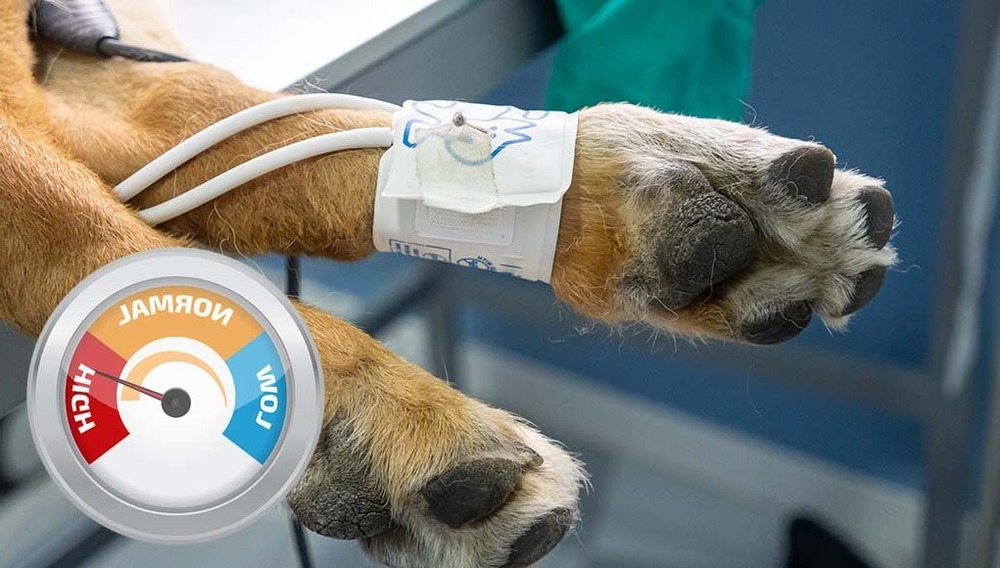
Dogs with hypertension often have no obvious signs, especially in the early stages. When signs do appear, they are frequently linked to which organ system is being affected rather than to blood pressure itself.1, 2
Some of the more common warning signs that prompt a blood pressure check include:
- Sudden vision changes, bumping into objects, reluctance on stairs, or apparent blindness (often linked to retinal injury)1, 4, 5
- Seizures, disorientation, wobbliness, or other neurological changes5
- Increased drinking and urination, weight or appetite changes, or a general “not quite right” presentation that later ties back to kidney or endocrine disease5
These signs are not specific to hypertension, and that is the point. They are clues that deserve a careful vet assessment, including blood pressure measurement, rather than guesswork at home.
How vets diagnose hypertension
A blood pressure reading in a clinic sounds straightforward, but good technique matters. Dogs can spike higher when they are anxious, and a single elevated number does not always equal true hypertension. Current veterinary guidance emphasises repeatable measurements in a calm environment, using appropriate cuff size and consistent method, before making big decisions on long-term treatment.2, 3
Because most canine hypertension is secondary, diagnosis usually includes looking for an underlying driver. Depending on the dog, this may involve:
- Blood and urine testing (kidney values, urine protein, endocrine screening where appropriate)2, 3
- Eye examination to look for retinal bleeding, swelling, or detachment, which can be a clear sign of hypertension-related injury2, 4, 5
- Imaging or further investigations if the initial picture suggests a specific disease process2, 5
In many cases, the conversation becomes: what is the blood pressure doing across several readings, and is there evidence of target organ damage that raises the urgency to treat?1, 2, 3
Treatment options and what they look like in real life

Treatment is usually a blend of managing the underlying cause (when possible) and lowering blood pressure to reduce ongoing risk. The aim is not to chase a “perfect” number overnight, but to bring pressure down safely and then keep it stable with monitoring and dose adjustments.2, 3
Medications commonly used
Vets choose antihypertensive medication based on the dog’s readings, concurrent disease, and evidence of organ injury. In many dogs, a calcium channel blocker such as amlodipine is commonly used, and ACE inhibitors or other drug classes may be added depending on the case, especially when kidney disease and protein loss in urine are part of the picture.2, 3, 8
It is also worth knowing that some commonly used hypertension drugs in pets are prescribed off-label (extra-label). That is normal in veterinary medicine, but it makes follow-up and clear instructions from your vet even more important.8
Diet, exercise, and supportive care
For dogs with secondary hypertension, lifestyle advice is usually about supporting the underlying condition and reducing avoidable strain on the body. Your vet may discuss weight management, appropriate daily movement (matched to age and mobility), and a diet plan suited to any kidney or endocrine diagnosis.
If weight is part of the picture, body condition scoring can be more useful than the number on the scales alone. Vet teams often use standardised tools like the WSAVA body condition score charts to make the discussion concrete and consistent.9
Monitoring and follow-up
Blood pressure management is rarely “set and forget”. Most dogs need rechecks, especially early on, so the vet can confirm the reading is truly improving, watch for side effects, and make stepwise changes. Ongoing monitoring is also how secondary causes, such as kidney disease, are tracked over time.2, 3, 5
Living with hypertension, prognosis, and quality of life

When hypertension is found early, and when the underlying condition can be treated or stabilised, many dogs do well. The main risk to quality of life tends to come from complications such as retinal injury or progression of kidney disease, not from the act of taking a daily tablet.1, 3, 5
Supportive care is often simple, but meaningful: predictable routines, sensible exercise, and a home environment that helps a dog cope if vision is reduced. If your dog has had any eye changes, it is also reasonable to ask your vet how often an eye exam should be repeated, as ocular damage can be one of the clearest ways hypertension shows itself.4, 5
Final thoughts
Hypertension in dogs is not always dramatic, which is exactly why it deserves a steady, practical approach. If your dog has kidney disease, Cushing’s disease, diabetes, unexplained eye changes, or neurological signs, a blood pressure check is a sensible part of joining the dots. The most helpful mindset is to treat hypertension as a useful clue, not a label, and to work with your vet on repeat measurements, underlying causes, and follow-up that protects your dog’s eyes, kidneys, and brain over the long term.2, 3, 5
References
- Merck Veterinary Manual: Systemic and Pulmonary Hypertension in Dogs and Cats
- ACVIM Consensus Statement (2018): Guidelines for the identification, evaluation, and management of systemic hypertension in dogs and cats
- International Renal Interest Society (IRIS): Hypertension
- Ocular lesions associated with systemic hypertension in dogs: 65 cases (2005 to 2007)
- VCA Animal Hospitals: Systemic Hypertension (High Blood Pressure) in Dogs
- RSPCA Knowledgebase: How do I tell if my dog is overweight?
- RSPCA Pet Insurance: How to spot signs of pet obesity
- VCA Animal Hospitals: Amlodipine (besylate) for pets
- WSAVA: Global Nutrition Guidelines (includes body condition score tools)