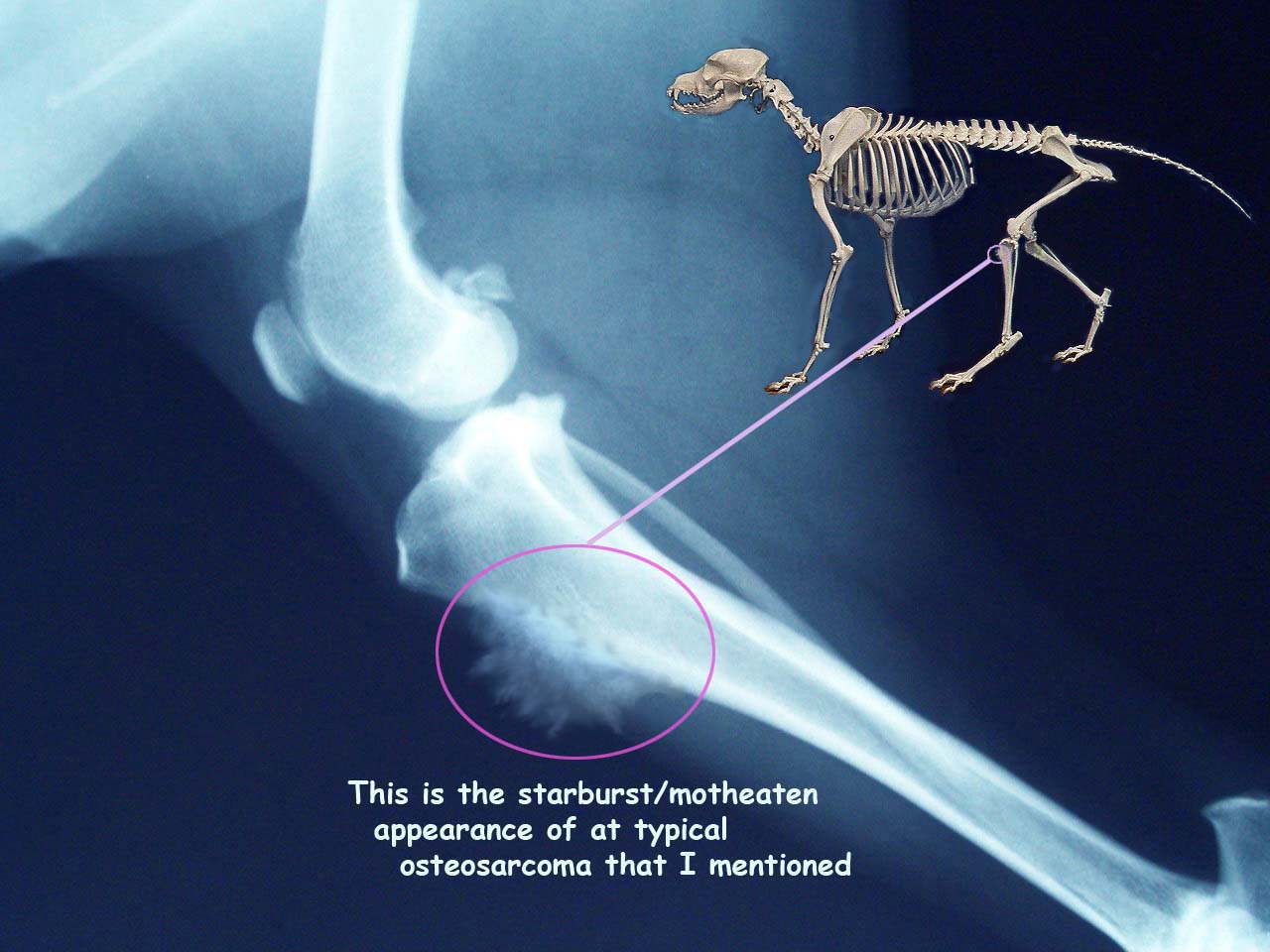
You might first notice it as a limp that does not quite add up. Your dog still wants to come along, still eats, still greets you at the door, but one leg is suddenly “off”. Sometimes there is a small swelling, or your dog looks stiff after resting. It is easy to assume it is a sprain, arthritis, or a pulled muscle, especially in a big, active dog.
Osteosarcoma often enters the picture in exactly these ordinary moments. It is a cancer of the bone that can cause significant pain early on, even when the outward signs seem mild. The practical challenge is that the first signs overlap with many far more common problems, and waiting for it to “settle” can mean losing valuable time.
Getting clear information helps you make calmer decisions, whether that means booking an x-ray, asking for a referral, or simply understanding what your vet is looking for and why. The aim is not to panic, but to recognise patterns that deserve a closer look.
Understanding osteosarcoma in dogs

Osteosarcoma is the most common primary malignant bone tumour in dogs, and it tends to behave aggressively.1, 2 Most cases involve the long bones of the limbs (called appendicular osteosarcoma), although it can also occur in the jaw, ribs, pelvis, or spine.2
Large and giant breeds are over-represented, with an average age of onset often around the senior years, although a smaller, earlier peak has also been reported in young adult dogs.2 That does not mean smaller dogs are “safe”, only that the probability shifts with size, breed background, and life stage.
One reason osteosarcoma is taken so seriously is its tendency to spread, most commonly to the lungs. Even when chest x-rays look clear, microscopic spread can already be present.2, 3 This is why treatment plans often combine local control of the painful bone tumour with therapies aimed at slowing metastasis.
Signs that warrant a closer look
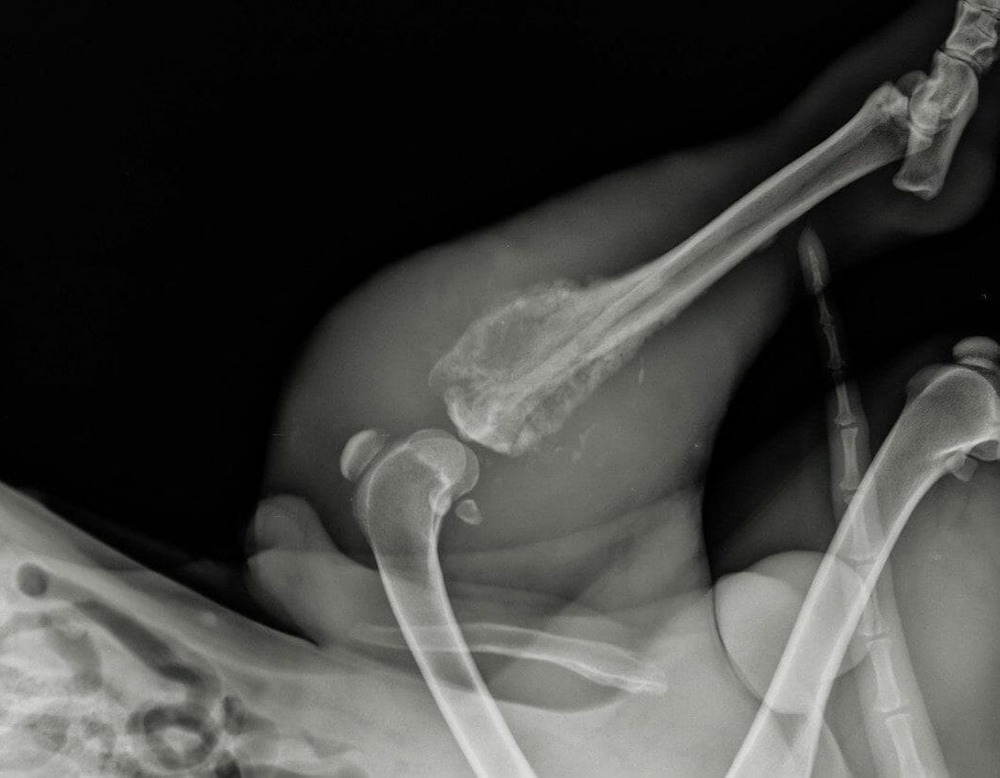
Dogs rarely present with a neat, obvious “cancer” picture. More often, you see a set of changes that persist or slowly intensify. Persistent lameness is the classic starting point, sometimes linked to mild trauma that seems out of proportion to the ongoing pain.2
Other common signs include swelling over a bone, sensitivity when the area is touched, and reluctance to run, jump, or use stairs. In some cases, a pathological fracture can occur, meaning the bone breaks with minimal force because it has been weakened by the tumour.1
- Limping that does not improve over days to a couple of weeks, or that keeps returning
- Firm swelling near the shoulder, wrist, knee, or hip
- Noticeable pain when getting up, turning, or bearing weight
- A sudden, severe lameness that could indicate a fracture
None of these signs confirm osteosarcoma on their own. They are simply good reasons to move from watchful waiting to proper assessment.
How osteosarcoma is diagnosed and staged
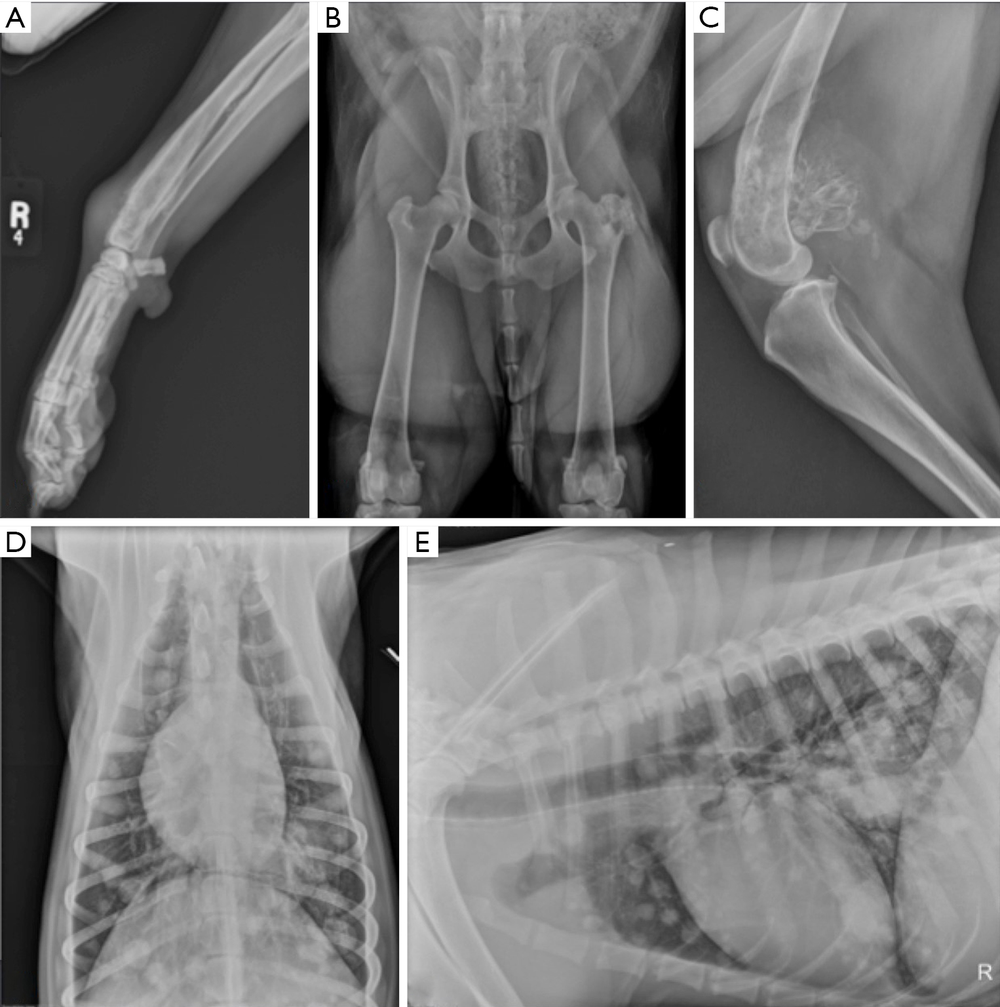
Most work-ups start with a physical exam and orthopaedic x-rays of the affected limb. Radiographs can show patterns of bone destruction and new bone formation that raise strong suspicion for a bone tumour.1
Because infections and some other conditions can occasionally mimic parts of this picture, confirmation commonly involves collecting a sample from the lesion. A bone biopsy is one accepted way to do this, and your vet may recommend referral so it can be done as safely and accurately as possible.1, 2
Staging is about looking beyond the painful bone to understand what else might be happening in the body. This usually includes imaging of the chest because the lungs are a common site of metastasis, plus additional tests depending on the dog and the planned treatment pathway.1, 2
Treatment options and what they are trying to achieve

In practice, treatment discussions usually revolve around two goals: pain control at the primary site and slowing or delaying spread.2 The right plan depends on where the tumour is, your dog’s overall health, and what is feasible for your household.
Surgery (often amputation, sometimes limb-sparing)
For limb tumours, amputation is commonly recommended because it removes the main source of pain and the primary tumour burden. It can feel like an enormous step, but many dogs adapt surprisingly well, especially when pain is well-managed and rehabilitation is supported.2
In selected cases, limb-sparing surgery may be an option, typically through specialist centres. This approach aims to remove the tumour while preserving the limb, but it comes with its own risks, costs, and aftercare demands.4
Chemotherapy
Chemotherapy is often used after surgery to address likely microscopic metastatic disease. In broad terms, dogs that have surgery plus chemotherapy tend to have longer median survival times than dogs that have surgery alone, although individual outcomes vary.2, 3
Veterinary chemotherapy is usually planned with quality of life in mind. Side effects can still happen, but many dogs tolerate protocols better than people expect when they first hear the word “chemo”.2
Radiation therapy and other palliative options
Radiation can be used for pain relief, particularly when surgery is not an option, or when the tumour is in a location where complete removal is difficult. Palliative protocols focus on comfort and function rather than cure.1, 2
Some dogs may also benefit from additional pain-relief strategies provided by specialists, including multimodal medication plans and, in some cases, treatments such as bisphosphonates as part of a palliative approach.2
Prognosis, in real-world terms
Prognosis is best thought of as a range, not a promise. It is shaped by factors such as metastatic status, tumour location, overall health, and how well pain can be controlled.
Published figures vary, but a commonly cited pattern is that median survival can be only a few months with amputation alone, and often longer when chemotherapy is added. Some dogs live substantially longer than the medians, while others have a shorter course despite treatment.1, 2, 3
It is also worth knowing that many dogs have metastatic disease at diagnosis at a microscopic level, even if imaging does not show obvious spread. That reality can help explain why vets recommend combined treatment, and why follow-up matters even when the primary leg pain has improved.2, 3
Managing pain and protecting quality of life

Even before you have all the answers, pain relief matters. Bone pain can be severe, and dogs can be stoic. Effective pain management is usually multimodal, meaning different medications and strategies are combined to target pain from multiple angles.1, 2
Simple home adjustments often make day-to-day life easier. Soft, supportive bedding, rugs for traction, and ramps for steps can reduce slips and awkward movements. Gentle, consistent routines can also help, especially if your dog is learning to move differently after surgery.
Regular rechecks give your vet the chance to adjust medication, monitor for complications, and talk through changes you are noticing at home. If something feels “off”, it is reasonable to ask whether referral to a veterinary oncologist or surgeon could add useful options or clarity.2, 5
Risk, prevention, and what you can and cannot control

There is no proven way to prevent osteosarcoma in the general dog population. Breed and body size are associated risk factors, and certain breeds are reported more often in clinical settings, but that does not translate into a simple prevention plan.2
What you can control is the speed and quality of your response when something changes. If you have a large-breed dog and you are seeing a limp that persists, especially with swelling over a bone, it is sensible to move quickly to diagnostic imaging rather than repeatedly resting and retrying exercise.
Keeping dogs at a healthy weight and maintaining appropriate fitness supports joints and mobility in general, which can make it easier to notice when a problem is not “just stiffness”. It does not remove cancer risk, but it can reduce the background noise that sometimes masks early signs.
Support for owners making hard decisions
An osteosarcoma diagnosis often brings practical and emotional decisions close together. Treatment can be time-consuming and expensive, and it can involve choices that feel confronting, such as amputation. It helps to talk openly with your vet about what matters most to your household and what a good day looks like for your dog.
If you are weighing palliative care, it can help to ask for a clear plan: what medications are available, what changes should prompt a review, and how you will recognise when comfort is slipping. Good palliative care is still active care, and many dogs can have meaningful, comfortable time with the right support.1, 2
Owner support can also come from veterinary oncology services and established animal cancer organisations, which often provide plain-language explanations and questions to take to your next appointment.5, 6
References
- Merck Veterinary Manual: Bone Tumors in Dogs and Cats
- Cornell University College of Veterinary Medicine: Canine Osteosarcoma (Oncology service information)
- PubMed: Canine osteosarcoma, amputation and chemoimmunotherapy (review)
- PubMed: Outcome and prognostic factors in dogs living greater than one year after osteosarcoma diagnosis
- American Veterinary Medical Association (AVMA): Cancer in dogs
- American College of Veterinary Surgeons (ACVS): Osteosarcoma
- dvm360: Current treatment options for dogs with appendicular osteosarcoma
- PubMed Central: Adjuvant chemotherapy and survival in dogs undergoing amputation for appendicular osteosarcoma
- UC Davis: Osteosarcoma in dogs (health and behaviour education)