Most people do not start by wondering about a dog’s urinary tract. They notice a change instead: a dog asking to go out again and again, taking longer to wee, leaving tiny puddles indoors, or looking uncomfortable in a way that is hard to place.
It is tempting to assume it is behavioural, or that it will pass on its own. Sometimes it does. But urinary signs are one of those everyday problems that can sit on a spectrum, from mild irritation to infection, stones, or a blockage that becomes urgent quite quickly.
Understanding what sits underneath these signs matters because the right response is often practical and simple, and the wrong one can mean delayed care or repeated flare-ups. The goal is not to panic, it is to recognise patterns early and work with your vet to keep your dog comfortable and safe.
Common types of urinary tract disorders in dogs
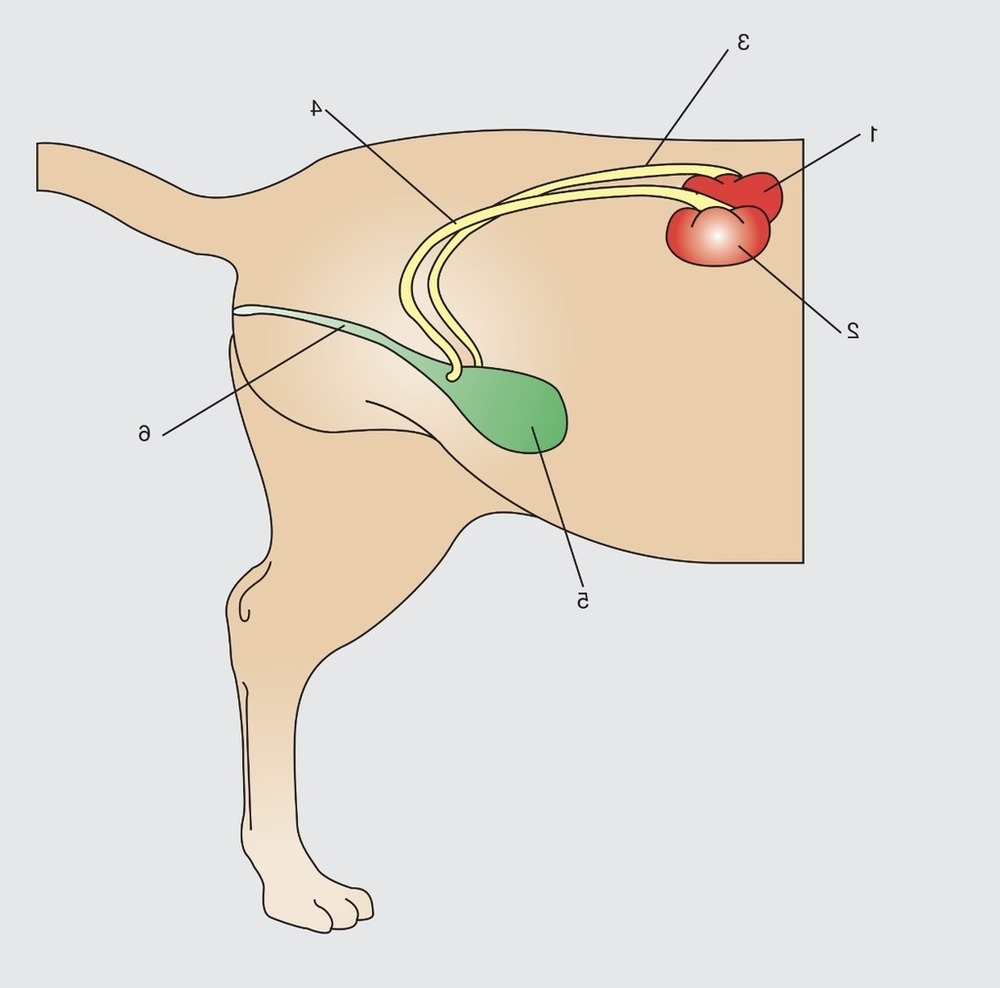
Urinary problems in dogs are often grouped together, but they are not all the same. A dog that strains to pass urine could have inflammation in the bladder, a bacterial infection, a stone rubbing the bladder wall, or a physical obstruction. Some conditions overlap, so the label matters less than the underlying cause.
Urinary tract infections (UTIs) and bacterial cystitis
A true lower urinary tract infection usually means bacteria have established in the bladder (often called bacterial cystitis). Signs commonly include urinating more often, straining, discomfort while weeing, blood in the urine, and sometimes toileting in unusual places.1
It is also worth knowing that not every dog with urinary signs has a bacterial infection. Your vet may recommend tests before antibiotics, especially if the problem is recurring.2
Bladder stones (uroliths)
Bladder stones can cause the same outward signs as an infection, particularly blood in the urine and straining. Stones may be visible on imaging such as X-rays or ultrasound, and management can include diet, minimally invasive removal, or surgery depending on stone type, size, and risk of obstruction.3, 4
Incontinence and related disorders
Incontinence is urine leakage rather than difficulty passing urine. It can be associated with hormone-responsive urethral sphincter mechanism incompetence, age-related changes, urinary tract infection, spinal or neurological disease, and a range of other conditions. It is easy to dismiss as a “getting older” issue, but it is often treatable once the cause is identified.
Symptoms to watch for
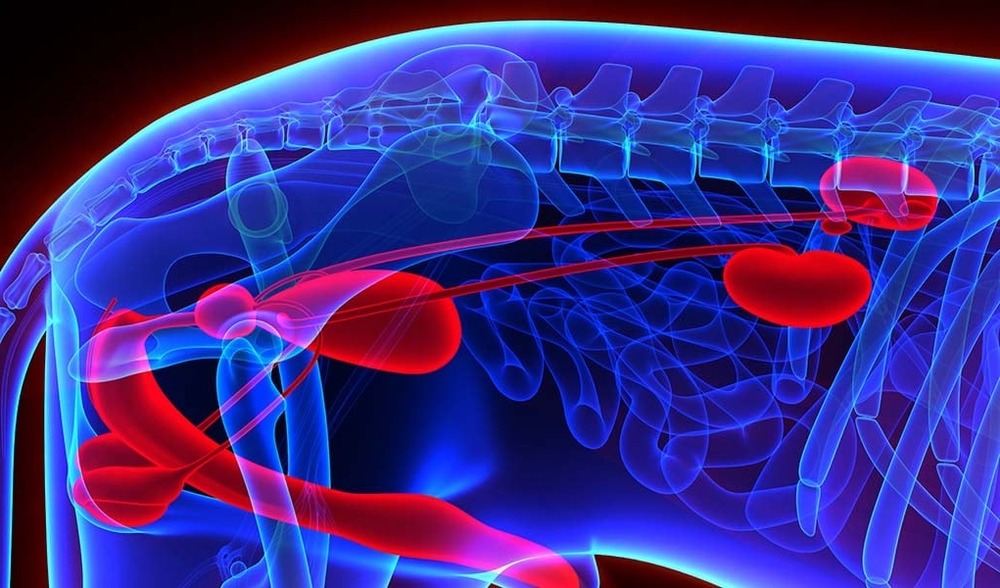
Urinary signs can look small at first, especially if a dog is still eating and acting mostly normal. The pattern is often the clue: little changes that repeat across a day or two, or that keep returning every few weeks.
Common signs
- Frequent urination, especially with small amounts each time1
- Straining, discomfort, or taking longer to pass urine1
- Blood-tinged urine, or blood more noticeable at the end of the stream1
- Accidents indoors in a previously toilet-trained dog1
- Increased licking around the genital area (not specific, but can appear with irritation)1
Behaviour changes that can signal discomfort
Some dogs become restless and ask to go out repeatedly. Others slow down on walks, seem reluctant to squat, or choose unusual places to wee. These changes do not prove pain or infection on their own, but they do suggest your dog is responding to something different in their body.
Why early attention helps
Early assessment can prevent a simple problem becoming complicated, and it can reduce the chance of repeated flare-ups. It also helps avoid unnecessary treatment. For example, urine culture is often used to confirm bacterial infection and guide antibiotic choice, rather than guessing.2
Causes and risk factors
Urinary disorders tend to have contributing factors rather than a single neat cause. Some are anatomical, some are metabolic, and some are about what is happening in a dog’s wider health.
Underlying causes
Lower urinary tract signs can be associated with bacterial infection, bladder stones, inflammation that is not primarily bacterial, and (less commonly) tumours or structural problems. Some systemic diseases can increase risk, including diabetes mellitus and hyperadrenocorticism (Cushing’s disease).5
Breed and body factors
Stone risk is influenced by genetics, urine chemistry, and anatomy. Sex also plays a part in practical risk, particularly because male dogs have a narrower urethra, which can make obstruction more likely if stones or grit move into the urethra.3
Environment and daily life
Hydration and toileting routine matter. Dogs that drink less, are fed only dry food, or “hold on” for long periods can be more prone to concentrated urine, which may contribute to crystal and stone formation in susceptible dogs. In real life, this often shows up in busy households where walks are shorter than usual, or where a dog is less keen to drink in hot or stressful periods.
Diagnosis and veterinary care

Urinary problems are a good example of why veterinary work is often detective work. The same sign, like straining, can sit on top of very different conditions. Diagnosis is about matching history, exam findings, urine testing, and imaging to what is actually going on.
What your vet may recommend
A typical work-up may include a physical exam, urinalysis, and a urine culture if infection is suspected. A quantitative urine culture is widely regarded as the best way to confirm bacterial cystitis and to guide antibiotic choice.2
If stones, anatomical issues, or upper urinary tract disease are on the list, your vet may recommend imaging such as X-rays or ultrasound, since many stones can be identified that way (and some require ultrasound or contrast studies).3
Why “just in case” antibiotics are not always ideal
In day-to-day practice, the urge to treat quickly is understandable. But antimicrobial stewardship matters. Guidelines and consensus statements emphasise using culture and clinical judgement to support appropriate antibiotic use, partly to reduce unnecessary exposure and antimicrobial resistance risk.6
Monitoring and follow-up
Follow-up is not only for complicated cases. Some stone types recur, and some dogs benefit from periodic checks so problems are found when they are smaller and easier to manage. In dogs with calcium oxalate stones, for example, recurrence is common and medical dissolution is not an option, so monitoring and prevention become central parts of care.7, 8
Treatment options

Treatment depends on the cause, and sometimes treatment has two tracks: relieving current discomfort and reducing the chance of recurrence. Your vet will tailor recommendations to your dog’s age, sex, history, test results, and any other health conditions.
Medications
If a bacterial infection is confirmed or strongly suspected, antibiotics may be prescribed and adjusted based on culture results. Pain relief can also be important, because urinary inflammation can be uncomfortable even when the dog is still trying to act normal.2
Stone management and procedures
For bladder stones, options may include dietary dissolution for certain stone types, minimally invasive techniques, or surgery. Current consensus recommendations generally favour minimally invasive removal when suitable, because it can reduce hospital time and recovery burden for many dogs.4
Diet and hydration as part of the plan
Diet changes are not a generic “urinary diet for everyone” solution. They are chosen based on stone type and urine chemistry goals. For calcium oxalate uroliths, guidance often focuses on increasing urine dilution, sometimes with a higher moisture diet, alongside targeted nutritional management.8
Prevention strategies that fit real life
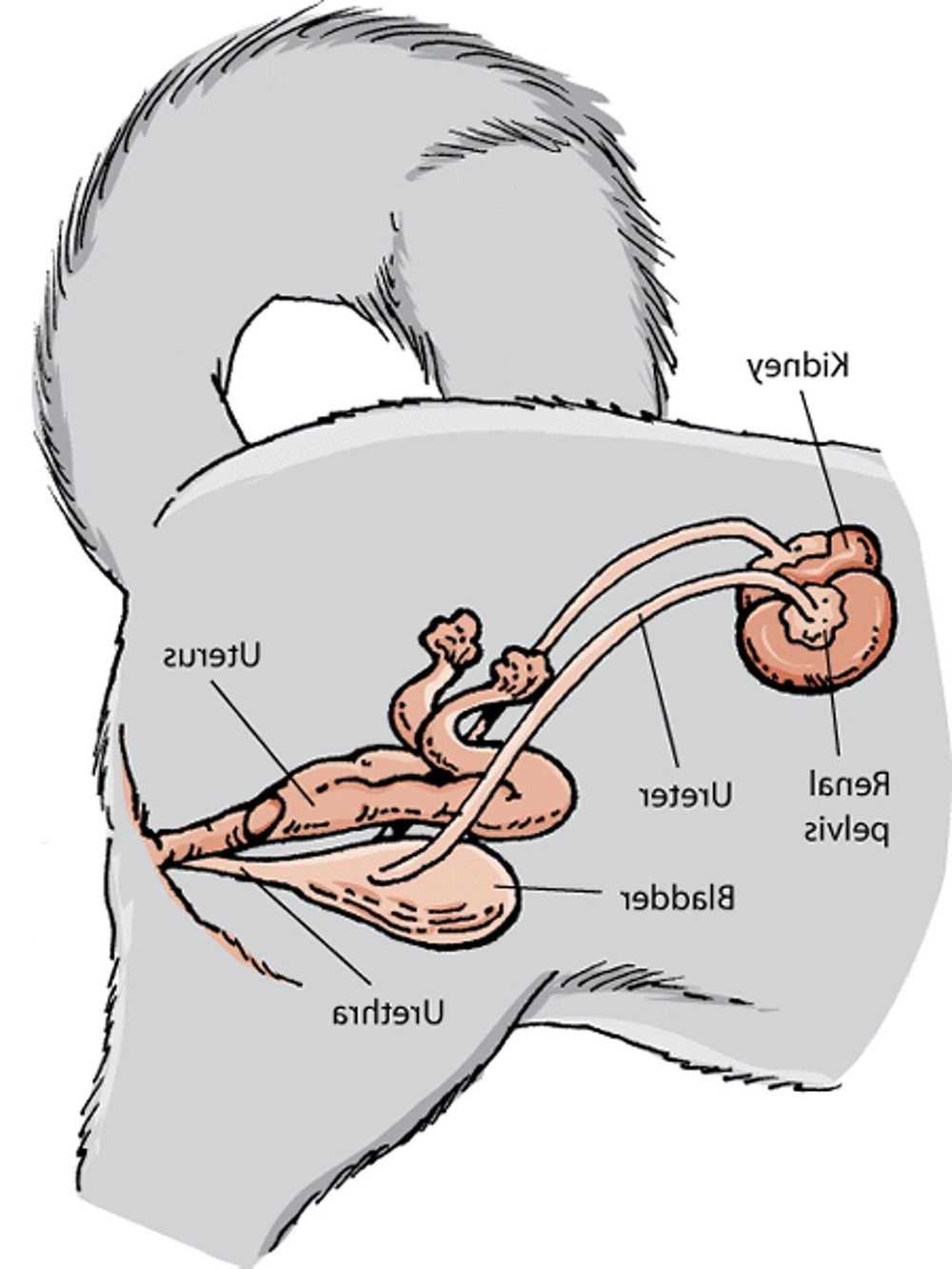
Prevention is rarely about perfection. It is about small routines that make urinary health easier on a dog’s body, and easier for you to notice when something changes.
Practical habits that help
- Keep water accessible and appealing, and consider additional water bowls in the places your dog actually rests.
- Offer more toilet opportunities, especially for dogs that spend long stretches indoors.
- If your dog has a history of stones or UTIs, follow your vet’s plan for rechecks and monitoring.
Weight, movement, and stress
Regular gentle exercise helps many systems, including bladder function and routine toileting. Weight management also matters, not as a judgement, but because it can influence mobility, posture for urination, and general health resilience.
When to seek immediate veterinary attention
Some urinary signs can wait for a routine appointment. Others should not. The most important red flag is a dog that cannot pass urine at all, or is producing only drops while repeatedly attempting.
Urgent signs
- Inability to urinate, or repeated straining with no urine produced3, 9
- Marked abdominal swelling or obvious distress
- Weakness, collapse, vomiting, or rapidly worsening condition
Why speed matters
A complete urinary obstruction is a medical emergency. It can lead to dangerous electrolyte changes and severe systemic illness. If you suspect obstruction, treat it as urgent and contact an emergency vet clinic immediately.3
Final thoughts on supporting urinary health
Urinary tract disorders are common enough that many dog owners encounter them at least once. The most useful mindset is steady observation: notice changes, take patterns seriously, and be open to testing that clarifies the cause rather than guessing.
With a good plan, many dogs do very well, even if they are prone to infections or stones. A little attention to hydration, toileting routine, and follow-up can make urinary health feel less like a recurring mystery and more like something manageable.
References
- Merck Veterinary Manual (Dog Owners): Infectious diseases of the urinary system in dogs
- Merck Veterinary Manual: Bacterial cystitis in small animals
- VCA Animal Hospitals: Bladder stones in dogs
- Journal of Veterinary Internal Medicine (ACVIM): Small Animal Consensus Recommendations on the Treatment and Prevention of Uroliths in Dogs and Cats
- Merck Veterinary Manual (Dog Owners): Risk factors and presentation of bladder infection in dogs
- Journal of Veterinary Internal Medicine (ACVIM): Consensus Statement on Therapeutic Antimicrobial Use in Animals and Antimicrobial Resistance
- University of Minnesota Urolith Center: Managing dogs with asymptomatic calcium oxalate bladder or urethral stones
- MSD Veterinary Manual: Urolithiasis in dogs
- PDSA: Urine and bladder problems in dogs

