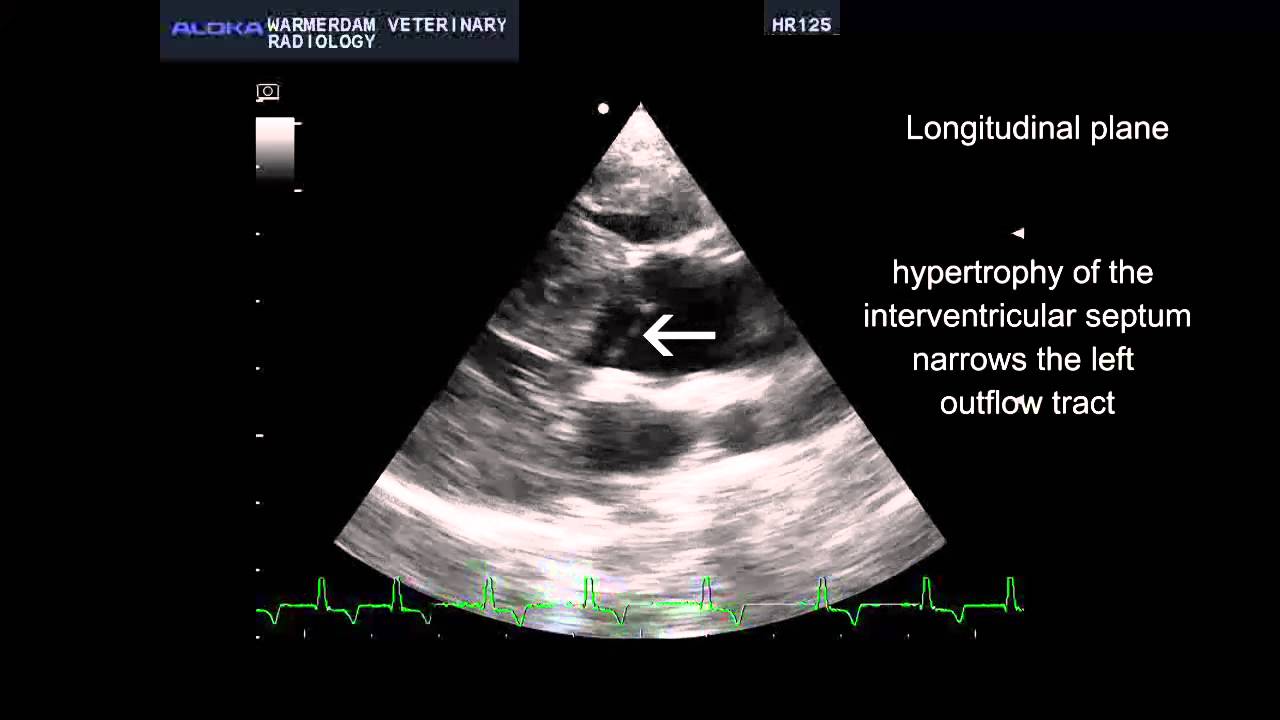
People often start wondering about heart disease in dogs in a fairly ordinary way. A dog that used to bound up the driveway now takes longer to recover after a walk, or starts coughing at night in a way that does not quite fit a cold. Sometimes a vet hears a murmur at a routine check, and suddenly you are looking up unfamiliar terms and trying to work out what matters and what does not.
Hypertrophic cardiomyopathy, usually shortened to HCM, is one of those terms that can sound more common than it is. In dogs, true HCM is considered uncommon, especially compared with cats, and it can be confused with other, more typical canine heart problems that also cause thickened heart walls or similar symptoms.1, 2
Still, the practical question is the same: if your dog’s heart is under strain, what signs should you take seriously, how is it properly diagnosed, and what does day to day management look like when you are trying to keep life steady and comfortable?
Understanding hypertrophic cardiomyopathy in dogs
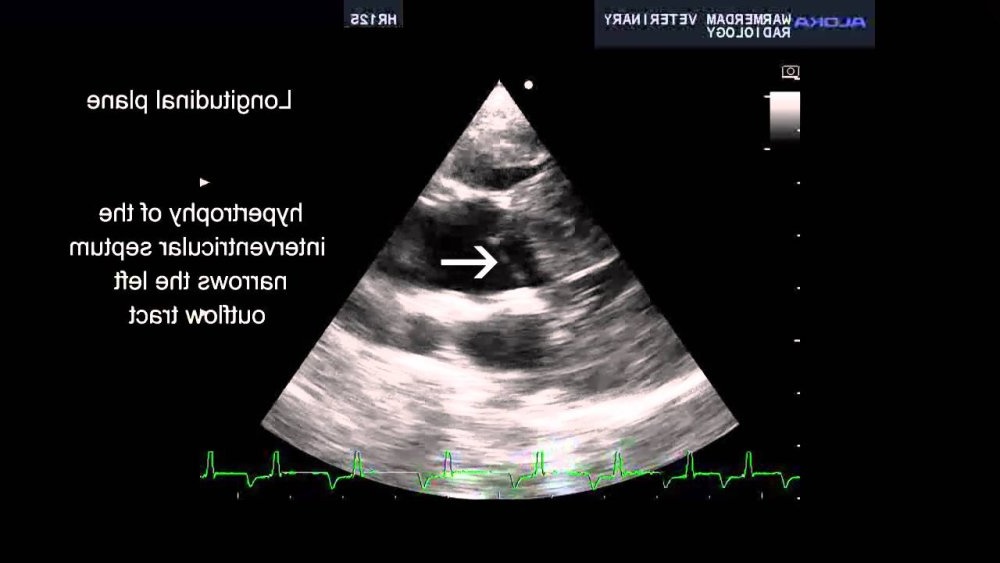
HCM refers to a pattern where the heart muscle, most often the left ventricle, becomes abnormally thickened. The thickening can make the heart stiffer, which means it may not fill as efficiently between beats, even if it still squeezes strongly.1
In real dogs in real clinics, the harder part is often not the definition, but the sorting out. A thickened heart wall on ultrasound can have several causes. Some are primary (a disease of the heart muscle itself) and some are secondary, where the heart thickens in response to another problem such as chronic high blood pressure or hormonal disease. That is why vets tend to talk about the underlying cause, not just the ultrasound appearance.1
It is also worth holding gently in mind that HCM is rare in dogs. In cats, HCM is the best known cardiomyopathy by far. In dogs, other conditions are much more common, particularly myxomatous mitral valve disease in small breeds and dilated cardiomyopathy in some larger breeds.1, 5
What thickening means for heart function
When the muscle is thickened and stiff, the heart may fill with less blood each cycle. The body can compensate for a while, but if pressures rise inside the heart, fluid can begin to back up towards the lungs. That is one pathway to congestive heart failure, which is where signs like faster breathing at rest and reduced stamina start to appear.4, 6
Genetics, breed, and what we actually know
You will sometimes see lists of “at risk” breeds for canine HCM online. The evidence is not as clear-cut as it is for some other inherited heart diseases. What we can say with more confidence is that canine HCM is uncommon overall, and published case series suggest some groups of dogs are overrepresented, including smaller breeds in at least one retrospective study.2
If a breeder claims screening for “HCM” in dogs, it is reasonable to ask what that screening involves. For most dogs, the meaningful screen is a cardiology exam that may include echocardiography, and sometimes rhythm monitoring, interpreted in context by a clinician with cardiac training.
Signs you might notice at home

Dogs are not especially good at advertising early heart trouble. Some will simply adjust their own pace, which can be easy to miss if changes happen gradually. When signs do show up, they are often not specific to HCM. They are signs that the heart and lungs are not coping as easily as they used to.
Common patterns owners report include:
- Reduced exercise tolerance, tiring sooner on walks or play
- Coughing, often more noticeable at night or after activity
- Fast or laboured breathing, including at rest
- Fainting or collapse (syncope), sometimes linked with excitement or exertion
- Restlessness at night, or difficulty settling into a comfortable sleeping position
These signs can occur with many types of heart disease, and also with non-cardiac problems such as airway disease. The safest approach is to treat them as a reason for a proper veterinary assessment, rather than trying to match symptoms to a single diagnosis at home.4, 6
When it is urgent
If your dog is struggling to breathe, has blue or very pale gums, collapses, or cannot settle because breathing seems difficult, that is a same day emergency. In Australia, the practical step is to contact your nearest vet or emergency clinic straight away and let them triage you by phone.7
How vets diagnose HCM, and why it can be tricky
A stethoscope exam is a starting point, not a finish line. Murmurs, extra heart sounds, and rhythm changes can suggest heart disease, but they do not tell you which disease, or how severe it is.
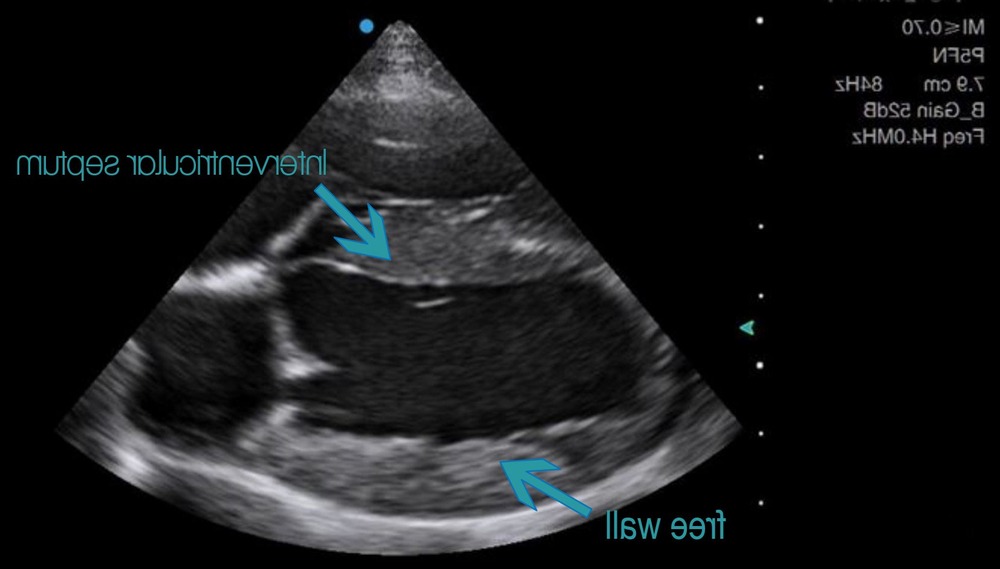
The test that matters most for HCM is an echocardiogram (ultrasound of the heart). It allows measurement of wall thickness, chamber sizes, filling patterns, and assessment for dynamic outflow obstruction or valve leakage. In many cases, your vet may recommend referral to a veterinary cardiologist, because subtle distinctions in cardiac ultrasound interpretation can change what “thickening” means clinically.1, 8
Other tests you may see alongside ultrasound
Depending on the signs and what the vet hears, diagnostic work-up may include:
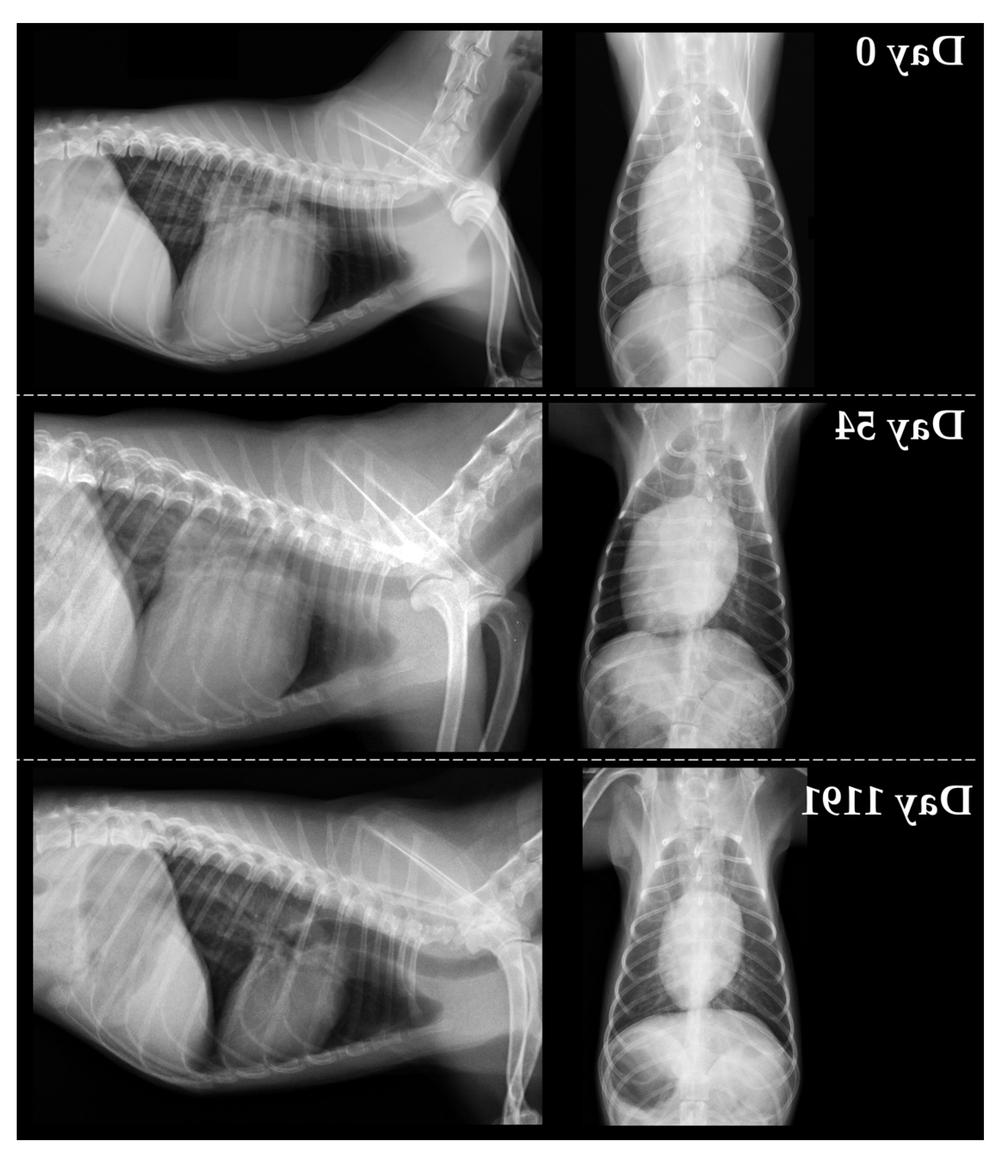
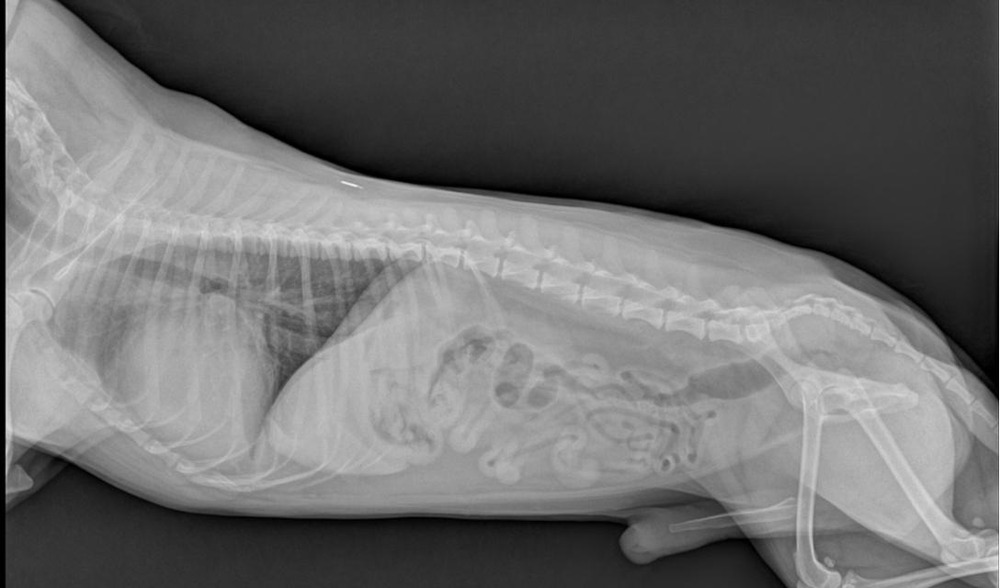
- Chest X-rays to look for heart enlargement and fluid in or around the lungs
- ECG (electrocardiogram) to assess rhythm and electrical conduction
- Blood pressure measurement and blood tests to look for secondary causes or complicating illness
- Longer rhythm monitoring (such as Holter monitoring) if fainting or intermittent arrhythmias are suspected
These are not “extra for the sake of it”. They help separate primary cardiomyopathy from other causes of thickened walls, and they help stage risk, which is what guides treatment decisions.1, 8
Treatment and management that fits real life
There is no single medication plan that suits every dog labelled with HCM, because the important details are not the name, but what the heart is doing. Is there congestion and fluid? Is there an obstructed outflow pattern? Are arrhythmias present? Is there a secondary cause driving the changes? Those questions shape the plan.
Medications you might encounter
When clinical signs are present, treatment is usually aimed at controlling congestion, supporting function, and managing rhythm problems where needed. Depending on the case, vets may prescribe:
- Diuretics if there are signs of congestive heart failure (to reduce fluid build-up)
- Medications to influence heart rate and relaxation of the heart muscle in selected cases
- Anti-arrhythmic medication if significant rhythm disturbances are documented
It is tempting to compare notes with other owners, but heart drugs are very context-dependent. A medication that helps one dog can be unhelpful, or even risky, in another dog with a different physiology. Your vet’s plan will usually evolve over time as monitoring results come back and your dog’s day to day comfort becomes clearer.
Activity, weight, and the “middle lane” approach
For many dogs with heart disease, a steady routine works better than extremes. Complete rest can lead to loss of conditioning and weight gain. Strenuous bursts can tip a borderline dog into coughing, breathlessness, or collapse.
In practical terms, think in terms of gentle, predictable exercise and stop well before your dog becomes puffed or reluctant. Weight management also matters because extra body weight increases workload on the heart and lungs, and can make breathing harder during warm weather.
Monitoring at home
Owners are often the first to notice that something has shifted. A simple, useful habit is to keep an eye on sleeping breathing. If your dog’s resting breathing rate is consistently higher than usual, or effort looks increased, it is worth contacting your vet promptly, even if everything else seems normal.4, 6
Prognosis, uncertainty, and what to plan for
“What is the prognosis?” is a reasonable question, and it is also one that tends to be answered in probabilities, not promises. In dogs, HCM is uncommon and the published veterinary literature suggests outcomes can vary widely. Some dogs live for years after diagnosis, and some deteriorate quickly, particularly if serious arrhythmias or heart failure develops.2
It can help to frame prognosis in terms of what we can measure and adjust. Breathing rate, appetite, stamina, fainting episodes, heart rhythm, and ultrasound findings all inform how the condition is tracking, and whether the current plan is doing its job.
Breeding considerations
If HCM, or a similar cardiomyopathy pattern, is suspected to be inherited in a line, the cautious approach is to avoid breeding affected dogs and to discuss screening protocols with a veterinary cardiologist. In dogs, many heart conditions have hereditary components to varying degrees, and reducing inherited risk generally starts with clear diagnosis and honest disclosure in breeding decisions.5
Living with a dog diagnosed with HCM
Most households settle into a rhythm. Medications become part of the day, and walks become a little more observant. The goal is not to wrap life in cotton wool, but to keep it workable and calm, with enough structure that you notice early if things change.
It often helps to keep a short record of:
- Medication doses and any side effects
- Exercise tolerance (what your dog comfortably does now)
- Coughing frequency or changes in breathing
- Any collapse or “wobble” episodes, with notes on what happened beforehand
If you ever feel you are guessing, that is a good reason to ask for a recheck, or to request referral. Cardiac disease management is usually a series of small adjustments, and good follow-up is what turns those adjustments into better comfort and a steadier quality of life.
Final thoughts
Hypertrophic cardiomyopathy in dogs sits in an awkward space. It is a real diagnosis, but it is also uncommon, and it can look similar to other conditions that are more familiar in canine practice.1, 2
The most helpful thing you can do is stay close to the practical signals: breathing, stamina, cough, fainting, and the results of objective tests like echocardiography. With a clear diagnosis, a tailored plan, and steady monitoring, many dogs do well for a meaningful time, and day to day life can remain surprisingly normal.
References
- Merck Veterinary Manual: Hypertrophic Cardiomyopathy in Dogs and Cats
- Journal of Veterinary Internal Medicine: Retrospective evaluation of hypertrophic cardiomyopathy in 68 dogs
- Merck Veterinary Manual: Overview of Cardiomyopathy in Dogs and Cats
- Lort Smith Animal Hospital: Heart disease in dogs
- ACVIM Consensus Guidelines (2019): Diagnosis and treatment of myxomatous mitral valve disease in dogs
- Sydney Animal Hospitals: Heart disease in dogs
- RSPCA Victoria: Issues requiring medical help (difficulty breathing and other emergencies)
- Cornell University College of Veterinary Medicine: Cardiology service (diagnostic tests including echocardiography and ECG)
- PubMed: ACVIM consensus guidelines for the diagnosis and treatment of myxomatous mitral valve disease in dogs (citation record)