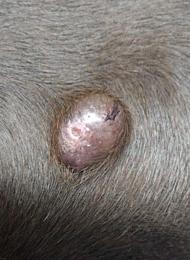
You do not usually start thinking about lymphoma because you want to. It comes up when you notice a few small changes that do not quite fit, a dog who seems a bit quieter on walks, a lump you find while patting them, a tummy that will not settle, or weight loss that feels out of proportion to what they are eating.
A common assumption is that cancer in dogs always looks dramatic or painful. With lymphoma, it can be the opposite at first. Some dogs seem largely themselves, except for painless, enlarged lymph nodes or a slow drift in energy and condition. That is part of what makes it unsettling.
Understanding what lymphoma is, how vets confirm it, and what treatment can realistically do helps you make steadier decisions. It also helps you avoid two extremes that rarely serve dogs well, brushing it off for too long, or panicking before you have a clear diagnosis.
Understanding lymphoma in dogs

Lymphoma (also called lymphosarcoma) is a cancer of lymphocytes, which are cells involved in immune function. Because lymphoid tissue is spread through the body, in lymph nodes, spleen, bone marrow, and other sites, lymphoma is often a whole-body disease rather than a single lump that can simply be removed.1, 2
Many dogs are diagnosed with the multicentric form, where multiple lymph nodes enlarge. Other forms involve the gut, the chest, or specific organs such as skin or eyes. The “type” and how far it has spread (staging) matters, but so does the biology of the cancer, including whether it is B-cell or T-cell lymphoma, and whether it is high grade or low grade.1, 2
Types you will hear your vet mention
- Multicentric lymphoma: typically presents as enlarged peripheral lymph nodes.
- Alimentary (gastrointestinal) lymphoma: affects the intestinal tract, sometimes with chronic vomiting, diarrhoea, appetite change, or weight loss.
- Mediastinal lymphoma: occurs in lymphoid tissue in the chest, can affect breathing.
- Extranodal lymphoma: arises in sites outside lymph nodes, for example skin, eyes, kidneys, or the nervous system.
Causes and risk factors, what is known and what is not
Most families want to know “what caused this”. In truth, lymphoma is rarely linked to one clear trigger. Breed predispositions suggest genetics plays a role in at least some dogs, but genetics is not destiny, and many dogs with lymphoma have no obvious risk factors.2
Environmental exposures are often discussed, but the evidence can be complex and not always conclusive. If you are worried about chemicals around the home or yard, it is reasonable to ask your vet for practical ways to reduce exposure without assuming this is the explanation for a specific diagnosis.
Symptoms people notice first

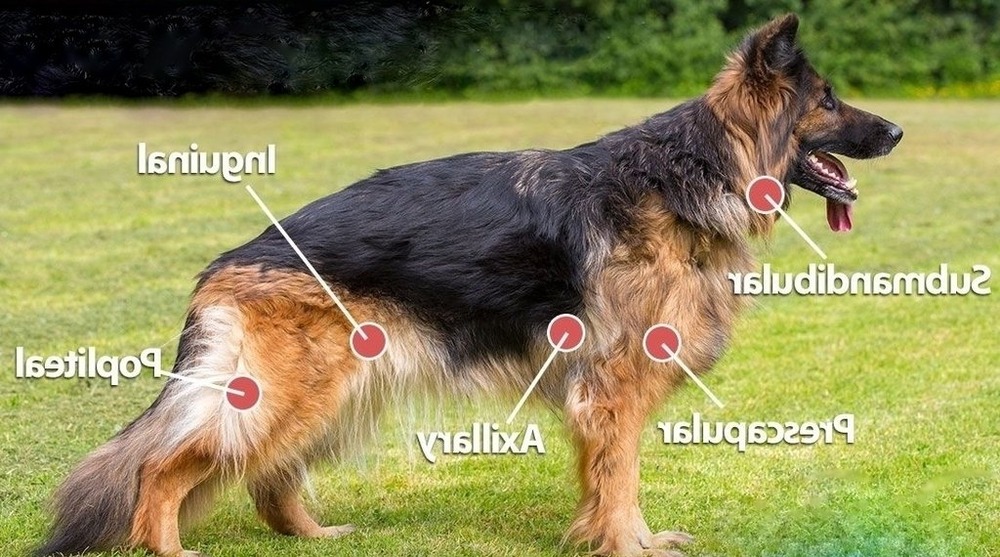
The sign that most often brings lymphoma onto the radar is enlarged lymph nodes. They can feel like firm, rounded, moveable lumps under the skin, commonly under the jaw, in front of the shoulders, in the armpits, in the groin, or behind the knees.1, 2
Other early changes can be subtle: reduced stamina, weight loss, a flatter appetite, or a dog who is “not quite right”. Some dogs drink and urinate more, particularly with certain forms of lymphoma or if they become unwell in other ways.2
How signs can differ by lymphoma location
It helps to keep the pattern in mind, rather than memorising a checklist. Multicentric lymphoma tends to be felt on the outside. Gut lymphoma can look like ongoing digestive trouble. Chest involvement may show up as cough, faster breathing, or exercise intolerance. Extranodal disease depends on the organ involved, for example skin lesions, eye inflammation or cloudiness, or neurological signs in rarer cases.1, 2
If you find a new lump, or several, it is worth booking a vet visit promptly. That does not mean it is definitely lymphoma. Infections and immune reactions can enlarge lymph nodes too, and your vet’s job is to sort out which is which.
How vets diagnose lymphoma
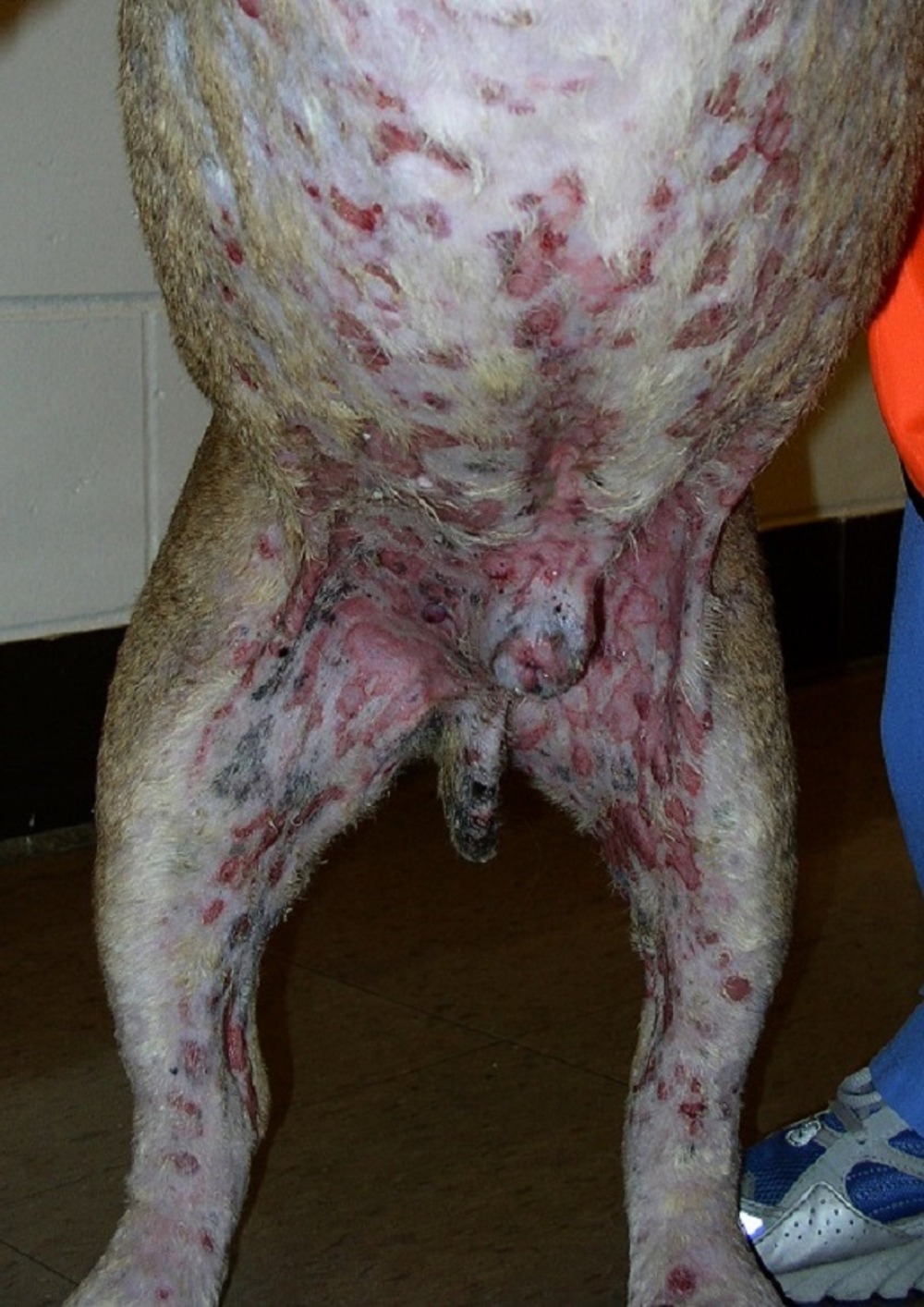
Diagnosis usually starts with a physical exam and a conversation about what you have noticed at home. If lymph nodes are enlarged, many vets will recommend a fine needle aspirate (a small needle used to collect cells for microscope examination). It is quick, commonly done without sedation, and often gives a clear answer for multicentric lymphoma.1
Sometimes a biopsy is needed, particularly if the aspirate is unclear, if the lymphoma is in the gut, or if more detail is needed for planning treatment. Blood tests and imaging (such as ultrasound or chest radiographs) are often used for staging and to assess overall health before therapy.1
Why “staging” and “immunophenotyping” come up
Once lymphoma is confirmed, vets may recommend further tests to determine how widespread it is and what subtype it is. This can include determining whether it is B-cell or T-cell, because that can influence prognosis and help guide expectations.3
Not every family will choose every test, and that is not automatically “wrong”. A thoughtful vet will explain what each test changes in practical terms, including whether it changes the treatment plan, the monitoring plan, or simply helps predict likely outcomes.
Treatment options, and what they are trying to achieve

For many dogs with lymphoma, treatment is about good quality time, not cure. That said, lymphoma is one of the cancers where treatment can often achieve remission, sometimes for many months, and occasionally longer, depending on the dog and the subtype.2, 3
Chemotherapy
Multi-drug chemotherapy protocols (often doxorubicin-based, such as CHOP-style protocols) are considered standard of care for many dogs with high-grade multicentric lymphoma. Published reviews report median remission durations around 7 to 10 months and median survival around 10 to 14 months for many dogs treated with these protocols, acknowledging that individual outcomes vary widely.3
One detail that reassures many people is that veterinary chemotherapy is typically dosed with the goal of maintaining quality of life. Dogs often tolerate it better than people expect, though side effects can occur, including reduced appetite, vomiting, diarrhoea, and lowered white blood cell counts.4
Steroids (prednisolone) and simpler protocols
Some families choose less intensive approaches, whether due to cost, travel, the dog’s temperament, or other health issues. Steroids may improve comfort and appetite for a time, and can shrink lymph nodes temporarily, but they are generally not a long-term solution on their own for high-grade lymphoma.2
If you are considering chemotherapy later, ask your vet before starting steroids, because steroid treatment can sometimes reduce the ability of some chemotherapy drugs to work as well afterwards (this depends on the situation and the protocol).
Radiation and surgery
Radiation therapy can be useful for localised disease or for symptom relief in certain cases. Surgery is less common for lymphoma because it is often systemic, but it can play a role in specific extranodal presentations or to obtain diagnostic tissue, depending on where the cancer is located.1
How treatment decisions are usually made
A good treatment plan is not just “what is available”, it is what suits the dog in front of you. Vets will often weigh up:
- type and grade of lymphoma
- stage and whether the dog feels well or unwell (often described as substage)
- other medical conditions and medications
- the family’s capacity for visits, monitoring, and costs
If you feel stuck, it can help to ask one practical question: “What will life look like for my dog, week to week, on this plan?” It brings the focus back to the dog’s actual day-to-day experience.
Prognosis and life expectancy
Prognosis in canine lymphoma is variable, and it is easy to get lost in averages. The most useful framing is often: what is typical, what factors make outcomes better or worse, and what range is plausible.
Without treatment, high-grade lymphoma is often fast moving. One university veterinary oncology service notes that dogs with high-grade lymphoma without treatment usually live around four to six weeks, while dogs treated with multi-drug chemotherapy have a median survival around one year, with a proportion living to two years.5
Response to chemotherapy is one of the strongest practical indicators. Dogs who achieve complete remission tend to live longer than those with partial or no remission in published studies, although outcomes still vary between individuals and subtypes.6
What changes the outlook
Prognosis is influenced by several interacting factors, including stage, immunophenotype (B-cell vs T-cell), tumour grade, and how well the lymphoma responds to treatment.3
It is also worth remembering that “prognosis” is not only about length of life. It includes how a dog feels during that time, and how smoothly side effects can be prevented or managed.
Caring for a dog living with lymphoma
Life with lymphoma often becomes a rhythm of ordinary days and vet days. Many dogs still want their usual comforts, familiar routes, favourite people, and time in the sun. You can support that normality while also keeping an eye on symptoms and treatment effects.
Monitoring at home, without over-watching
Keep notes if it helps you think clearly, but aim for calm observation rather than constant checking. Useful things to track include appetite, stools, energy on walks, willingness to play, and whether lymph nodes are changing in size.
If your dog is on chemotherapy, ask your vet what to do if vomiting, diarrhoea, or appetite loss occurs. Supportive care can make a big difference, and veterinary guidelines emphasise planning for common side effects such as nausea, diarrhoea, and reduced appetite, rather than waiting until a dog is already struggling.4
When to ring the vet the same day
- Repeated vomiting or inability to keep water down
- Watery or bloody diarrhoea
- marked lethargy, collapse, or weakness
- laboured breathing or sudden cough
- fever, or if your dog feels hot and unwell after chemotherapy
Your clinic may also give you specific thresholds based on your dog’s treatment plan and blood test results. If in doubt, ring and ask. That is part of the job, and most issues are easier to manage early.
Prevention, and the reality of current research
There is no proven way to prevent lymphoma in dogs. That can be frustrating, particularly for people who take great care with diet, exercise, and the home environment.
What you can do, and what is sensible even without perfect evidence, is focus on reducing avoidable exposures, maintaining a healthy weight and activity level, and seeing your vet when something changes rather than waiting for it to pass. Research is also active in improving treatment, monitoring remission, and developing newer approaches, including work at major veterinary centres investigating lymphoma biology and response to therapy.7
If your dog is diagnosed, ask whether clinical trials are an option. Trials are not suitable for every family, but they can provide access to new therapies and help improve care for future dogs.8
Final thoughts
Lymphoma is a heavy diagnosis to carry, but it is not the same as “nothing can be done”. For many dogs, there is a middle path between aggressive treatment at all costs and doing nothing. It is a path built around comfort, function, and the particular dog you know best.
If you take one practical step from all of this, let it be this: when you notice new, persistent lumps or a cluster of changes that do not add up, book the appointment and ask for clarity. Having real information in front of you makes the next decisions steadier, and kinder.
References
- Merck Veterinary Manual: Malignant Lymphoma in Dogs
- Cornell University College of Veterinary Medicine: Oncology service information (includes lymphoma overview and survival estimates)
- PubMed: Canine lymphoma, a review (standard protocols, remission and survival ranges)
- AAHA: 2026 Oncology Guidelines (Supportive and Symptomatic Care)
- Cornell University College of Veterinary Medicine: Lymphoma without treatment and median survival with multi-drug chemotherapy
- PMC: Clinical outcome of multicentric lymphoma treated with CHOP (response categories and survival)
- Purdue University College of Veterinary Medicine: Canine lymphoma research and chemotherapy response information
- Cornell University College of Veterinary Medicine: Clinical trials for dogs with lymphoma