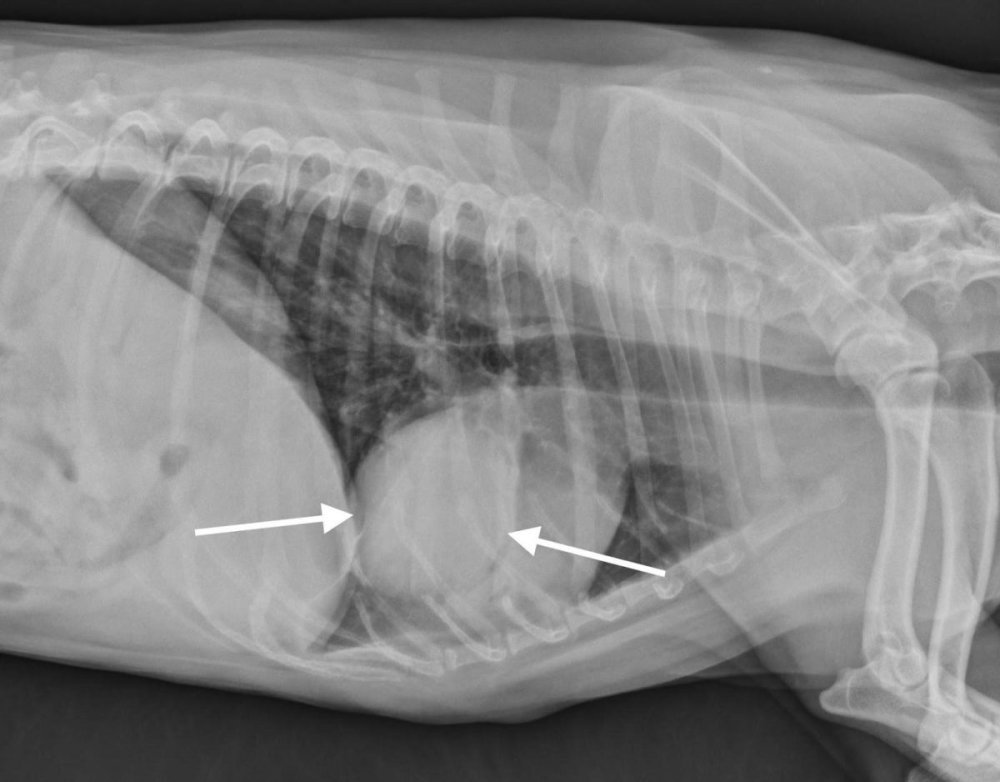
It often starts with something small that does not quite fit. A cough that lingers after a cold. Breathing that sounds a little noisier on walks. A dog who used to bounce up the stairs, now pauses halfway. Most of the time these changes have everyday explanations, but they are also the kind of slow shifts that are worth taking seriously.
Lung cancer in dogs is not common, and it is easy to assume it would be obvious if it were happening. In practice, some dogs show very few signs until a mass is spotted on an X-ray taken for another reason.1, 2 When it is caught early, there may be meaningful treatment choices. When it is caught late, the focus often shifts to comfort and good days.
What helps most is having a clear sense of what can raise suspicion, how vets confirm what is going on, and what treatment and supportive care can realistically look like.
Causes and risk factors
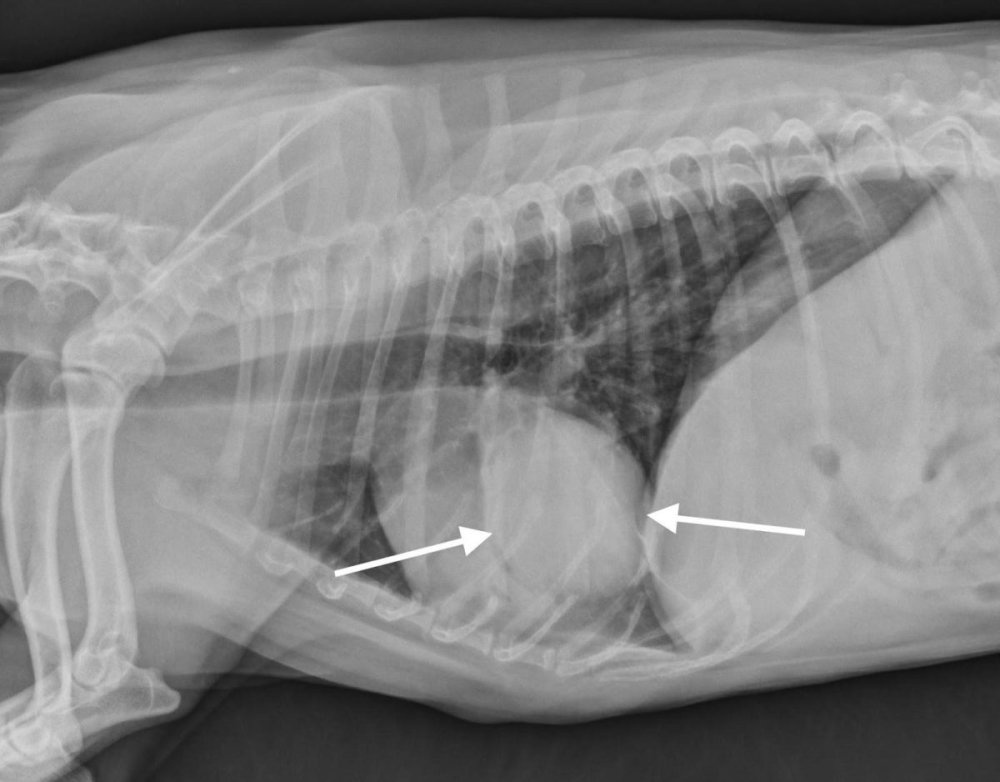
When vets talk about “lung cancer” in dogs, they usually separate it into two broad groups: tumours that start in the lung (primary), and tumours that have spread to the lungs (metastatic) from somewhere else in the body.1 Metastatic disease is actually more common than a primary lung tumour.1
The exact cause of primary lung tumours is not always known. Risk is thought to be influenced by a mix of age, environment, and biology. Many dogs diagnosed are middle-aged to older.1, 3
Environmental exposure matters, too. Living with cigarette smoke has been associated with airway disease and cancers in dogs, and there is no risk-free level of passive smoke exposure for animals.4, 5 Some sources also note increased risk with certain pollutants (including asbestos).1
Breed and head shape may play a role in which cancers are seen with smoke exposure. Longer-nosed dogs are described as being more prone to nasal cancer, while shorter-nosed dogs may be more prone to lung cancer in this context, although individual risk is still hard to predict for any one dog.6
What you might notice at home
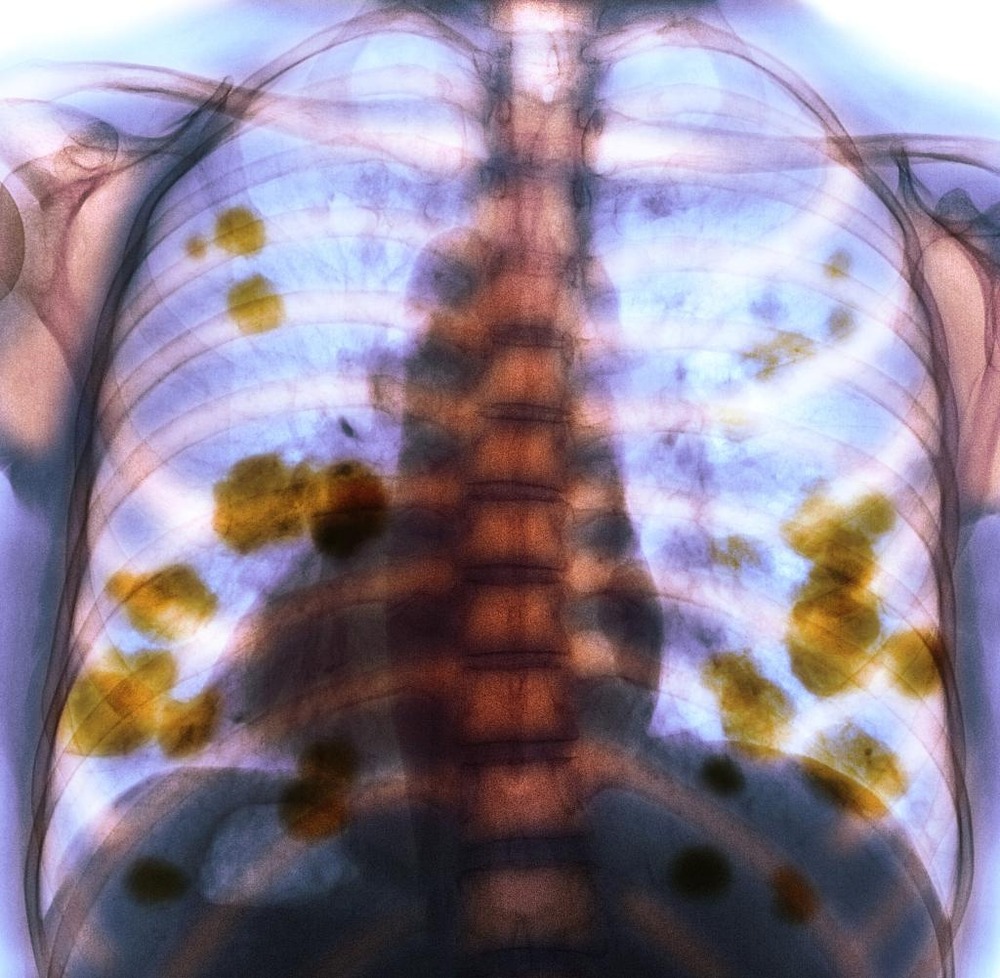
Lung cancer signs can overlap with far more common problems such as infections, chronic bronchitis, heart disease, laryngeal paralysis, or even simple deconditioning. That overlap is one reason dogs can go a while before anyone thinks to check the chest.2, 3
Changes that vets commonly associate with primary lung tumours include:
- Persistent cough, often dry or non-productive3, 7
- Faster breathing rate at rest, or more effort to breathe3, 7
- Reduced exercise tolerance, tiring earlier on walks3, 7
- Weight loss, reduced appetite, or lethargy2, 3
- Coughing up blood (less common, but important if seen)2, 3
- Lameness in some dogs, including from hypertrophic osteopathy (a bone and limb change linked to some chest masses)1, 7
A useful detail, and one that often surprises people, is that some dogs have no obvious symptoms. A lung mass may be found incidentally during radiographs for an unrelated problem, particularly in older dogs.1, 7
When it is an emergency
If your dog is struggling to breathe, has blue or grey gums, collapses, or cannot settle, treat it as urgent. Breathing effort can worsen quickly for many reasons, including fluid around the lungs, pneumonia, airway obstruction, or a heavy tumour burden.7
How vets diagnose lung cancer
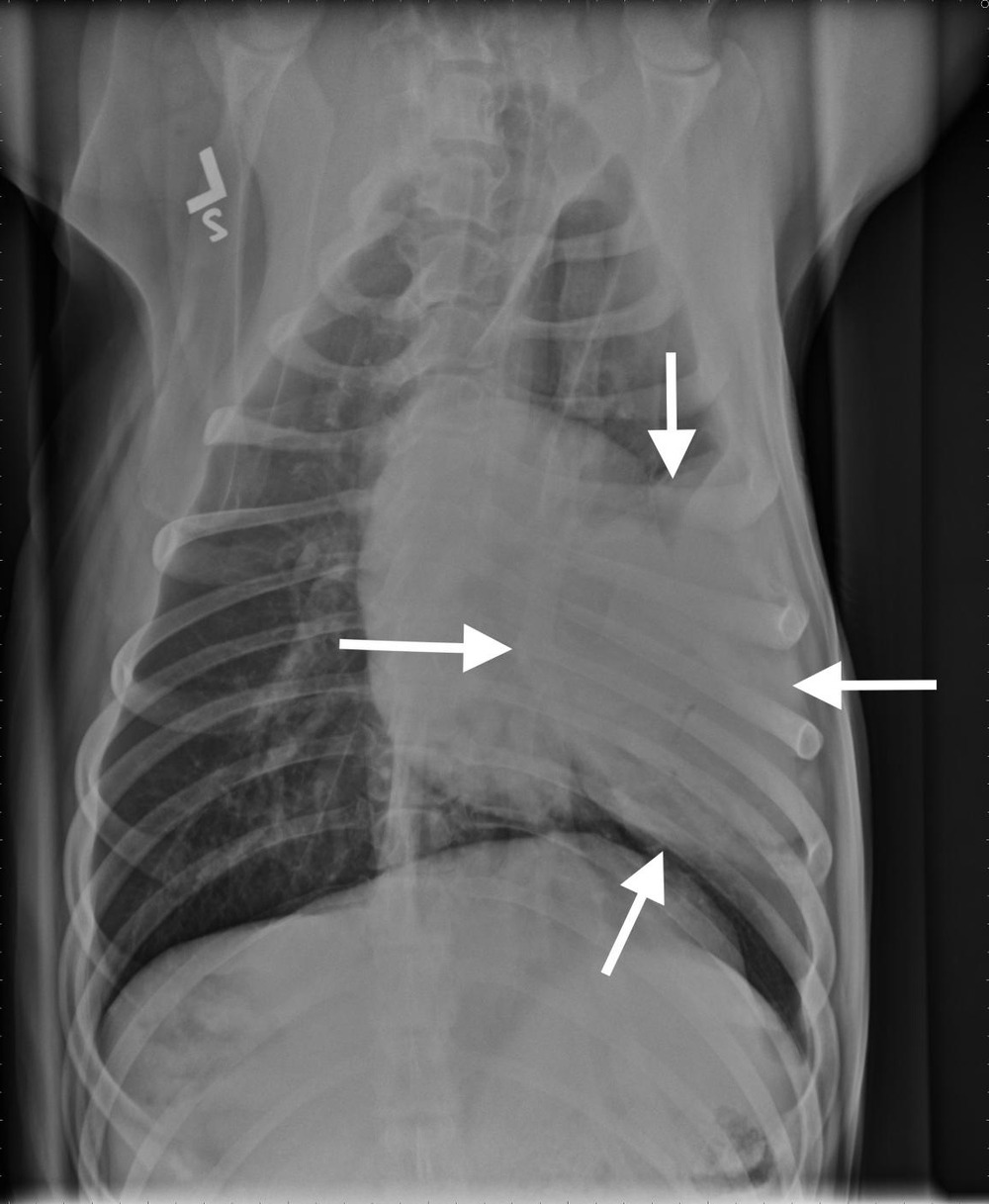
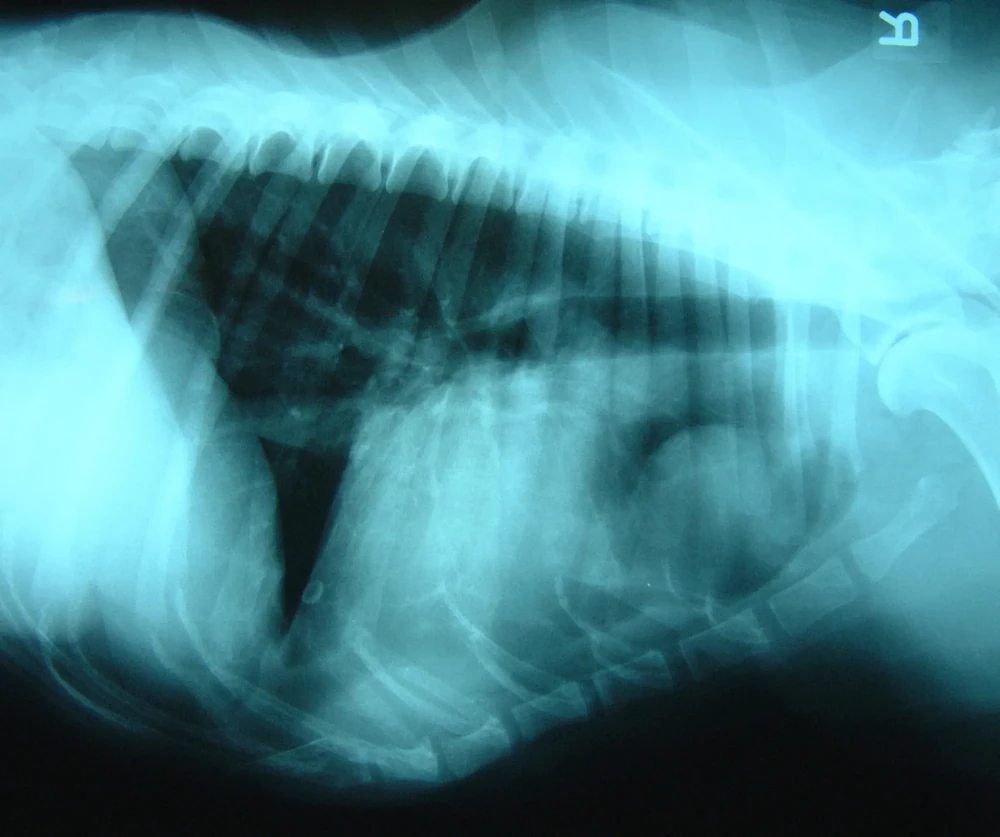
Diagnosis usually happens in layers. A vet will start with a physical exam and history, then move to imaging. Chest X-rays are often the first step, and they can show lung masses, changes in lung pattern, and sometimes enlarged lymph nodes.1, 7
A CT scan can provide a much clearer map of what is happening in the chest, including the size and location of a mass, whether lymph nodes look involved, and whether there are multiple lesions that might suggest spread.1, 7
To confirm cancer, vets often need cells or tissue. Depending on the case, that may involve a needle sample (fine needle aspirate) or a surgical biopsy, then examination by a pathologist.1, 7 Imaging can strongly suggest a tumour, but biopsy is usually needed to know what type it is and to guide treatment decisions.7
Staging matters
Because many lung lesions are metastatic, and because primary lung tumours can spread, vets often recommend “staging” tests. This can include blood and urine tests, more detailed chest imaging, and sometimes an abdominal ultrasound to look for a primary tumour elsewhere or signs of spread.1, 7
Treatment options that may be offered

Treatment depends on whether the tumour is solitary, whether it has spread, what type it is, and your dog’s overall health. In many dogs with a single primary lung lobe tumour, surgery to remove the affected lung lobe (lung lobectomy) is considered the treatment of choice, especially when there is no evidence of spread.1, 7
Surgery can be performed via an open approach or, in some cases, minimally invasive thoracoscopy. Post-operative care is focused on breathing support, pain control, and rest while the chest heals.1
Chemotherapy and radiation therapy may be considered in selected cases, particularly when there is metastatic disease, lymph node involvement, incomplete surgical margins, or tumour types known to behave aggressively. The expected benefit varies, so it is worth a detailed conversation with a veterinary oncologist about goals and likely outcomes for your dog’s specific diagnosis.1, 2, 7
Supportive care is still real care
Not every dog is a surgical candidate, and not every family wants aggressive treatment. Supportive care can include medications to manage cough, nausea, appetite, anxiety, and pain, plus practical adjustments at home. Good palliative planning is not “doing nothing”, it is choosing comfort and function as the priority.
International veterinary pain guidelines emphasise structured pain recognition and treatment, including for cancer-related pain, with plans tailored to the individual patient and reassessed over time.8
Prognosis, in plain language
Prognosis is not one number, and it is rarely the same across dogs. It tends to be influenced by:
- Tumour size and whether it can be fully removed1, 9
- Lymph node involvement1, 7
- Evidence of metastasis (spread)1, 7
- Histologic type and grade (what the pathologist sees under the microscope)1, 9
- How well your dog tolerates treatment, and any other health problems
In surgical cases where a solitary primary tumour is removed, some dogs can do well for a year or more on average, and longer in favourable situations. Outcomes are generally better when tumours are smaller, more peripheral, and there is no lymph node involvement.1
On the other hand, when lymph nodes are involved or multiple tumours are present, survival times are often shorter, and the plan may focus more on maintaining comfort and breathing quality rather than cure.7
Prevention and sensible risk reduction
You cannot prevent every cancer, and you cannot control every exposure. Still, a few practical steps are worth taking because they support respiratory health generally.
The clearest, most actionable prevention step is to avoid exposing your dog to tobacco smoke, including second-hand smoke in the air and third-hand residue that clings to clothes, furniture, and carpets.4, 5 If quitting is not immediately possible, reducing indoor smoking and changing clothes after smoking can help reduce what is carried back into the home, although it does not remove risk entirely.5
It also helps to be thoughtful about irritants in general:
- Keep strong fumes (sprays, solvents, harsh cleaners) well away from pets and ventilate the home.
- If you live in a high-traffic area, choose walking times when air quality is better, and avoid heavy exercise near exhaust.
- Stay on top of chronic cough or recurrent “bronchitis” rather than repeatedly hoping it will pass, since ongoing inflammation can mask new problems.
Living with a dog diagnosed with lung cancer

Once a diagnosis is made, day-to-day life often becomes a balance between medical plans and what your dog is showing you at home. Many families find it helpful to keep notes on resting breathing rate, appetite, sleep, interest in walks, and tolerance for stairs or heat. Small changes can be easier to spot when you look back over a week, rather than trying to remember how things felt yesterday.
Quality of life support is usually built around a few themes:
- Breathing comfort, including avoiding overexertion and heat, and using medications as directed.
- Nutrition that is easy to eat and digest, especially if appetite is variable.
- Pain control with a plan that is adjusted as needs change, rather than waiting for obvious distress.8
- Home set-up changes, such as rugs for traction, a ramp for the car, or resting spots on one level.
If you are deciding between treatments, ask your vet to walk you through what the next few weeks would look like for each option, including hospital stays, rechecks, likely side effects, and what would trigger a plan change. Clear expectations can make decisions feel less overwhelming.
Final thoughts
Lung cancer in dogs can be quiet at first, and that is part of what makes it hard. A persistent cough, changes in stamina, weight loss, or breathing effort do not automatically mean cancer, but they do justify a proper check, especially in older dogs.1, 7
When a lung tumour is found, the most useful next step is usually careful staging and a discussion of goals. For some dogs, surgery offers a real chance of extended time. For others, the best care is steady symptom management and a focus on comfort. Both approaches can be thoughtful, and both can be kind.
References
- American College of Veterinary Surgeons (ACVS), Lung Lobe Tumors (Pneumonectomy/Lung Lobectomy)
- PetMD, Lung Cancer in Dogs
- Merck Veterinary Manual, Neoplasia of the Respiratory System in Dogs and Cats
- RSPCA Australia Knowledgebase, Is it risky to smoke or vape around companion animals?
- US Food and Drug Administration (FDA), Secondhand (and Third-Hand) Smoke May Be Making Your Pet Sick
- Cancer Council Victoria, Tobacco in Australia: Health effects of secondhand smoke on pets
- VCA Animal Hospitals, Lung Tumors
- World Small Animal Veterinary Association (WSAVA), Global Pain Guidelines
- Journal of Veterinary Internal Medicine (PubMed), Prognosis of primary pulmonary adenocarcinoma after surgical resection in small-breed dogs: 52 cases (2005-2021)